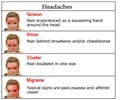
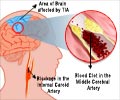
Patients with migraine, especially migraine with aura, are at an increased risk for perioperative stroke, reveals study.

- A stroke causes prolonged hospital stay, disability and even death
- Patients with a migraine, especially migraine with aura, appear to be at an increased risk for ischemic stroke soon after the surgery
- Identification of a patient with migraine prior to surgery can help the surgeon and anesthetist to take adequate precautions to prevent its occurrence
Studies have suggested an association between migraine and the increased risk of ischemic stroke. The research team from Massachusetts therefore conducted a study to see if patients with migraine are at a higher risk for ischemic stroke in the perioperative period, that is, around the time when they undergo surgery. Ischemic stroke is a type of stroke where a part of the brain gets damaged due to reduced blood supply.
A stroke following a surgery increases the duration of the hospital stay, prolongs disability as well as increases the chances of mortality. Therefore, if factors that could predict the chances of the stroke can be identified, these could be taken care of before the surgery, or increased precautions can be taken during the surgery to avoid a stroke.
The research team collected data from 124,558 patients undergoing surgery under general anesthesia over a period of seven years from Massachusetts, USA. They found that:
- Around 0.6% patients suffered a stroke within 30 days of the surgery. Patients undergoing vascular surgery had the highest rate, followed by cardiac surgery and neurosurgery.
- Among those who suffered from stroke, 11.9% patients were previously suffering from migraine.
- The risk for an ischemic stroke soon after surgery was higher in patients with prior migraine, especially migraine with aura.
- The risk was unrelated to other diseases and conditions that could also cause stroke
- Ambulatory patients with migraine were at a higher risk for stroke
- The risk for stroke in migraine patients was highest among those patients with a low estimated baseline risk of perioperative ischemic stroke
- Patients with migraine had an increased risk of posterior circulation strokes following the surgery, but also experienced partial anterior strokes
- Patients with migraine had a higher rate of ischemic stroke following discharge from the hospital
- Patients with migraine also had a higher re-admission rate within 30 days of the surgery. In addition to stroke, the readmission was also due to diseases of the neurologic, digestive or circulatory system, cerebrovascular disease, or due to symptoms of pain, syncope/collapse, or nausea/vomiting. Readmission increases the economic burden on the patient as well as the health care system.
- Administration of a high dose vasopressor (drug that increases blood pressure) and a possible right-to-left shunt appeared to increase the risk of stroke in migraine patients. These are important to note since they can be prevented or treated, and the stroke avoided. Adequate fluids during and after anesthesia and surgery could help to reduce the dosage of the vasopressor, which in turn can reduce the chances of stroke.
The study thus implies that migraine, especially migraine with aura, should be considered as a risk factor for stroke during the perioperative period, and extra caution should be taken in these patients during and after surgery. They also suggest an individual risk assessment for stroke should be carried out in these patients before the surgery.
- Timm FP et al. Migraine and risk of perioperative ischemic stroke and hospital readmission: hospital based registry study. BMJ 2017;356:i6635