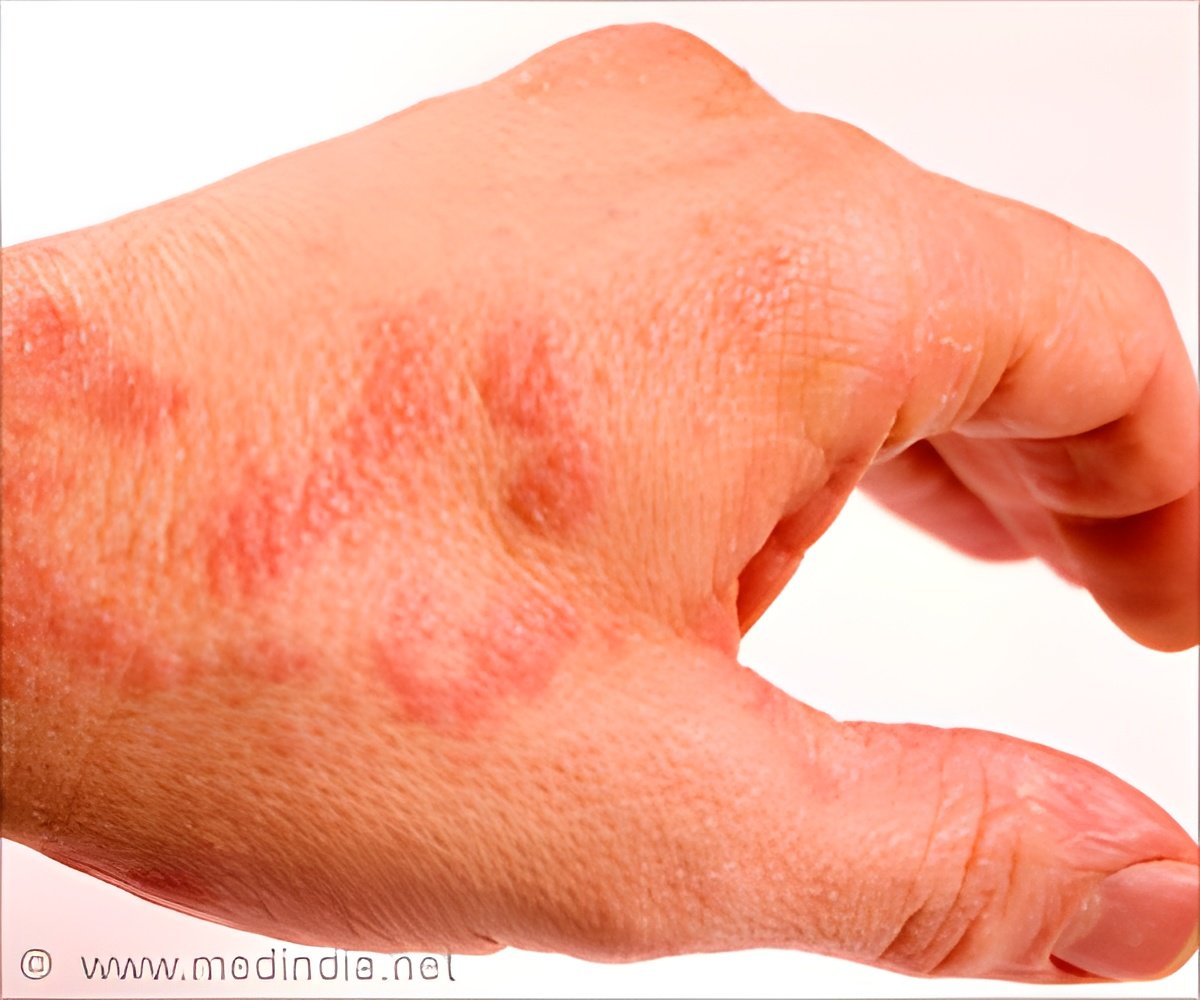
Eczema causes skin inflammation, deficiency in the skin’s barrier is the key to trigger eczema, finds study.
TOP INSIGHT
Deficiency in the skin barrier is a key to trigger eczema. Filaggrin is a skin barrier protein that impacts the development of eczema.
Common condition
Atopic eczema is one of the commonest skin conditions in the UK, affecting up to 10% of adults and 20% of children in the UK. It's more common in children, often developing before their first birthday and often persists into adulthood with severe itching that has profound effects on well-being and may lead to sleep disturbance.
The research builds on the important discovery by scientists in Dundee which showed that lack of the protein filaggrin in the skin caused an inherited dry skin condition known as ichthyosis vulgaris that is strongly linked to the development of atopic eczema, as well as other allergic diseases such as hayfever and asthma.
Nick Reynolds, Professor of Dermatology at Newcastle University and who works within the Newcastle Hospitals NHS Foundation Trust is the lead investigator of the study. He said: "We have shown for the first time that loss of the filaggrin protein alone is sufficient to alter key proteins and pathways involved in triggering eczema. This research reinforces the importance of filaggrin deficiency leading to problems with the barrier function in the skin and predisposing someone to eczema."
New skin model
Publishing in the Journal of Allergy and Clinical Immunology (JACI), researchers at Newcastle University, in collaboration with scientists at Stiefel, a GSK company, report on their development of a human model system.
This model enabled the team to discover proteins and signalling pathways directly down-stream of filaggrin, and most importantly, identified a number of key regulatory mechanisms. These included regulators of inflammatory signalling, cell structure, barrier function and stress response. These pathways were found to map to those networks observed in the skin of people with active eczema.
Nina Goad of the British Association of Dermatologists said: "This latest research from Newcastle is crucial as it expands on our knowledge of how filaggrin impacts on other proteins and pathways in the skin, which in turn trigger the disease. This type of research allows scientists to develop treatments that target the actual root cause of the disease, rather than just managing its symptoms. Given the level of suffering eczema causes, this is a pivotal piece of research."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email










