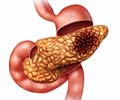
The implant which is placed in the peritoneal cavity resembles a spider’s web with islet cells embedded in a calcium-releasing thread.
Highlights
- TRAFFIC or Thread-Reinforced Alginate Fiber For Islets enCapsulation can help treat type 1 diabetes.
- The thread is a calcium-releasing, nanoporous polymer and is coated with islet cells that produce insulin.
- Through minimally invasive laparoscopic surgery, the thread can be implanted in the peritoneal cavity.
TRAFFIC - Insulin Cells Embedded in a Thread
Taking inspiration from the way water beads on a spider's web, Ma and his team first attempted to connect the islet cell-containing capsules through a string but realized that it would be better to put the hydrogel layer uniformly around a string instead. The string is an ionized calcium-releasing, nanoporous polymer thread.
This thread - which the group has dubbed TRAFFIC (Thread-Reinforced Alginate Fiber For Islets enCapsulation) - was inspired by a spider's web but, according to Ma, is even better because the hydrogel covers the thread uniformly.
"You don't have any gaps between capsules," he said. "With a spider's silk, you still have gaps between the water beads. In our case, gaps would be bad in terms of scar tissue and the like."
Drawback of Other Treatments
The ability to remove the transplant is key because of its potential to form tumors. "When they fail or die, they need to come out," Ma said. "You don't want to put something in the body that you can't take out. With our method, that's not a problem."
Facts on Type 1 Diabetes
- Nearly 1.25 million Americans are living with T1D, including about 200,000 youth (less than 20 years old) and more than 1 million adults (20 years old and older).
- Each year 40,000 people are diagnosed with type 1 diabetes
- 5 million people in the U.S. are expected to have T1D by 2050, including nearly 600,000 youth.
- Between 2001 and 2009, there was a 21 percent increase in the prevalence of T1D in people under age 20.
- In the U.S., there are $14 billion in T1D-associated healthcare expenditures and lost income annually.
- Less than one-third of people with T1D in the U.S. are consistently achieving target blood-glucose control levels.
- Minglin Ma, Dan Luo ,Wei Song, Jason Lu, Yehudah Pardo, Dahua Shou, Ling Qi, Yewei Ji. ‘Spider's web inspires removable implant that may control type 1 diabetes.’ Proceedings of the National Academy of Sciences (2017).
- http://www.jdrf.org/about/what-is-t1d/facts/
Source-Medindia