Diabetic retinopathy is an eye disease that occurs in diabetics. The automated algorithm can improve patient outcomes by providing early detection and treatment.
Highlights
- Diabetic retinopathy is the leading cause of blindness in adults with type 2 diabetes.
- Diabetic eye disease is screened using retinal photography with manual interpretation.
- The evaluation of retinal images using an algorithm based on deep machine learning can improve early detection and treatment of diabetic retinopathy, claims research.
TOP INSIGHT
Algorithm-based on deep machine learning for detection of diabetic retinopathy can improve care and outcomes compared with the current ophthalmologic assessment.
Machine learning is a discipline within computer science that focuses on the development of computer programs on teaching machines to grow and change when exposed to new data. Machine learning has been leveraged for a variety of classification tasks including automated classification of diabetic retinopathy.
An algorithm is needed to maximize the use of automated grading and detect referable diabetic retinopathy. Deep learning is a machine learning technique that allows an algorithm to program itself from the given set of data.
Lead researcher Lily Peng, M.D., Ph.D., of Google Inc., Mountain View, Calif., and colleagues applied deep learning to create an algorithm for automated detection of diabetic retinopathy and diabetic macular edema in retinal fundus photographs. The algorithm was designed to detect specific lesions or predict the presence of any level of diabetic retinopathy.
Benefits of Automated Grading of Diabetic Retinopathy
- Early detection and treatment of diabetic retinopathy
- Increases efficiency and coverage of screening programs
- Reduces barriers to access
- Improves patient outcomes
The researchers used a data set of 128,175 retinal photographs for image classification. The images were graded 3 to 7 times for diabetic retinopathy, diabetic macular edema by a panel of 54 U.S. licensed ophthalmologists and ophthalmology senior residents between May and December 2015.
Both the data sets were used to analyze the prevalence of referable diabetic retinopathy (RDR), which is defined as moderate and worse diabetic retinopathy, referable diabetic macular edema, or both.
EyePACS-1
The EyePACS-1 data set consisted of 9,963 images from 4,997 patients and 8 percent of fully gradable images.
Messidor-2
The Messidor-2 dataset had 1,748 images of 874 patients and 15 percent of fully gradable images.
The algorithm achieved high sensitivities for detecting referable diabetic retinopathy (97.5 percent [EyePACS-1] and 96 percent [Messidor-2]) and specificities (93 percent and 94 percent, respectively) for detecting referable diabetic retinopathy.
The automated algorithm for the detection of diabetic retinopathy offers several advantages such as consistency of interpretation, high sensitivity, specificity and near instantaneous reporting of results.
The authors noted that, "These results demonstrate that deep neural networks can be trained, using large data sets and without having to specify lesion-based features, to identify diabetic retinopathy or diabetic macular edema in retinal fundus images with high sensitivity and high specificity.”
"Further research is necessary to determine the feasibility of applying this algorithm in the clinical setting and to determine whether the use of the algorithm could lead to improved care and outcomes compared with the current ophthalmologic assessment."
The study is published in JAMA.
Diabetic Retinopathy
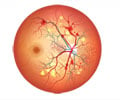
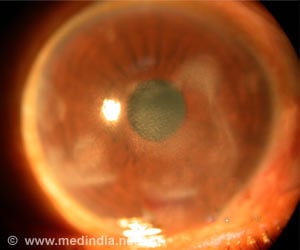
Diabetic retinopathy is a condition caused by damage to the blood vessels of the retina. More than 285 million people have diabetes and over one-third have signs of diabetic retinopathy.
About 29 percent of the Americans with diabetes have diabetic retinopathy. Adults with no retinopathy or mild diabetic retinopathy should go for annual screening. Adults with moderate diabetic retinopathy should go for screening every six months.
Source-Medindia
 MEDINDIA
MEDINDIA


 Email
Email










