A randomized controlled study was conducted for establishing the efficacy of artificial pancreas over conventional insulin therapy in type I diabetes adults, and control of nocturnal hypoglycemia
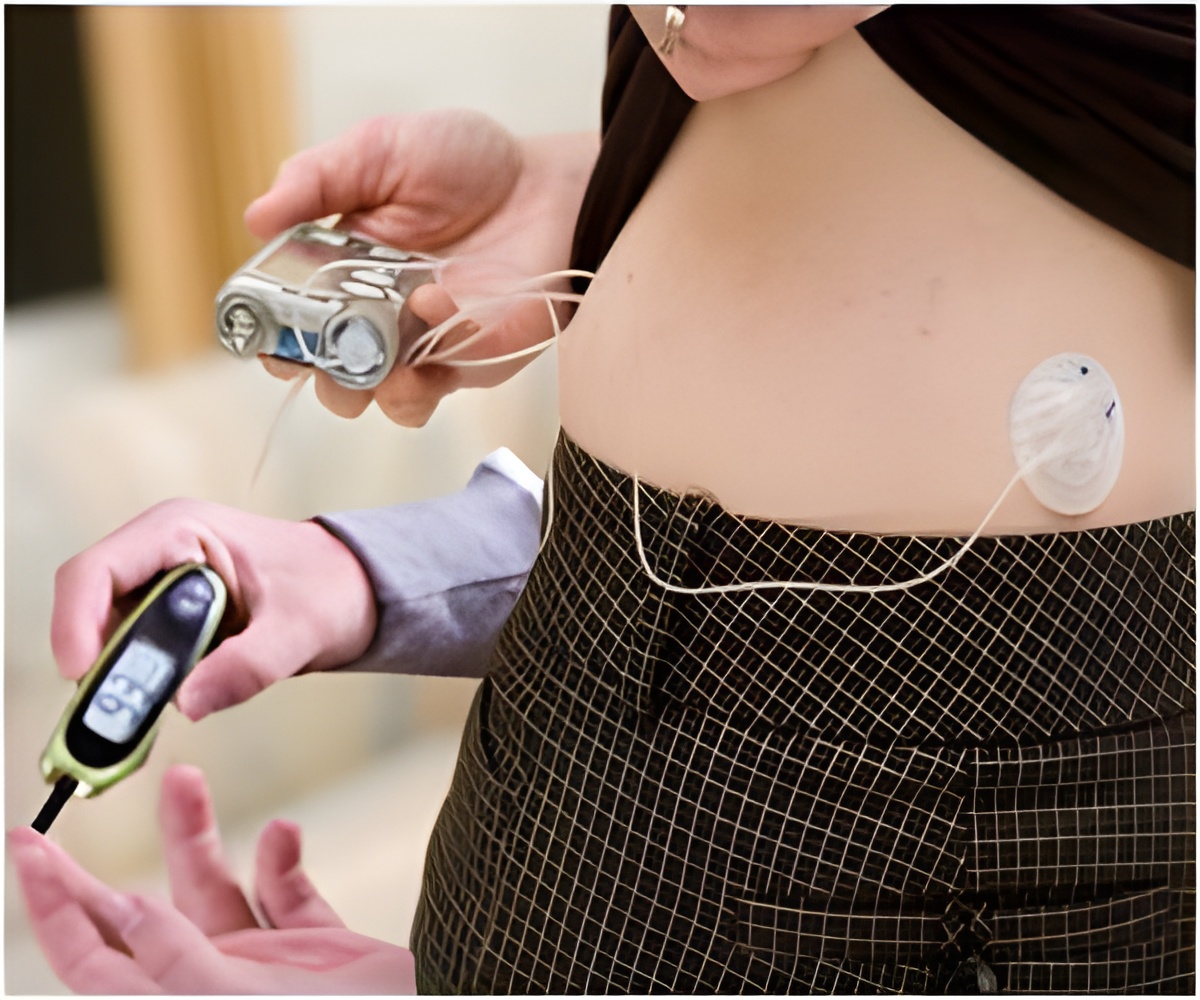
An important British study led by Roman Hovorka was conducted to analyze and assess the efficacy of overnight Closed Loop Insulin Delivery (or in other words - artificial pancreas) in diabetics with type 1. Artificial pancreas combines the two diabetes technology, namely insulin pumps and blood glucose monitoring, with computer algorithm to improve glucose control and reduce the risk of nocturnal hypoglycemia.
The volunteers for the study consisted of 24 adults with type-1 diabetes, belonging to the age group 18 to 65 years (10 males and 14 females) who were on insulin pump therapy for the last 3 months before the trial.
The study began by testing 12 individuals post medium size meal, and remaining 12 were tested following alcohol with larger meal.
Sensor measurements of glucose were fed in the computer algorithm, during the overnight closed loop delivery, at the rate of 15 minutes interval as advised on insulin pump infusion. Conventional pump settings were applied during the control nights.
13 people were chosen for the 'eating in' portion of the study and were randomly assigned for either closed loop delivery of insulin or conventional insulin pump therapy for 2 nights separated by 1 to 3 weeks. On both visits participants ate an identical meal comprising 60g of carbohydrate at 7 in the evening. During the intervention visit, closed loop insulin delivery was applied from 7 in the evening to 8 in the morning next day. During the control visit, participants applied their usual insulin pump settings over the same timeframe.
For 'eating out' phase of the trial, 12 type-1 diabetics were given a larger meal (100g of carbohydrate) at 8:30 in the evening accompanied by prandial insulin and dry white wine (7.2 mL/kg or 6.6 units per 70 kg participant) with or after their meal, completing the meal by 10 in the night. As with the other trial, some were managed with the artificial pancreas while the others used conventional insulin pump therapy from 10 in the night to 12 pm the next day.
The most significant outcome of the study was the comparison of time required for targeting plasma glucose levels (3.91-8.0mmol/L), in closed loop delivery and controlled period. Pooled data analysis and time glucose levels, being below targets (
Says Hovorka, 'In these two small crossover trials overnight closed loop delivery of insulin (artificial pancreas) in adults with type 1 diabetes improved glucose control and reduced exposure to low plasma glucose levels, with no overnight values below 3.0 mmol/L'.
The trials successfully suggested the effectiveness in improving overnight control of plasma glucose levels and mitigating the risks of nocturnal hypoglycemia in adults with type-1 diabetes.
Conclusion These two small crossover trials suggest that closed loop delivery of insulin may improve overnight control of glucose levels and reduce the risk of nocturnal hypoglycemia in adults with type-1 diabetes.
Source: The Study was conducted by Roman Hovorka, et al published on14 April, 2011 in BMJ
BMJ 2011 http://www.bmj.com/content/342/bmj.d1855.full?sid=7886a784-e7ef-4fd2-b7b3-be9cbdf729cb
Source-Medindia
 MEDINDIA
MEDINDIA




 Email
Email