A way to coat an iron-based MRI contrast agent for safer, cheaper and effective cancer detection has been developed by scientists.
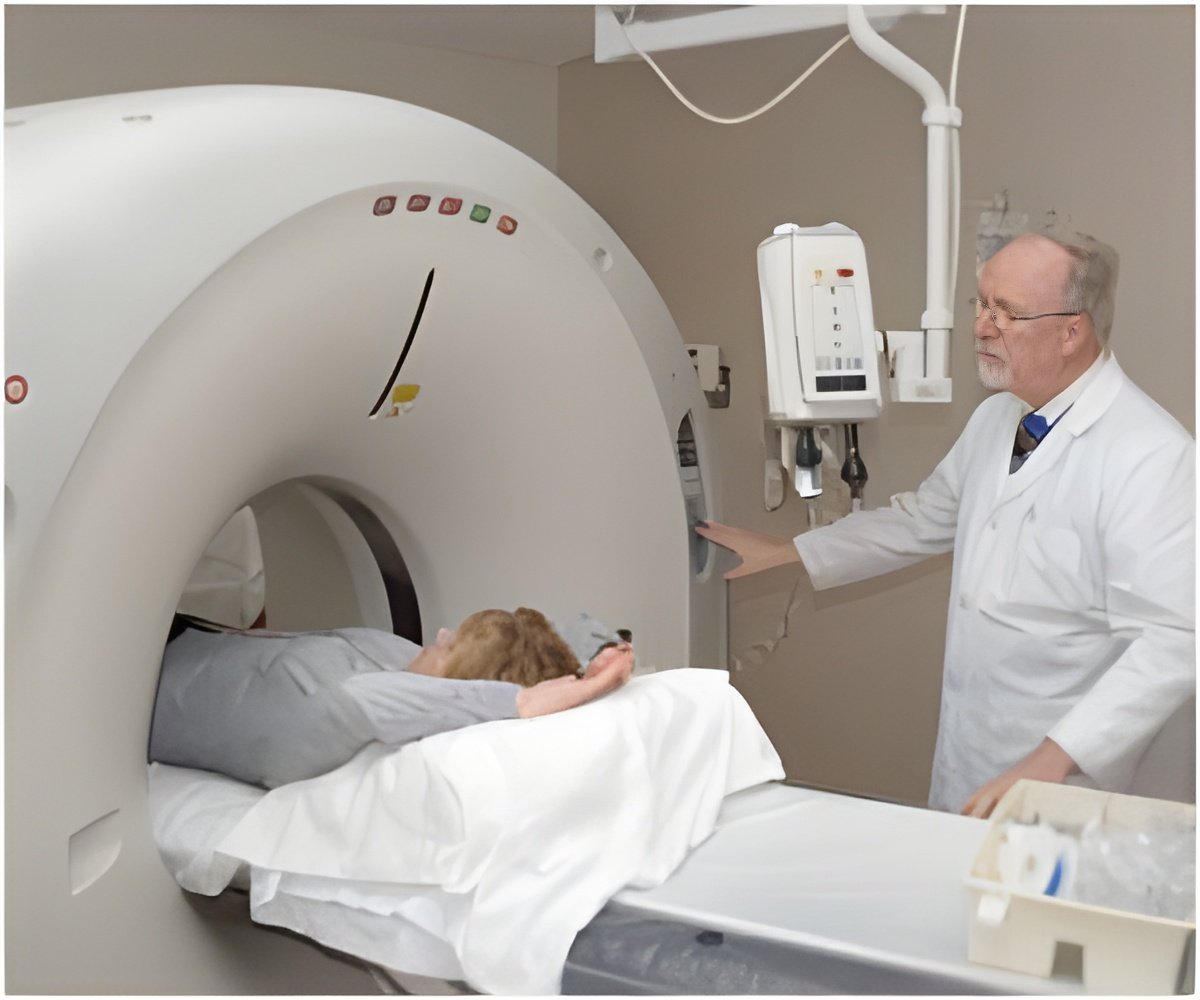
Magnetic resonance imaging, or MRI, is an increasingly common feature of medical care. Using a strong magnetic field to detect and influence the alignment of water molecules in the body, MRI can quickly produce pictures of wide range of bodily tissues, though the clarity of these pictures is sometimes insufficient for diagnoses. To improve the differentiation — or contrast — between tumors and healthy tissue, doctors can apply a contrast agent, such as nanoparticles containing iron oxide. The iron oxide can improve MRI images due to their ability to distort the magnetic field of the scanner; areas they are concentrated in stand out more clearly.
These nanoparticles, which have recently been approved in the United States for clinical use as contrast agents, are literally sugar-coated; an outer layer of dextran keeps the particles from binding or being absorbed by the body and potentially sickening the patient. This non-reactive coating allows the iron oxide to be flushed out after the imaging is complete, but it also means that the particles can't be targeted to a particular kind of tissue.
If the contrast agent could be engineered so it only sticks to tissue that is already diseased, such as tumors, it would solve both problems at once. Scientists have tried this approach by coating nanoparticles with proteins that bind only to receptors found on the exterior of tumors, but not all tumors are the same in this regard.
"One of the limitations of a receptor-based approach is that you just don't hit everything," Tsourkas said. "It's hard to recommend them as a screening tool when you know that the target receptors are only expressed in 30% of tumors."
"One of the reasons we like our approach is that it hits a lot of tumors; almost all tumors exhibit a change in the acidity of their microenvironment."
Some imaging technologies, such as magnetic resonance spectroscopy, can also take advantage of tumors' low-pH microenvironments, but they require expensive specialized equipment that is not available in most clinical settings.
This approach has another benefit: the more malignant a tumor is, the more it disrupts surrounding blood vessels and the more acidic its environment becomes. This means that the glycol chitosan-coated is a good detector of malignancy, opening up treatment options above and beyond diagnosis.
"You can take any nanoparticle and put this coating on it, so it's not limited to imaging by any means," said Tsourkas. "You could also use it to deliver drugs to tumor sites."
The researchers hope that, within seven to 10 years, glycol-chitosan-coated iron oxide nanoparticles could improve the specificity of diagnostic screening. The ability to accurately detect sites of malignancy by MRI would be an immediate improvement to existing contrast agents for certain breast cancer scans.
"Gadolinium is used as a contrast agent in MRI breast cancer screenings for high-risk patients. These patients are recommended to get an MRI in addition to the usual mammogram, because the sensitivity of mammograms can be poor," said Tsourkas. "The sensitivity of an MRI is much higher, but the specificity is low: the screening detects a lot of tumors, but many of them are benign. Having a tool like ours would allow clinicians to better differentiate the benign and malignant tumors, especially since there has been shown to be a correlation between malignancy and pH."
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email










