A new study identifies a novel strategy to diagnose the leading cause of blindness in adults, diabetic retinopathy, before irreversible structural damage has occurred.
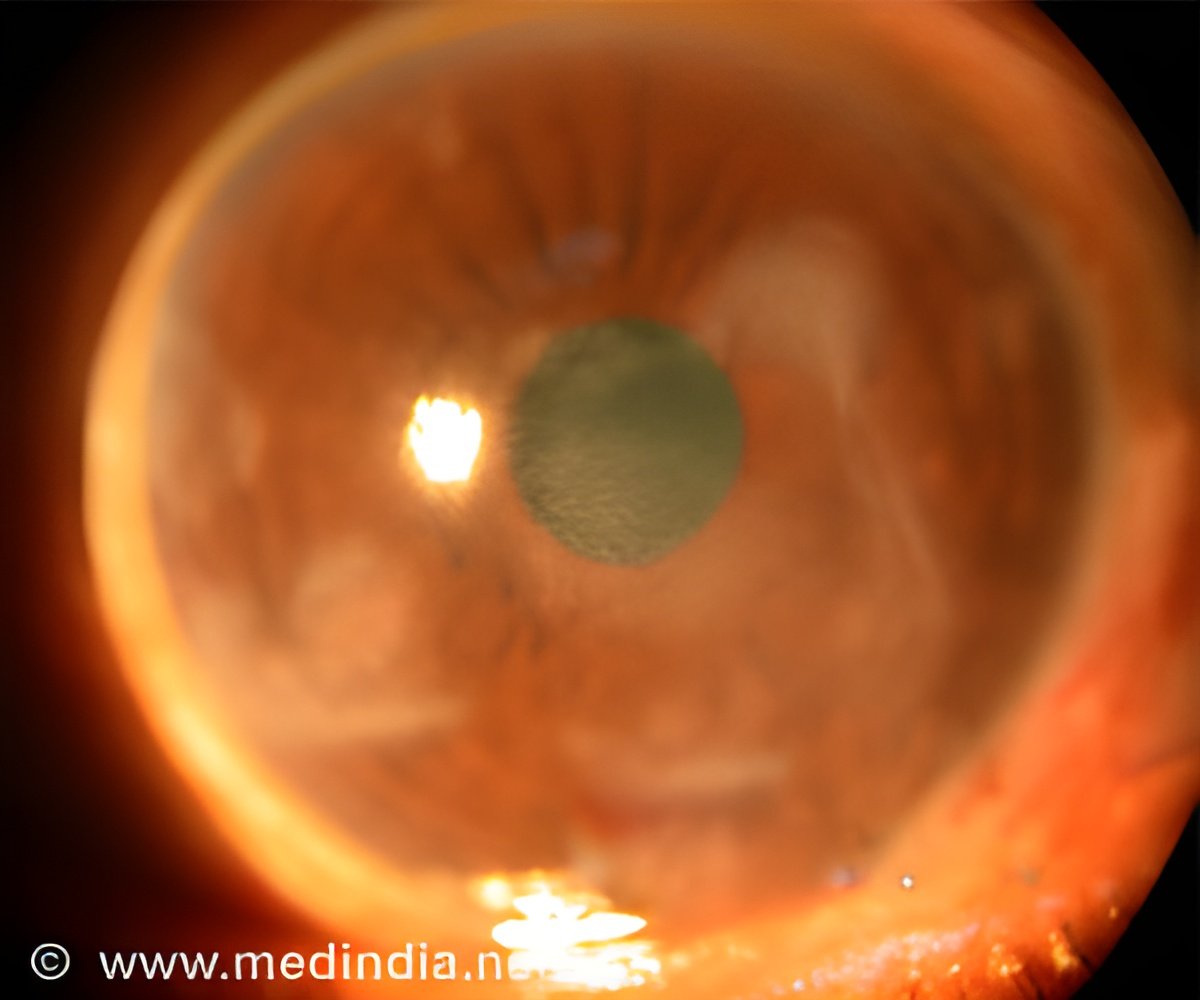
"My goal is to establish a versatile clinical tool that alerts of a disease process right when the first molecular changes take place. This will then provide ample opportunity to act, as opposed to merely acknowledge that there is structural damage that we cannot do anything about," said Ali Hafezi-Moghadam, M.D., Ph.D., a researcher involved in the work from the Center for Excellence in Functional and Molecular Imaging at Brigham and Women's Hospital and Harvard Medical School in Boston, MA. "Here, we have shown it in an important disease, the diabetic retinopathy, but there is no reason to stop there."
Hafezi-Moghadam and colleagues identified a target on the intraluminal surface of the retinal vessels that is expressed at higher levels in diabetes. They found significantly more vascular endothelial growth factor receptor 2 (VEGFR-2) in the diabetic micro-vessels compared to control. They then custom-generated molecular probes and characterized their binding properties.
Light-based live imaging was then used to quantify binding interaction. An unexpected finding in this work was that not only was VEGFR-2 higher in the retinas of diabetic animals as well as humans, but the molecule was found in the retinal micro vessels, not in the larger vessels. When the imaging probes were injected into the blood stream of living normal and diabetic animals, they circulated throughout the animal's vasculature. With the help of live imaging of the retinal vessels, it was possible to visualize the interaction of individual probes with their endothelial targets.
The probes transiently interacted with the intraluminal surfaces. In comparison, control probes with a surface moiety that does not interact with the inner vascular lumen freely flowed through the retinal micro vessels. Since the probe interaction with the inner vessel wall can be deduced to individual molecular interactions, the information gained from this study provides quantitative knowledge of target molecules in the retinal micro vessels.
"This study should be a huge eye-opener for doctors hoping to prevent eye disease resulting from diabetes," said Gerald Weissmann, M.D., Editor-in-Chief of The FASEB Journal. "This study shows that it is possible to do this, and the next step is to make this accessible at the clinical level. The sooner doctors can detect that their patients might have a vision problem, the more time they have to save someone's sight."
 MEDINDIA
MEDINDIA

 Email
Email