After menopause vitamin D levels drop and may increase the risk of cancer and heart disease but supplements fail to show any benefits.
Highlights
- Low vitamin D status may increase the risk of cancer.
- Supplementing the active form of vitamin D in healthy adults may not have beneficial effect.
- Postmenopausal women supplemented with vitamin D and calcium did not show a reduced risk for cancer.
Joan Lappe, Ph.D., R.N., of the Creighton University Schools of Nursing and Medicine, Omaha, and colleagues randomly assigned 2,303 healthy postmenopausal women 55 years or older (average age, 65 years) to the treatment group which was given 2,000 IU/d of vitamin D3 and 1,500 mg/d of calcium or to the placebo group. Duration of treatment was four years. The researchers examined the incidence of all types of cancer (excluding nonmelanoma skin cancers).
A new diagnosis of cancer was confirmed in 109 participants, 45 (3.89 percent) in the vitamin D3 + calcium group and 64 (5.58 percent) in the placebo group (difference, 1.69 percent). Incidence over four years was 0.042 in the treatment group and 0.060 in the placebo group. There was no statistically significant difference between the treatment groups in incidence of breast cancer.
Adverse events potentially related to the study included kidney stones (16 participants in the treatment group and 10 in the placebo group) and elevated serum calcium levels (six in the treatment group and two in the placebo group).
The authors write that one explanation for lack of statistically significant differences between the treatment groups in all-type cancer incidence is that the study group had higher baseline vitamin D (serum 25-hydroxyvitamin D) levels compared with the U.S. population.
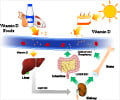
- Vitamin D helps the body use calcium and phosphorus to make strong bones and teeth.
- Two major forms of vitamin D that are important to humans are vitamin D2, or ergocalciferol, and vitamin D3, or cholecalciferol.
- Vitamin D2 is made naturally by plants, and vitamin D3 is made naturally by the body when skin is exposed to ultraviolet radiationin sunlight. Both forms are converted to 25-hydroxyvitamin D in the liver.
- 25-Hydroxyvitamin D is further modified to 1,25-dihydroxyvitamin D, or calcitriol, the active form of vitamin D in the body.
- The most accurate method of evaluating a person’s vitamin D status is to measure the level of 25-hydroxyvitamin D in the blood.
Previous Research on the Role of Vitamin D in Cancer
Exposure to ultraviolet light from sunlight leads to the production of vitamin D, and so researchers hypothesized that variation in vitamin D levels might account for this association.
A number of epidemiologic studies have investigated whether people with higher vitamin D intakes or higher blood levels of vitamin D have lower risks of specific cancers. The results of these studies have been inconsistent.
The cancers for which the most human data are available are colorectal, breast, prostate, and pancreatic cancer. Numerous epidemiologic studies have shown that higher intake or blood levels of vitamin D are associated with a reduced risk of colorectal cancer.
In contrast, the Women’s Health Initiative randomized trial found that healthy women who took vitamin D and calcium supplements for an average of 7 years did not have a reduced incidence of colorectal cancer.
"Further research is necessary to assess the possible role of vitamin D in cancer prevention."
Reference
- Joan Lappe et al., Vitamin D, calcium supplementation among older women does not significantly reduce risk of cancer, JAMA (2017) http://jamanetwork.com/journals/jama/fullarticle/10.1001/jama.2017.2115.
- Vitamin D and Cancer Prevention https://www.cancer.gov/about-cancer/causes-prevention/risk/diet/vitamin-d-fact-sheet.
Source-Medindia