- Fallopian Tube Cancer - (https://www.macmillan.org.uk/information-and-support/fallopian-tube-cancer#291434)
- All About Fallopian Tube Cancer - (https://www.oncolink.org/cancers/gynecologic/fallopian-tube-cancer/all-about-fallopian-tube-cancer)
- About Fallopian Tube Cancer - (https://www.mdanderson.org/cancer-types/fallopian-tube-cancer.html)
- Ovarian Cancer Types - Fallopian Tube - (http://www.cancerresearchuk.org/about-cancer/ovarian-cancer/types/fallopian-tube)
Fallopian Tubes - Overview
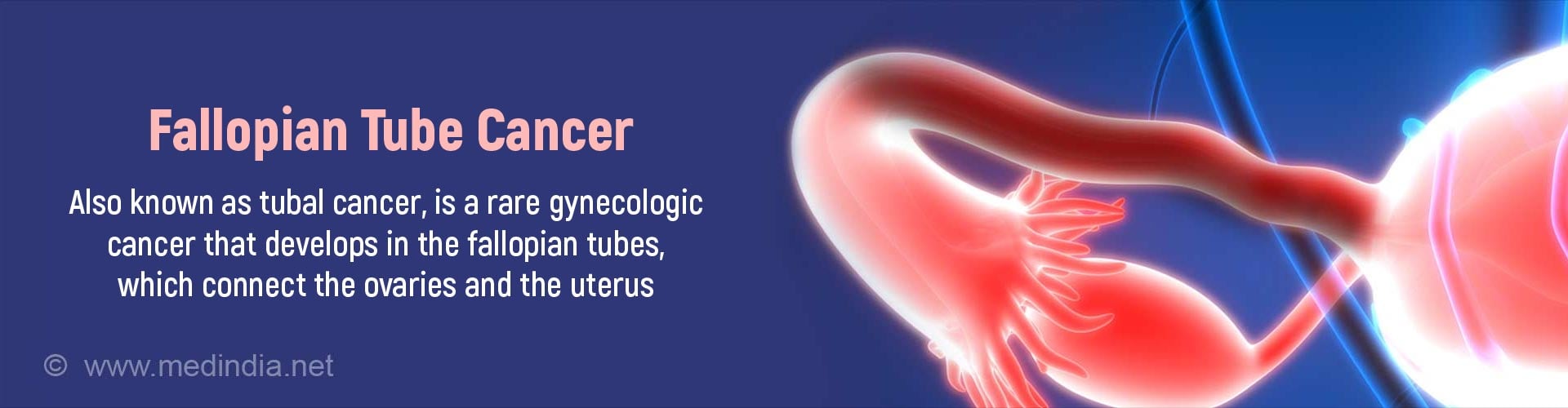
The fallopian tubes (or simply tubes) are paired tubular structures, one on either side of the uterus (womb). They link the ovaries to the uterus. In women of reproductive age, the ovaries produce eggs (ova) that travel via the fallopian tubes to the uterus. The egg may either develop into a fetus after fertilization by a sperm, or is expelled during menstruation in the absence of fertilization. Typically, an egg is discharged from an ovary into the fallopian tube of the same side every month. The movement of the egg to the uterus is aided by fine hair like projections (cilia) that line the inner surface of the fallopian tube.
What is Fallopian Tube Cancer?
Cancer arising from the fallopian tubes is termed fallopian tube cancer or tubal cancer. It is a comparatively rare form of gynecologic cancer with an incidence of about 1 in 100 (1 percent). A gynecological cancer is a cancer that arises from the female reproductive tract.
Tubal cancer can spread to other parts of the body via direct extension, the bloodstream or the lymphatics with deposition of cancer cells in the lymph nodes.
What are the Types of Fallopian Tube Cancer?
Depending on the site of origin within the fallopian tubes, the cancers may be classified as follows:
- Arising from the lining epithelium of the tube – Serous adenocarcinoma (most common type), endometrioid adenocarcinoma
- Arising from the smooth muscle of the tube – Leiomyosarcoma
- Arising from other cells – Transitional cell cancer
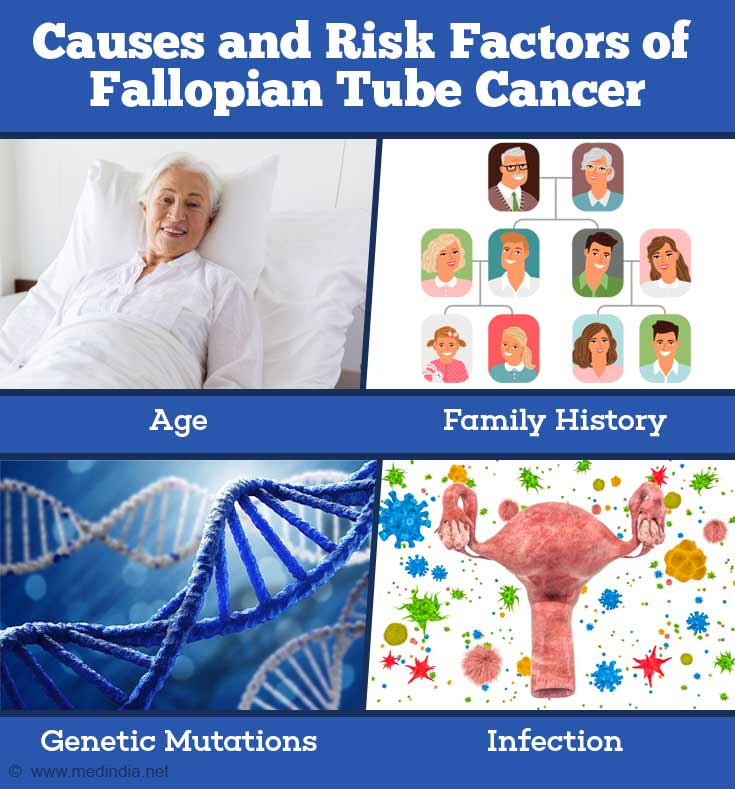
What are the Causes/Risk Factors of Fallopian Tube Cancer?
The exact cause of fallopian tube cancer is not known but several risk factors are known to be associated with an increased incidence of tubal cancer:
- Age – Though it may occur at any age, fallopian tube cancer appears to be more common in women in the age group of 50 to 65 years.
- Parity – It is common in women who have had no children or only a few.
- Family history – Previous occurrence of tubal cancer in a close relative such as mother, sister or daughter increases the risk for the cancer.
- Genetic mutations – Presence of mutations in certain genes such as BRCA1 gene (also associated with risk of breast and ovarian cancer), or the gene associated with HNPCC (hereditary nonpolyposis colorectal cancer), also referred to as Lynch syndrome, increase the risk for fallopian tube cancer.
- Infection – Chronic infection of the reproductive tract may increase risk of tubal cancer, although this risk factor is not well established.
Factors that might reduce the risk of tubal cancer include use of oral contraceptive pills, and delivering and breastfeeding more children.
What are the Symptoms and Signs of Fallopian Tube Cancer?
Fallopian tube cancer may not cause any symptoms or may be associated with vague or non-specific symptoms. The symptoms vary from person to person and may include one or more of the following:
- Abnormal vaginal bleeding, especially bleeding that occurs after menopause
- Abdominal or pelvic pain or discomfort. The pain may be dull or may appear as a colic
- Abnormal vaginal discharge that may be white, clear or tinged with pink due to the presence of blood
- Swelling or lump in the pelvic region
- Swelling of the abdomen due to accumulation of fluid (ascites) in the late stages

What are all Stages of Fallopian Tube Cancer?
Staging system for any cancer is employed by the treating clinician to determine the extent of the cancer, the best treatment options and the likely outcome of treatment for the patient. This information is determined by imaging studies such as CT-PET and MRI scans that give precise information regarding extent and spread of the cancer.
The American Cancer Society (ASC) staging system is used to stage fallopian tube cancer. There are 4 ASC stages as follows:
- Stage I: The tumor is confined to one or both fallopian tubes
- Stage II: The tumor involves one or both tubes and has spread to the adjacent pelvic area and/or the uterus, ovary or other pelvic tissues
- Stage III: The tumor involves one or both tubes and the pelvis with spread to the abdominal cavity and/or regional lymph nodes
- Stage IV: The cancer has spread to distant organs such as lung and liver
How to Diagnose Fallopian Tube Cancer?
The diagnosis of tubal cancer may be challenging because the symptoms are usually vague and non-specific, the cancer is rare and finding cancer inside the tube is not always easy. The following steps help to diagnose the cancer:
History – A detailed menstrual and reproductive history, a family history of cancer and other relevant information could indicate the presence of a gynaecological cancer
Physical examination – A general assessment as well as an abdominal examination could detect the presence of a suspicious mass.
Pelvic or internal examination – During a pelvic or vaginal examination, the woman is asked to lie on the examination table with feet drawn close to the body, spreading the knees apart. The doctor inserts a gloved finger into the vagina while simultaneously pressing down on the lower abdomen with the other hand. The examination may reveal an unusual lump or swelling in the reproductive tract, which will require further investigation.
If the above examinations raise the index of suspicion, the following blood test and imaging tests may be recommended to confirm the diagnosis.
CA125 test: This blood test checks the levels of CA125, a protein whose level is elevated in the blood in several gynecologic diseases, which may be cancerous or non-cancerous. A high CA125 level warrants further testing and does not confirm the presence of fallopian tube cancer.
Ultrasound – An ultrasound is a simple non-invasive imaging test using sound waves to look for pathology in the various organs of the body including in the fallopian tube. The probe may be moved over the lower abdomen (pelvic ultrasound) or inserted into the vagina (transvaginal ultrasound).
CT or CAT (computed axial tomography) scans – CT scans provides high resolution images of blood vessels, soft tissue and the bone involvement as well.
MRI (magnetic resonance imaging) scans – MRI is similar to CT scan but provides even better detail of soft tissue involvement.
Biopsy – A CT scan guided biopsy may be performed to obtain a sample of cells from the suspected mass. The skin over the abdomen is numbed with an injection of a local anesthetic agent. The biopsy needle is passed through the abdominal skin and guided to the right spot. The tissue sample thus obtained is then analysed under the microscope to look for presence of cancer cells.

How is Fallopian Tube Cancer Treated?
The following modalities of treatment are usually employed. Treatment will depend on the clinical stage of cancer as described earlier.
Surgery
Surgery, followed by chemotherapy, is the mainstay in the treatment of fallopian tube cancer. The nature of the surgery depends on the stage of the disease. The surgery can done as an open procedure or through minimally invasive laparoscopic surgery. Surgery to treat the cancer may be done during the same operation as the biopsy.
During surgery, the tubes, ovaries, cervix and uterus, including nearby lymph nodes, are removed for extended disease, while only the tubes with the ovary (salpingo-oophorectomy) are removed for an early stage of the disease.
Chemotherapy
Chemotherapy is usually given after surgery for tubal cancer to kill the remaining cancer cells. Platinum based-chemotherapy is most commonly employed in fallopian tube cancer. In some cases, it may be administered before surgery to reduce the size of the tumor.
Radiation Therapy
Radiation therapy is generally not used to treat fallopian tube cancer. It may be used to shrink bulky tumor tissue prior to surgery or after surgery to eradicate residual tumor mass. Occasionally, it may be used if chemotherapy is contraindicated.

How to Prevent Fallopian Tube Cancer?
Since the cause of tubal cancer is not clear, it is not easy to prevent it.
- If there is a family history of tubal or other gynecologic cancer, the woman should be closely monitored to pick up any new growth early.
- Women with BRCA1 gene mutation may opt to undergo prophylactic (preventive) removal of ovaries and tubes to reduce cancer risk
- Use of birth control pills may reduce risk
- Lifestyle changes that may be adopted include the following:
- Eating plenty of fresh fruits and vegetables
- Quitting smoking and reducing alcohol intake
- Exercising regularly and maintaining a healthy body weight
- Reducing stress through regular practice of yoga and meditation