Sleeve gastrectomy improves chances of successful organ transplantation in morbidly obese patients, reveals study.
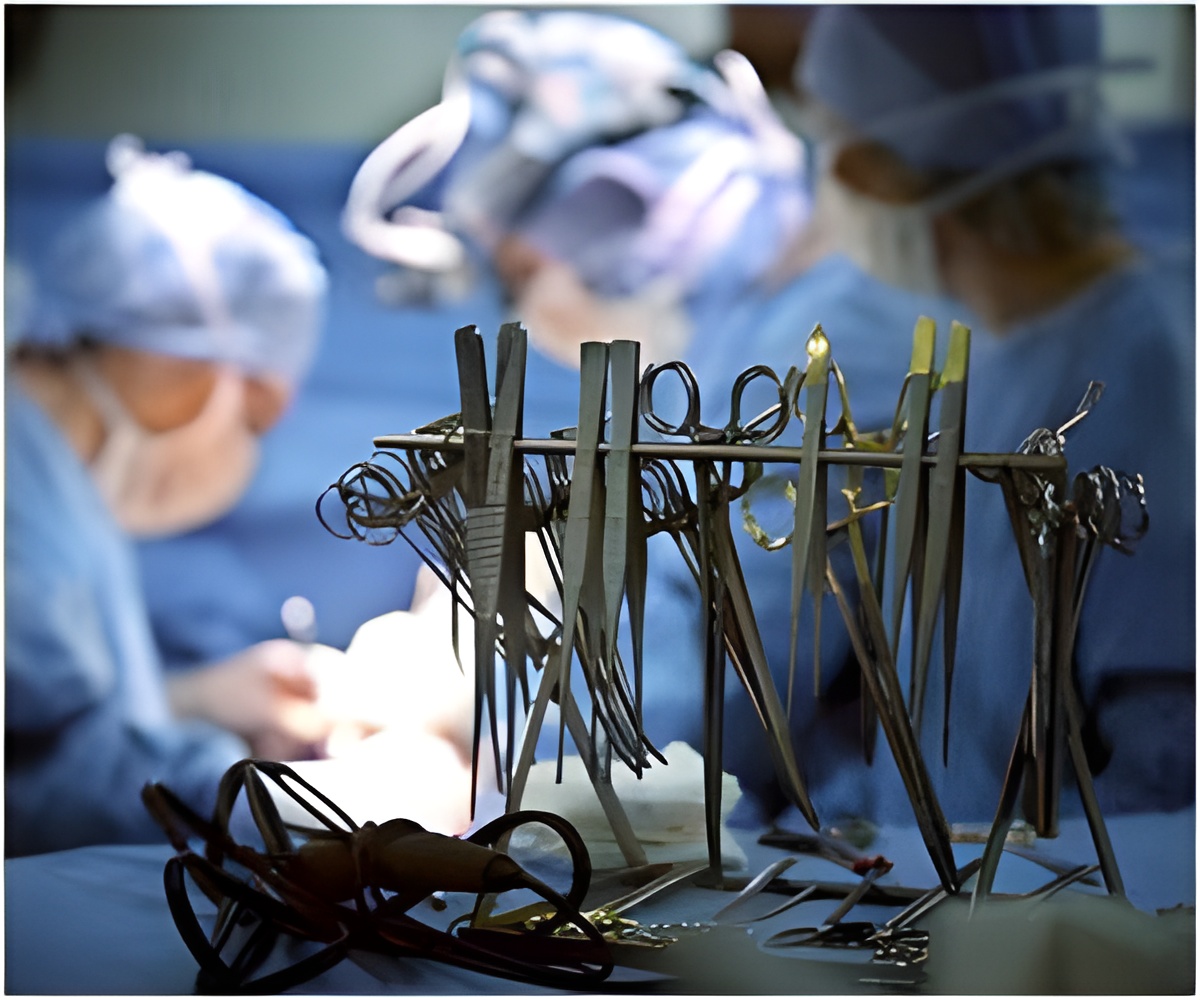
After gastric sleeve surgery, patients lost 17 percent of their excess weight at one month, 26 percent at three months, 50 percent at 12 months, and 66 percent at 24 months. Within nine months of surgery, one patient''s kidney function stabilized and he was taken off the transplant list, one patient had a combined liver and kidney transplant, one patient had a kidney transplant and six patients had liver transplants. Sixteen patients are currently on the transplant list and have lost enough weight to qualify for transplantation at UCSF. There were six complications among the group and one patient died four years later, while waiting for a transplant.
"This study suggests sleeve gastrectomy may be performed safely in carefully selected morbidly obese patients with impending organ failure and the significant weight loss they achieve may make them more suitable candidates for transplantation," said lead study author Matthew Yi-Chih Lin, MD, a bariatric surgeon at the UCSF School of Medicine.
In addition to significant weight loss, gastric sleeve patients saw improvements in obesity-related health conditions including Type 2 diabetes. Seven of the 13 patients with Type 2 diabetes had complete resolution of the disease and one patient was able to significantly reduce insulin use.
With more than two-thirds of Americans overweight or obese, obesity-related liver and kidney diseases are becoming a more common reason for transplantation.1,2 However, many who are waiting for a transplant may not qualify for it because of their excess weight. Researchers say most centers will not perform organ transplantation in
patients who have BMIs of more than 35 to 40.
According to the federal government, there were 16,898 kidney transplant procedures in 2010, with 94,598 people on the waiting list. Liver transplants numbered 6,291, with 16,954 people on the waiting list.3 About one-third of people on organ transplantation waiting lists are obese and as many as 15 percent are morbidly obese.4
In a laparoscopic sleeve gastrectomy, surgeons remove almost 85 percent of the stomach and shape the remaining stomach into a tube or sleeve.5 The minimally invasive procedure limits the amount of food patients can consume and helps them feel full sooner.
About Obesity and Metabolic and Bariatric Surgery
Obesity is one of the greatest public health and economic threats facing the United States.6 Approximately 72 million Americans are obese7 and, according to the ASMBS, about 18 million have morbid obesity. Obese individuals with a BMI greater than 30 have a 50 to 100 percent increased risk of premature death compared to healthy weight individuals as well as an increased risk of developing more than 40 obesity-related diseases and conditions including Type 2 diabetes, heart disease and cancer.8,9 The federal government estimated that in 2008, annual obesity-related health spending reached $147 billion,10 double what it was a decade ago, and projects spending to rise to $344 billion each year by 2018.11
Metabolic/bariatric surgery has been shown to be the most effective and long lasting treatment for morbid obesity and many related conditions and results in significant weight loss.12,13,14 In the United States, about 200,000 adults have metabolic/bariatric surgery each year.15 The Agency for Healthcare Research and Quality (AHRQ) reported significant improvements in the safety of metabolic/bariatric surgery due in large part to improved laparoscopic techniques.16 The risk of death is about 0.1 percent17 and the overall likelihood of major complications is about 4 percent.18
Source-Newswise
 MEDINDIA
MEDINDIA



 Email
Email