Globally more than one in ten babies are born prematurely, and this can be explained better by a new device which could lead to better treatments and prevention options for preterm labor resulting from bacterial infections.
TOP INSIGHT
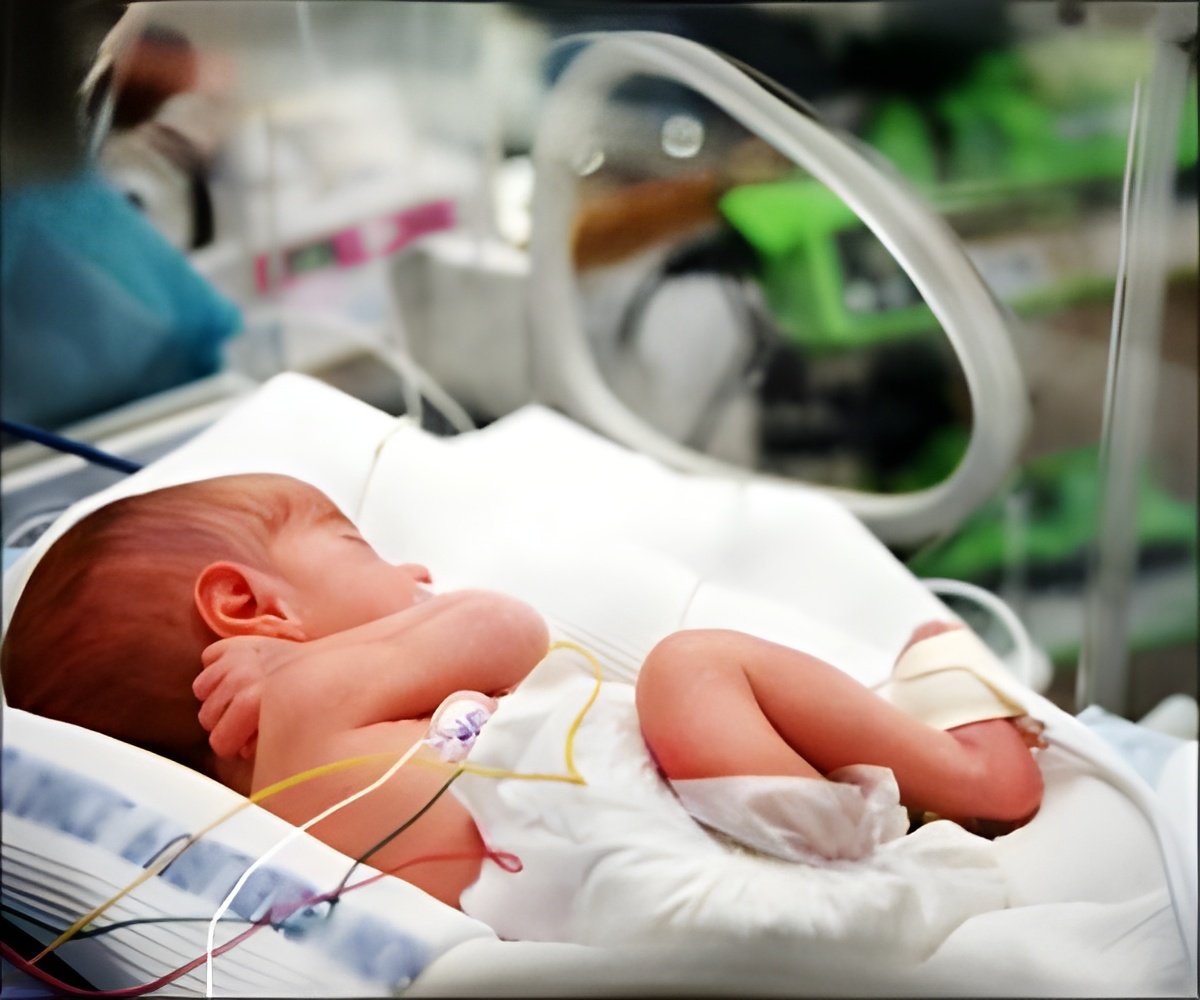
Placental barriers-on-a-chip could lead to better treatments and prevention options for preterm labor resulting from bacterial infections.
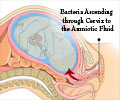
As a result, the amniotic sac can rupture, producing early-onset labor. Studying this problem has proven tricky, in part because it's not feasible to run clinical trials including pregnant women, and human placentas donated after birth can only survive a few hours.
However, researchers recently created a placenta-on-a chip a promising new microfluidic device that allows placental cells to grow and function as if they were still in the body. Delving deeper, Jianhua Qin and colleagues sought to create a similar device that would specifically replicate the functions of the placental barrier and how it responds to bacterial infection.
The researchers implanted human trophoblasts (representing the mother's cells) and endothelial cells (representing the fetus) from a human umbilical cord vein onto opposite sides of a three-layer microfluidic device.
A porous membrane between the two cell layers allowed the tissues to form a placental barrier between them. After determining that the barrier was functioning much as it would in the body, the researchers added E. coli bacteria to the maternal layer. The bacteria proliferated rapidly, breached the placental barrier, and subsequently triggered inflammation and cell death in both of the adjoining maternal and fetal layers.
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email



