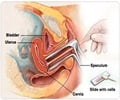
Currently in the UK, women aged between 25 and 49 are invited for screening every three years, and up to the age of 64, every five years.
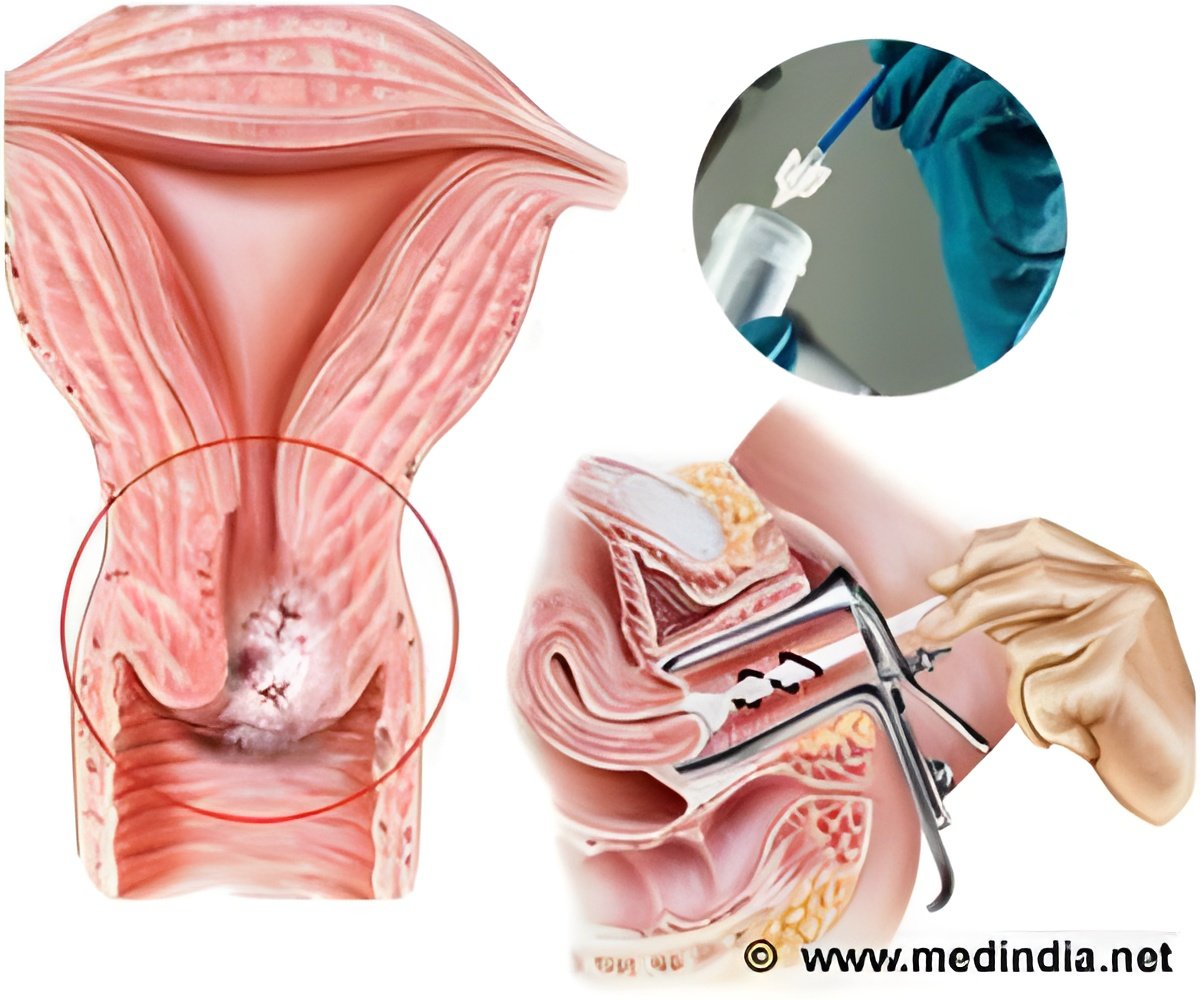
‘Women who test negative for human papillomavirus have very less chances of developing cervical cancer so screening them once in 5 years remains unaffected.’





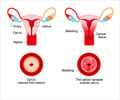
CIN is divided into grades - CIN1, 2 or 3. The higher the number, the more of the cervix is affected by abnormal cells. Currently in the UK, women aged between 25 and 49 are invited for screening every three years, and up to the age of 64, every five years.
In the Netherlands, screening intervals for HPV negative women aged at least 40 years will be increased from five to 10 years in 2017.
Evidence on the safety of screening intervals beyond five years is limited. So a team of researchers based in the Netherlands decided to assess the safety of extending screening intervals beyond five years.
They base their findings on 14 year follow-up data from over 43,000 women aged 29-61 years who took part in a large trial of three cervical screening rounds (each round done every five years).
Advertisement
The data show that HPV negative women aged at least 40 have a very low risk of CIN3+ (the highest grade of abnormal cells) in the long term, "indicating that extension of the current screening interval in the Netherlands is justifiable," say the authors.
Advertisement
The use of the HPV test result and age to define the year of next screen is a first step towards tailoring screening to individual risks - and could improve screening efficiency and eventually provide optimal prevention for all women, they write.
However, they point out that data on cervical cancer risk are inconclusive, and "therefore it remains important to closely monitor the number of interval cancers observed under the new HPV based screening programme."
Source-Eurekalert