Learn more about early syphilis mimicking acute sclerosing cholangitis.
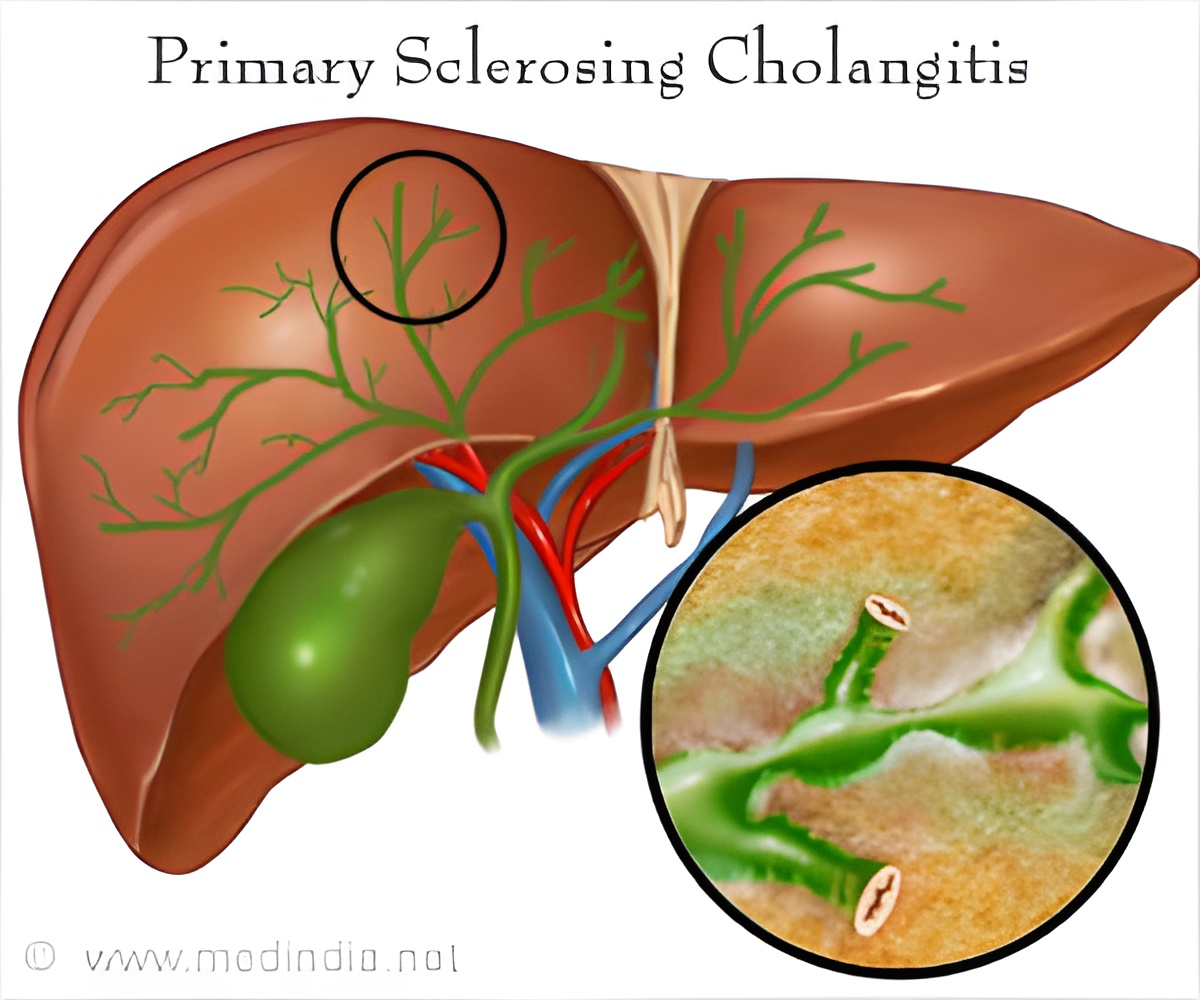
Syphilis, a sexually transmitted disease is caused by an organism called Treponema pallidum. The disease has three stages depending on the degree of severity: stage 1 (primary syphilis), stage 2 (secondary syphilis), stage 3 (tertiary syphilis). Primary syphilis is usually localized for example, at the genitals. Patients with secondary syphilis show symptoms like rash and sore throat, and can affect organs. Tertiary syphilis is a severe form of the disease which affects the brain and spinal cord, heart and skin. With the right antibiotics, syphilis can be treated. In fact, syphilis rarely progresses to the tertiary stage nowadays.
Case Studies
Syphilis as acute sclerosing cholangitis with elevated liver enzymes
A 36-year old HIV-positive man visited an outpatient genitourinary service with jaundice, rash and sore throat. Tests were carried out, which showed elevation in liver enzymes (alkaline phosphatase and alanine transaminase) more than ten times the normal range; liver ultrasound was though normal.
The diagnostic test magnetic resonance cholangiopancreatography (MRCP) revealed some kind of structuring and beading of the bile ducts, which was similar to that seen in sclerosing cholangitis. Blood tests were positive for syphilis infection. Biopsy of liver done revealed obstruction in large bile duct with inflammation around smaller ducts.
The patient was treated for secondary syphilis with oral steroids and benzathine penicillin (injected intramuscularly). Treatment resulted in marked improvement in symptoms and blood tests.
After treatment duration was completed, a repeat MRCP was done after 18 months, which showed resolution of the liver disease. This was a classic case for syphilis presenting as acute sclerosing cholangitis. There were other similar cases of syphilis in which elevated liver enzymes were observed.
Syphilis with hepatitis and raised liver enzymes
A 39-year-old homosexual man with HIV came to an infectious disease clinic with history of 3-week dull, intermittent pain located in upper right abdomen with no fever, chills, nausea, vomiting, or change in bowel habits. Also, he had no history of alcohol abuse or recent consumption of any over the counter medication which could affect the liver. The patient had been diagnosed for HIV many years back and no history of any opportunistic infection as well. Opportunistic infections are infections which do not occur in normal individuals but occur only in those who have reduced immunity.
The patient was on anti-HIV treatment of lamivudine, stavudine, and indinavir with an absolute CD4+ T cell count of 455 cells/mm3. CD4+ T cell count is indicative of the level of immunity in the patient. On physical examination, presence of jaundice and a generalized rash was noted. Abdominal examination showed tenderness in the right upper abdomen. Blood tests showed that liver enzyme alkaline phosphatase was elevated [727 IU/L (normal level, 20–125 IU/L)].
Blood tests were negative for hepatitis A, B and C infections. Ultrasound of abdomen did not reveal liver abnormality. However, blood tests were positive for syphilis. A diagnosis of syphilitic hepatitis was made and the patient was treated with penicillin G, following which the liver enzymes came back to normal.
Syphilis with liver involvement and rise in liver enzymes
A 28-year-old male evaluated three months prior for vomiting and upper abdominal pain had complaints about the upper mid-abdominal pain that worsened after eating. The patient reported having no fever, chills, no changes in urine, but presence of rash. Laboratory tests showed elevated liver enzymes. Though these symptoms subsided, liver enzymes further increased in the subsequent weeks. The patient also complained of mild sore throat.
Laboratory tests showed progressive rise in liver enzymes [alkaline phosphatase, aspartate aminotransferase (AST), and alanine aminotransferase (ALT)]. Ultrasound of liver and biliary tree showed no significant signs. Blood tests for syphilis were positive. The patient was negative for HIV.
On basis of this, the patient was diagnosed for secondary syphilis with liver involvement. Patient was then treated with 2.4 million units of benzathine penicillin G intramuscularly, liver enzymes then showed marked improvement.
Future Directions
In HIV-infected patients as well as in some other patients, liver involvement can present along with skin manifestations of secondary syphilis. As presentation of secondary syphilis is varied, diagnosis should be suspected in people with vague symptoms.The recognition of syphilis such as this is important since it is reversible with appropriate antibiotic treatment, and also reduces the financial burden that may otherwise be acquired in evaluating an HIV-positive patient with elevated liver enzymes.
References:
1. Primary sclerosing cholangitis. Accessed June 19 2015. Available from: http://www.mayoclinic.org/diseases-conditions/primary-sclerosing-cholangitis/basics/definition/con-200294462. Primary Sclerosing Cholangitis. Hopkins medicine. Accessed June 19 2015. Available from: http://www.hopkinsmedicine.org/gastroenterology_hepatology/_pdfs/liver/primary_sclerosing_cholangitis.pdf
3. Primary Sclerosing Cholangitis (PSC). Liver Foundation. Accessed June 19 2015.
4. Syphilis. NHS. Accessed 19 June 2015. Available from: http://www.nhs.uk/Conditions/Syphilis/Pages/Introduction.aspx
5. Suzuki I, Orfanidis N, Moleski S, Katz LC, Kastenberg D. The “Great Imitator” Presents with Abnormal Liver Enzymes. Accessed 19 June 2015. Available from: http://jdc.jefferson.edu/cgi/viewcontent.cgi?article=1171&context=tmf
6. Wallace HE, Harrison LC, Monteiro EF, Jones RL. The Great Pretender: early syphilis mimicking acute sclerosing cholangitis. Frontline Gastroenterol. 2015. Available from: http://fg.bmj.com/content/early/2015/04/09/flgastro-2015-100577.short?g=w_fg_ahead_sidetab
7. Mullick CJ, Liappis AP, Benator DA, Roberts AD, Parenti DM, Simon GL.
8. Syphilitic hepatitis in HIV-infected patients: a report of 7 cases and review of the literature. Clin Infect Dis 2004; 39:e100-5.
9. Treating syphilis. Accessed June 19 2015. Available from: http://www.nhs.uk/Conditions/Syphilis/Pages/Treatmentpg.aspx
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email









