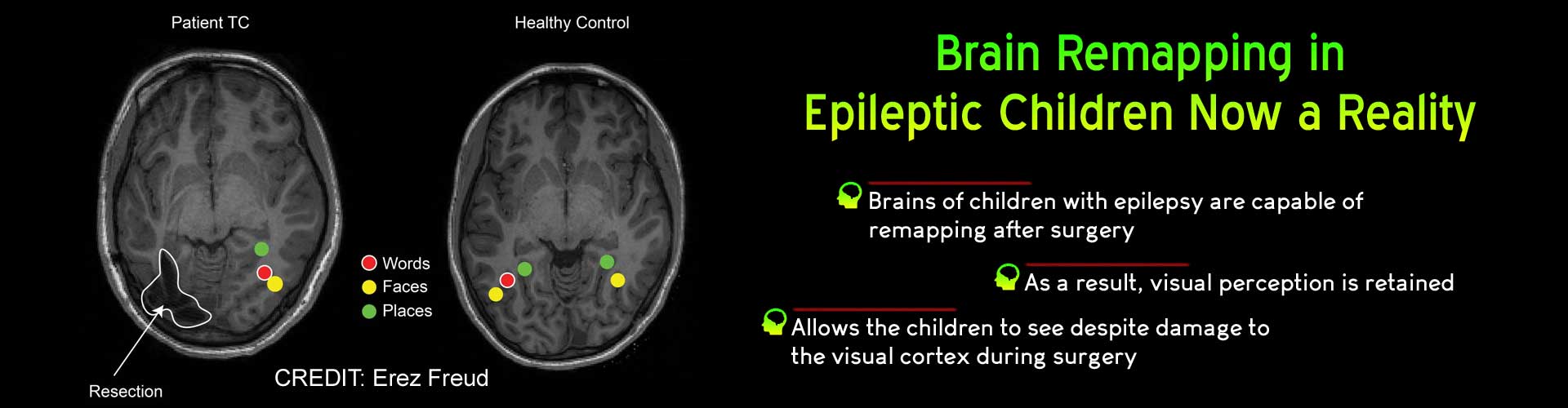
Brains of children with epilepsy are able to remap following surgery to retain visual perception. This enables the children to see, despite damage to the visual cortex of the brain.
- Brains of children with epilepsy are capable of remapping following surgery
- This allows visual perception to be retained
- As a result, the children are able to see despite lesions in the visual cortex sustained during surgery
The study, published in the Journal of Neuroscience, was led by Dr. Marlene Behrmann, PhD, who is a Professor of Psychology at Carnegie Mellon University, Pittsburgh, Pennsylvania, USA.
The co-lead author of the study was Dr. Erez Freud, PhD, who is an Assistant Professor in the Department of Psychology, Faculty of Health at York University, Toronto, Canada.
The other co-lead author was Dr. Tina Liu, PhD, who is a postdoctoral researcher at the National Institute of Mental Health (NIMH), Bethesda, Maryland, USA. She was formerly a PhD student at Carnegie Mellon University at the time of the study.
TOP INSIGHT
Brains of children with epilepsy are able to remap following surgery to retain visual perception. This enables the children to see despite damage to the visual cortex of the brain.
Read More..
Features of the Cases and Controls
- 10 children aged 6-17 years were included in the study
- All children had undergone surgery for severe epilepsy
- Epilepsy had been caused by injury (stroke) or tumor formation
- 3 children had lost parts of the visual cortex on the right side during surgery
- 3 children had lost parts of the visual cortex on the left side during surgery
- 4 children had lost other parts of the brain not associated with perception
- 10 healthy children were included in the study for comparison (controls)
- Visuoperceptual and neural profiles of the cases were compared with the controls
Study Procedure
The study was conducted in two phases in order to discern the mechanism of occurrence of plasticity due to the rewiring of the neural networks:Phase - 1
The first phase tested the children’s perception abilities that involved the following parameters:
- Facial recognition
- Classification of objects
- Reading
- Pattern recognition
The second phase involved the following procedures:
- The children’s brains were imaged using functional magnetic resonance imaging (fMRI)
- During the fMRI procedure, the children watched images of words, pictures, faces, places, and objects
- The fMRI enabled visualization of brain areas that were activated, as well as the measurement of the responses while the children watched the images
Study Findings
The study findings included the following:- 4 of 6 children who had partially lost their visual cortex during surgery, experienced a permanent diminishment of peripheral vision on one side
- In all children, epilepsy completely resolved or significantly improved after recovery from surgery
- 8 of 10 children showed normal perceptual abilities, including recognition of words, pictures, objects, faces, and places
- Despite suboptimal remapping/rewiring in some of the cases, the undamaged areas of the brain compensated for the damaged areas
Concluding Remarks
The research findings provide new insights into the plasticity of the cerebral cortex in children.Freud concludes: “It’s possible that early surgical treatment for children with epilepsy might be what allows this remapping.” He adds: “This may be because epilepsy is an ongoing condition of the brain and with early removal of the tissue, the brain may have time to rewire itself to the other healthy hemisphere and can, therefore, compensate for the functions that are impaired in the other part of the brain. But more research is needed to better understand exactly what the developmental processes are that mediate this compensation.”
Funding Source
The study was funded by the ’Vision: Science to Applications Program’ at York University, Toronto, Canada.Reference:
- Perceptual Function and Category-selective Neural Organization in Children with Resections of Visual Cortex - (http://www.jneurosci.org/content/early/2019/06/05/JNEUROSCI.3160-18.2019)
Source-Medindia
 MEDINDIA
MEDINDIA
 Email
Email