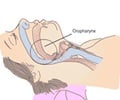
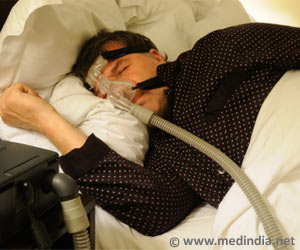
Obstructive sleep apnea (OSA) is associated with subclinical myocardial injury, say researchers.

The findings were published online ahead of print publication in the American Thoracic Society's American Journal of Respiratory and Critical Care Medicine.
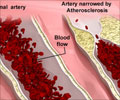
The study included 1,645 middle-aged and older participants in both the Atherosclerosis Risk in Communities and the Sleep Health Study who were free of CHD and HF at baseline. All subjects underwent overnight home polysomnography. Median follow-up was 12.4 years. OSA severity was categorized as none, mild, moderate, or severe using the respiratory disturbance index.
Hs-TnT levels, but not N terminal pro B-type natriuretic peptide levels (a marker for increased ventricular wall stress), were significantly associated with OSA after adjustment for 17 potential confounders (p=0.02), including age, gender, body mass index, smoking status, hypertension, diabetes, alcohol intake, pulmonary function variables (FEV1 and FVC), COPD status, systolic blood pressure, total cholesterol, LDL cholesterol, HDL cholesterol, triglycerides, insulin level and estimated glomerular filtration rate (eGFR). In all OSA severity categories, hs-TnT was significantly related to the risk of death or incident heart failure, and this relationship was strongest in the severe OSA group.
Limitations of the study include its cross-sectional design, which precludes conclusions on causality, and a limited number of participants with severe OSA.
"Our results suggest a relationship between subclinical myocardial injury and the increased cardiovascular risk seen in patients with OSA," said Dr. Shah. "Monitoring of hs-TnT levels in these patients may have prognostic value, particularly in patients with severe OSA."
 MEDINDIA
MEDINDIA


 Email
Email