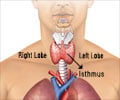
In a recent study, free thyroxine levels (FT4) were found to positively correlate with development of Age-related macular degeneration (AMD).

AMD has an unknown etiology wherein the causes are still unclear. The major risk factors include age, ethnicity, family medical history of AMD and smoking. However, according to a recent study published in BMC Medicine, researchers Layal Chakar, Gabriëlle HS Buitendijk, Abbas Dehghan, Marco Medici and Albert Hofman et al., found a link between the thyroid hormone and AMD. In animal studies, it had been proved that inducing hypothyroidism in mice with retinal degeneration preserves cone photoreceptors while hyperthyroidism worsens the deterioration. The researchers investigated this correlation in human populations.
The researchers studied data collected from 5,573 participants from the Rotterdam Study in the age range of 55 years or older. The Rotterdam Study is a population-based cohort study to examine factors that determine the occurrence of cardiovascular, neurological, ophthalmologic, psychiatric, and endocrine diseases in the elderly population residing in Ommoord, a suburb of Rotterdam. The study began in 1989.
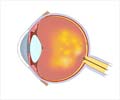
In the current study, the researchers explored correlations between free thyroxine (FT4), thyroid-stimulating hormone (TSH) and development of AMD. TSH is a regulatory hormone that controls the release of thyroid hormone. A low level of TSH is seen in hyperthyroidism while a high level is seen in hyperthyroidism. The aim of the study was to find an association between FT4, TSH with retinal pigment alterations (RPA), which act as an early warning for retinal damages.
The researchers were able to demonstrate a positive correlate between elevated levels of FT4 and increased risk of AMD. They discovered an association between higher thyroid levels and RPA. This suggests an important role played by the thyroid hormone in the development of AMD. However, the study did not indicate a link between TSH and AMD.
The study has significant implications for clinical practice in terms of treating hypothyroidism with thyroid hormone. The researchers suggest a cautious approach to treating subclinical hypothyroidism, a condition where FT4 levels are normal but TSH levels are high. The researchers also suggest that treatment of thyroid cancer, which involves suppressing TSH, could possibly lead to development of AMD. However, further studies are required to establish the same.
References:
1. Chakar, L., Buitendijk, G., Dehghan, A., Medici, M., Hofman, A. et al. (2015). Thyroid function and age-related macular degeneration: a prospective population-based cohort study - the Rotterdam Study. BMC Medicine, 13:94, doi:10.1186/s12916-015-0329-0. Accessed on 5 August 2015 from http://www.biomedcentral.com/1741-7015/13/942. Ittermann, T. & Jürgens, C. (2015). Thyroid function: a new road to understanding age-related macular degeneration? BMC Medicine, 2015; 13:95, doi: 10.1186/s12916-015-0343-2. Accessed on 5 August 2015 from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4407388/
Source-Medindia
 MEDINDIA
MEDINDIA
 Email
Email