Two regions of the genome (loci) associated with ulcerative colitis only in people of African descent have been identified by researchers.
TOP INSIGHT
Two regions of the genome (loci) associated with ulcerative colitis only in people of African descent have been identified by researchers.
The study was led by Emory University, the Johns Hopkins University School of Medicine, and Cedars-Sinai and is published online in the journal Gastroenterology.
In more than 1,000 studies of IBD genetics in white and Asian populations, more than 200 susceptibility loci for IBD have been identified in populations of predominantly European ancestry, and at least 35 loci have been identified in Asians, with a few that appear to be Asian-specific.
The research team hypothesized that a high-density GWAS of IBD in African-Americans could identify population-specific variants, further define IBD genetic architecture, and expose novel disease mechanisms.
"Although most human gene mapping has been done in people of European background, inflammatory bowel disease is not race-specific," says Subra Kugathasan, professor of pediatrics at Emory University School of Medicine and corresponding author of the study. "Genome-wide studies lag behind in non-European populations, and African-Americans are the last group not to be studied specifically. As new therapies are developed, it will be important to know the genotype of individuals we are treating."
The study identified single-nucleotide polymorphisms (SNPs) - at ZNF649 and at LSAMP - with genome-wide significance in ulcerative colitis. These SNPs are very specific to sub-Saharan Africans and are not found in any other populations - making these findings unique and novel. This is the first time African- specific loci are known to contribute to IBD, and these loci will be added to the already known 200+ loci in IBD to further expand the IBD genetic architecture. The team also found evidence of overlapping genome-wide associations for ulcerative colitis and IBD in African- Americans and other populations.
The study's first author was Steven Brant, director of the Johns Hopkins Meyerhoff Inflammatory Bowel Disease Center. In addition to Brant, Kugathasan and McGovern, the study was authored by 40 other physicians and researchers in the United States and Canada.
"The detection of variants associated with IBD risk in only people of African descent demonstrates the importance of studying the genetics of IBD and other complex diseases in populations beyond those of European ancestry," say the authors.
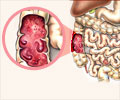
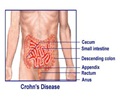
In a previous study using the Immunochip genotyping platform, and also published in Gastroenterology, the research team had evaluated more than 1,500 African-American patients with IBD - including 1,088 with Crohn's disease and 361 with ulcerative colitis - from 35 IBD centers across North America and used 1,797 African-Americans without IBD for comparison. They found that gene variants within three of the most highly associated regions for Crohn's disease in whites - NOD2, interleukin 23 receptor (IL23R) and a region on chromosome 5 known as 5p15.1 - are also important risk factors for Crohn's disease in African-Americans.
The authors summarize: "This first GWAS of AA IBD has demonstrated unique, African specific loci, as well as loci that are shared across multiple populations. While some of these shared loci contain unique association patterns and African specific risk variants, many contain universal risk variants (like HLA-DRB1) or risk variants that have arisen from European admixture (like NOD2).
"Given our results and the evolution of IBD genetics research in non-European populations, it is clear that further studies with larger sample sizes in the AA population are needed to identify additional population specific variants and novel loci, as well as more fully characterize the role of risk variants established in other populations on the development of IBD in AAs. Such research is paramount to allow for the future benefits of IBD genetics research, from risk prediction and family counseling to targeted therapies and eventually disease preventive strategies to be available for the under-studied AA population."
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email