Study finds links between continuous glucose monitoring and better control of blood sugar levels in adults with type 1 diabetes.
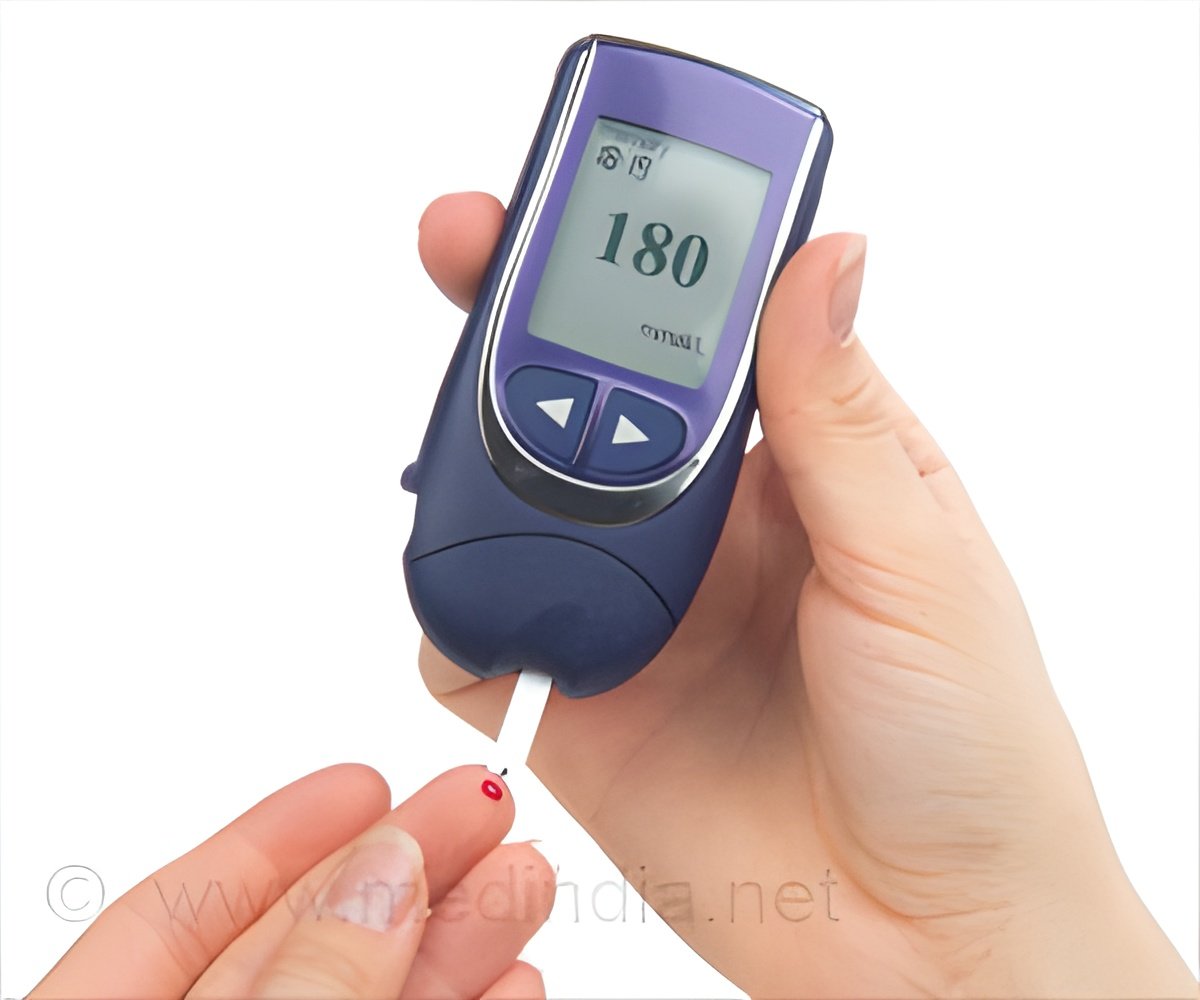
- To lower the risk of complications associated with type 2 diabetes, continuous monitoring of blood sugar is necessary.
- New study shows that the use of continuous glucose monitoring compared with conventional treatment, helps in lowering the mean sugar levels.
- Apart from offering protection to the patient, the continuous glucose monitoring also improved quality of life and sense of well-being.
TOP INSIGHT
Continuous glucose monitoring may result in better glycemic control in type 1 diabetes, compared with conventional treatment.
Type 1 diabetes is an autoimmune disease in which the body's immune system attacks the pancreas and prevents it from producing insulin. It mostly affects children and young adults.
Insulin is an hormone that is necessary to transport the glucose in the bloodstream to the cells for energy. In the absence of insulin, glucose tends to accumulate in the blood, increasing the level of blood sugar.
According to the he American Diabetes Association, around 1.25 million Americans have type 1 diabetes and an estimated 40,000 people will be newly diagnosed each year in the U.S.
Continuous Glucose Monitoring Versus Conventional Treatment
A total of 161 people took part in the study, from Härnösand in the north to Malmö in the south. All patients required insulin injections several times per day in order to keep their blood sugar levels in check.
- use a traditional equipment to prick their finger at least four times per day in order to measure the sugar levels
- use a device which measures the blood sugar continually via a thin filament under the skin on the stomach and a separate unit kept in the pocket would beep or vibrate when the sugar level was to high or too low
Decrease in Sugar Level and Improved Well-Being
"The principal question was whether there would be a difference in the average blood sugar levels. What we saw was that when patients used this continual blood sugar measurement, they had a lower blood sugar level on average; something which is considered significant in reducing the risk of complications with type 1 diabetes," Marcus Lind explains.
The blood sugar value was measured using the marker HbA1c. This gives the mean value over a three-month period.
The HbA1c levels dropped by five millimole per mole in the group that had continuous glucose monitoring.
During the washout period, 7 patients had severe hypoglycemia.
"Different interpretations have been made at different hospitals across the country, and the interpretations also vary from one country to the next. A grey zone has been created pending the arrival of this type of long-term study," says Marcus Lind.
A decrease in the mean sugar levels has a protective effect on the patient group.
"When there are high sugar levels in the cells, various biochemical processes are triggered which increase the risk of damage, primarily to nerves and vessels. If you have high sugar values over long periods, for example, the retinas, kidneys and heart can be affected. The higher the values, the more harmful, which is why this is so important," Marcus Lind explains.
Treatment satisfaction levels and sense well-being also increased.
"It's important how the patients experience the treatment in their everyday lives in terms of their willingness to continue; it mustn't get too complicated. Quality of life and well-being are also becoming increasingly emphasized in guidelines for diabetes care," says Marcus Lind.
To assess the clinical outcomes and longer-term adverse effects, further research is needed.
The findings are published in the Journal of the American Medical Association.
References:
- Your journey with type 1 diabetes - (https://diabetes.org/living-with-diabetes/type-1)
- Marcus Lind et al. Continuous Glucose Monitoring vs Conventional Therapy for Glycemic Control in Adults With Type 1 Diabetes Treated With Multiple Daily Insulin Injections. Journal of the American Medical Association ; (2017) doi:10.1001/jama.2016.19976
Source-Medindia
 MEDINDIA
MEDINDIA

 Email
Email










