Personalized interventions can improve colorectal cancer screening rates in primary care practices considerably.
A new study at the Jefferson Medical College in Philadelphia shows that to encourage to get screened for colorectal cancer, a personalized approach can go a long way. These personalized interventions can improve colorectal cancer screening rates in primary care practices considerably.
Ronald Myers, Ph.D., professor of medical oncology at Jefferson Medical College of Thomas Jefferson University and his co-workers divided 1,546 at-risk primary care patients who were not up-to-date on colon cancer screening into four groups. They randomly assigned patients to receive one of the following: usual care (control); mailed information, screening materials and a mailed reminder (group one); mailed information with messages addressing personal concerns about screening, screening materials, and a mailed reminder (group two); or mailed information with personal messages, screening materials, plus mail and telephone reminders (group three).The team, reporting online September 24, 2007 in the journal CANCER, found that compared to usual care controls, all of the personalized approaches made a difference. Two years after the study began, screening rates were higher in each intervention group compared to the control group. Only 33 percent of individuals in the control group were screened, compared to 48 percent in group three, 46 percent in group two and 44 percent in group one.
“We found that we can get a substantial increase in screening by taking a personalized approach in which the at-risk population is identified and then offered screening and information,” Dr. Myers says. “More than 40 percent responded and were screened. By adding in the personal messages that addressed personal barriers to screening, such as concerns about test inconvenience and discomfort, we were able to see additional, modest improvements.”
According to Dr. Myers, the number of individuals going for colon cancer screening in primary care practices has traditionally been low. His team and others have been trying to find new ways to raise screening rates. But it has been difficult. “The key to addressing this important public health problem is to apply a relatively simple, low-cost approach that not only increases screening use, but is also cost-effective,” Dr. Myers says. His team showed “the potential impact that can be achieved when such an intervention strategy can be delivered to patients in primary care practice settings. In fact, if personalized interventions were delivered as an ancillary service to primary practices, we could increase screening rates substantially, and as a result, reduce the burden of colorectal cancer dramatically.”
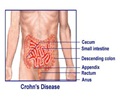
Colorectal cancer is the third most common cancer and third leading cause of cancer death in this country. Yet, when found early, the disease can be prevented or easily treated. Generally, recommendations include fecal blood testing every one to two years after age 50, a flexible sigmoidoscopy every five years and a colonoscopy every ten years.
Source-Eurekalert
GAN /J
 MEDINDIA
MEDINDIA
 Email
Email