Failure of organs like heart, liver and kidneys could be reversed and organs can be made to survive. There are two cell types in the body that can help in restoring a non-functioning or failing organ to a functioning organ.
Highlights:
- New research is exploring how people can survive organ failure
- Two different types of cells work together to restore the functioning of failed organs
- Treatments for acute organ failure could be developed from the findings
TOP INSIGHT
There is hope for patients who suffer from organ failure. Understanding the mechanism can help develop effective treatment methods.
Read More..
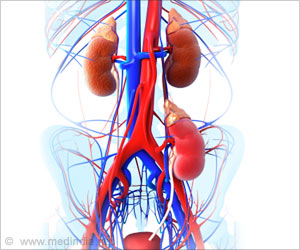
What Happens in Organ Failure?
In case of organ failure, the cells that have survived in the organ, work extensively to help the organ to continue functioning and the other stem-like cells help in replacing the damaged tissues. “When tissue is injured, cells divide to replace it, but the process of cell division in specialized cells would prevent the cell from performing its normal duties. In situations where an organ is failing, which means the organ already isn't functioning properly, your body can't afford to have many cells stop working,” explains Dr. Paola Romagnani, a Professor of Nephrology at the University Meyer Children's Hospital of Florence.“Up until recently, it was believed that function recovery after the injury was a consequence of regeneration involving all specialized cells simply ignoring that such cell divisions would imply a further potentially life-threatening decline of residual organ function,” Dr. Romagnani added.
How do the Cells Help Restore Function of Failing Organ ?
Since it has been known that regeneration of all specialized cells is not responsible for the recovery of function in the organs, it has also been understood that there are two types of cells that react to organ failure.“The majority of cells in an organ are highly specialized cells that have lost the ability for cell division but that can enhance their working capacity. In contrast, a minority of cells is un-programmed, like a stem cell, and able to divide efficiently,” says Dr. Romagnani. “Armed with this knowledge, we wanted to understand how the two processes worked together to help an organ recover from failure,” she added. Only the stem-like cells have the ability to divide quickly and replace the damaged cells, whereas, the cells in specialized organs like kidneys, liver and heart have only specific tasks to perform. “Skin, for example, performs the same function wherever it is, which makes rapid cell division an effective way to repair skin damage. Indiscriminate replication of specialized organ tissue, however, would reduce an organ's health more than it would help,” Dr. Romagnani explained.
On how the specialized cells react, she said, “This is why the cooperation between the two cell types is so important. The specialized cell will replicate its DNA, but not divide, which is a process known as endoreplication. By doing that, the cell is still able to function and the amount of work it can do greatly increases--it's making up the work of cells that have died. Simultaneously, or shortly after cells have endoreplicated, you have the stem-like cells rapidly dividing to replenish lost tissue.”
Organ Regeneration - Is One Technique Better than the Other?
Certain organs seem to be highly relevant on one technique than others, Dr. Romagnani and her team found while studying the interaction between the two cell types. The following example illustrates this point – “The heart tends to have smaller densities of stem-like cells than the liver, for example, which means the heart responds to organ failure largely with endoreplication of specialized cells and to a lesser degree with cell regeneration.” On the other hand, “In the liver, cell regeneration will occur more readily; but regardless of the more dominant reaction, both responses play critical roles in both organs.”There are pros and cons attached to both the recovery responses, which may have implications for developing medication which in turn may encourage one of the two responses over the other.
“Endoreplication is a way to quickly increase cell size and function undergoing hypertrophy, which is great in the short term because it can save a life, but in the long run, having a high proportion of cells in this state can result in chronic organ dysfunction due to the breaking-down of tissues,” Dr. Romagnani elaborated on the point.
Whereas, in case of cell division in stem-like cells, while in the long run, the tissue strength is better, there are also chances of cancer developing in the affected organ. “When you have a high number of cells that are efficient at dividing, you have a higher risk of cancer. These significant tradeoffs are likely why both methods exist and why it's so important for them to be balanced,” says Dr. Romagnani.
The Way Forward for Reversing Organ failure
Dr. Romagnani and her team are now looking forward to making use of this finding in developing treatments for acute organ failure. “Understanding the role of endoreplication in coordination with cell replication in each organ is really important. Researchers need to know that there are two mechanisms going on and that we need to target them separately. Currently, we don't have specific drugs for acute organ failure because up until now, trying to find a solution was utterly impossible. Now, we can take the next step,” she remarked.Reference:
- Surviving Acute Organ Failure: Cell Polyploidization and Progenitor Proliferation - (https://doi.org/10.1016/j.molmed.2019.02.006)
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email






