Genes that increase thyroid cancer risk have been identified by researchers.
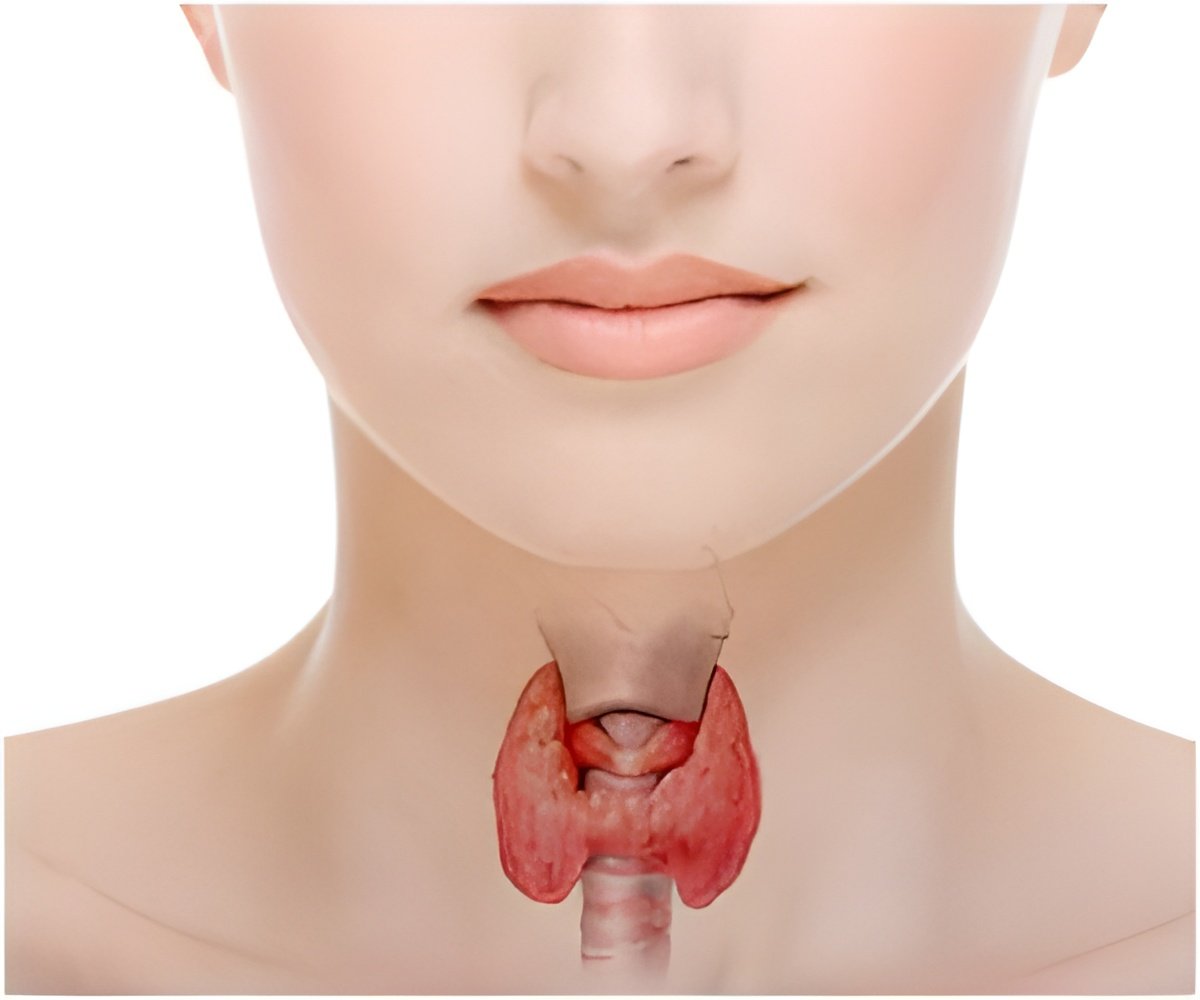
Research led by Charis Eng, M.D., Ph.D., Chair and founding Director of the Genomic Medicine Institute of Cleveland Clinic's Lerner Research Institute, included nearly 3,000 patients with Cowden syndrome (CS) or CS-like disease, which is related to an increased risk of breast and thyroid cancer.
Mutations in the PTEN gene are the foundation of Cowden syndrome. PTEN is a tumour suppressor gene, helping to direct the growth and division of cells. Inherited mutations in the PTEN gene have been found in approximately 80 percent of Cowden syndrome patients.
These mutations prevent the PTEN protein from effectively regulating cell survival and division, which can lead to the formation of tumours.
"Our investigation into the genetics behind thyroid disease raises important details relevant to diagnosis and treatment," said Dr. Eng.
"We hope to promote the earliest diagnosis and most targeted treatment possible."
Children with thyroid cancer are recommended to have testing for PTEN mutations, which could warrant surveillance for additional cancers or maladies. In contrast, alterations in the SDH and KLLN genes did not associate with thyroid cancer in children.
Once SDH and KLLN findings are independently validated, the tests could be implemented as a clinical routine test as well. Importantly, these three genes belong to different cell pathways so that specific molecular-targeted treatments can be utilized depending on which gene is involved.
The study has been published in the Journal of Clinical Endocrinology and Metabolism.
Source-ANI
 MEDINDIA
MEDINDIA

 Email
Email










