Scientists have been able to show that the damage to the locus coeruleus region of the brain could precipitate multiple sclerosis.
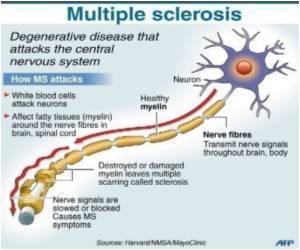
The pathological processes in MS are not well understood, but an important contributor to its progression is the infiltration of white blood cells involved in immune defense through the blood-brain barrier.
Douglas Feinstein, research professor in anesthesiology at the UIC College of Medicine, and his colleagues previously showed that the neurotransmitter noradrenaline plays an important role as an immunosuppressant in the brain, preventing inflammation and stress to neurons. Noradrenaline is also known to help to preserve the integrity of the blood-brain barrier.
Because the major source of noradrenaline is neurons in an area of the brain called the locus coeruleus, the UIC researchers hypothesized that damage to the LC was responsible for lowered levels of noradrenaline in the brains of MS patients.
“There’s a lot of evidence of damage to the LC in Alzheimer’s and Parkinson’s disease, but this is the first time that it has been demonstrated that there is stress involved to the neurons in the LC of MS patients, and that there is a reduction in brain noradrenaline levels,” said Paul Polak, research specialist in the health sciences in anesthesiology and first author on the paper.
For the last 15 years, Feinstein and his colleagues have been studying the importance of noradrenaline to inflammatory processes in the brain.
Advertisement
The researchers found that LC damage and reduced levels of noradrenaline occur in a mouse model of MS and that similar changes could be found in the brains of MS patients.
Advertisement
“There are a number of FDA-approved drugs that have been shown to raise levels of noradrenaline in the brain, and we believe that this type of therapeutic intervention could benefit patients with MS and other neurodegenerative diseases, and should be investigated,” he said.
Sergey Kalinin, post-doctoral research associate in anesthesiology, also contributed to the study. This study was supported by grants from the Department of Veteran Affairs and Partners for Cures.
Source-Medindia