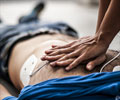
The study revealed that a pharmacological blockade of the brain's electrical connections to the heart during cardiac arrest may improve the chances of survival.

"Despite the absence of signs of life, internally the brain exhibits sustained, organized activity and increased communication with the heart, which one may guess is an effort to save the heart," said Dr. Jimo Borjigin, senior study author, associate professor of neurology.
However the brain signaling at near-death may, in fact, accelerate cardiac demise. To understand this, the researchers looked at the mechanism by which the heart of a healthy person ceases to function within just a few minutes without oxygen.
They simultaneously examined the heart and brain during experimental asphyxiation and documented an immediate release of more than a dozen neurochemicals, along with an activation of brain-heart connectivity. Following a steep fall of the heart rate, brain signals strongly synchronized with the heart rhythm, as visualized beat-by-beat using a new technology developed in the Borjigin laboratory called electrocardiomatrix.
According to the study, blocking the brain’s outflow significantly delayed ventricular fibrillation, in which the lower chambers of the heart quiver and the heart cannot pump any blood. It is the most serious cardiac rhythm disturbance.
"The study suggests that a pharmacological blockade of the brain’s electrical connections to the heart during cardiac arrest may improve the chances of survival in cardiac arrest patients," Borjigin said.
Source-IANS
 MEDINDIA
MEDINDIA


 Email
Email