- Ichthyosis - (http://www.nhs.uk/conditions/ichthyosis/pages/introduction.aspx)
- About Ichthyosis - (http://www.niams.nih.gov/health_info/ichthyosis/)
- Ichthyosis vulgaris - (http://www.nlm.nih.gov/medlineplus/ency/article/001451.htm)
- What is Ichthyosis? - (http://www.firstskinfoundation.org/content.cfm/ichthyosis/what-is-ichthyosis/page_id/952)
What is Ichthyosis?
Ichthyosis is a skin disorder in which the individual has thickened, scaly, dry skin. The condition is generally passed on from parents, but it may also develop suddenly in some individuals. In cases where the condition is inherited the symptoms tend to become apparent within the first year of life, sometimes being noticeable at birth. No matter how early the onset is observed, the condition will persist and affect the individual throughout his or her life. Unfortunately, there is no cure from the condition and patients can only turn to treatment and skincare plans to manage and cope with the symptoms of ichthyosis.
Like other inherited conditions, ichthyosis is passed on to offspring through a mutated gene. This specific gene regulates the rate of skin regeneration, which includes the shedding of old skin cells and production of new ones. Because of a mutation in the gene this cycle of shedding and new skin growth goes awry, with old and dead skin cells being shed too slowly or new skin cells being produced too rapidly so the shedding of dead skin cannot keep pace. The result is the dry, scaly and rough skin. Although rare, in some instances the condition may arise on account of certain medical problems like inflammatory, hormonal or malignant disorders. From all of the types of inherited ichthyosis, ichthyosis vulgaris is the most common, affecting around 1 in 250 individuals.
Ichthyosis can show variation in symptoms but almost all types of ichthyosis affect just the skin. In some types the symptoms and extent of area affected may be a lot more severe, but there are also types of ichthyosis in which internal organs are also affected. Inherited ichthyosis is generally categorized based on the gene that is responsible for the condition, but when classified according to the clinical appearance of symptoms there are five categories. These include:
- Ichthyosis Vulgaris - Patients experience dryness of the skin and mild scaling.
- Epidermolytic Ichthyosis or Epidermolytic Hyperkeratisis - Patients afflicted with Epidermolytic ichthyosis will find spiny dark thick scales forming on the skin and the skin may also be prone to blistering under almost any kind of impact or trauma.
- Lamellar Ichthyosis - Thickening of the skin is again present in this variation of ichthyosis, but one would also observe the formation of large, platelike scales.
- Congenital Ichthyosiform Erythroderma. In addition to scaly, dry skin, redness and inflammation are also observed.
- Localized Ichthyosis - In this type of ichthyosis the thickening and scaly appearance of the skin is not present across the entire body, but is restricted to specific regions such as the foot soles or palms of the hand.
What are the Causes of Ichthyosis?
Ichthyosis is almost always inherited and is passed on through mutated genes that may be present in one or both parents. There is also a possibility that the parents may not suffer from ichthyosis, but one of them could still be silently carrying the genetic mutation,. In the rare cases where the condition is not inherited it could develop as a result of a spontaneous mutation in the gene at the time of conception or shortly after. There are over 40 known genes that could cause inherited ichthyosis if they undergo mutation, with the general rule being that any clinical type of ichthyosis can develop if more than a single gene is mutated.
What are the Symptoms of Ichthyosis?
Although the different types of ichthyosis show variation in symptoms, patients who suffer from any type of ichthyosis are likely to experience some of these symptoms:
- Severe dryness of the skin
- Formation of scaly skin
- Thickening of the skin
- Some amount of itchiness of the skin
- Severe scaling on the legs, but it could also affect the torso and arms.
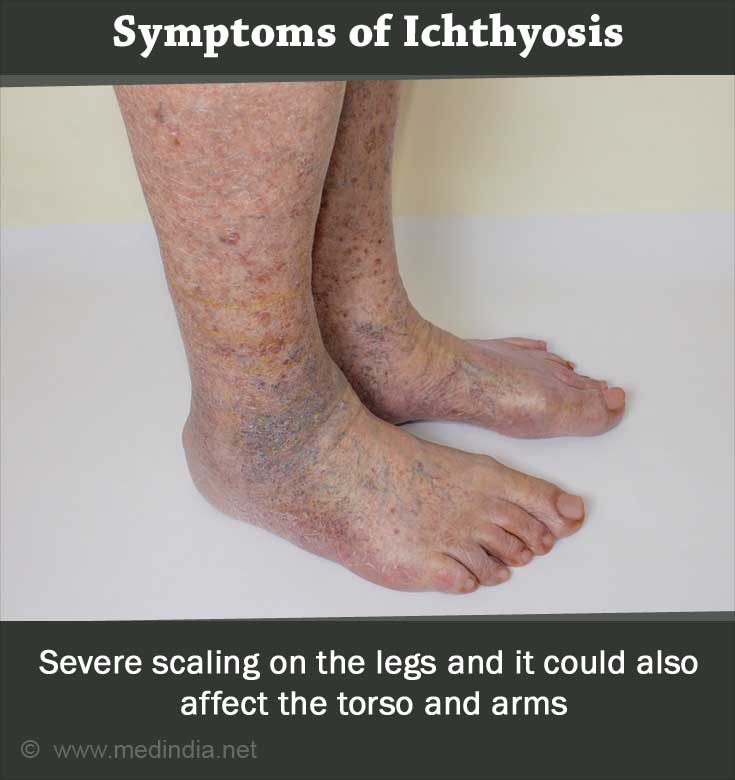
- Formation of lines along the palms.
- Flaking of skin from the scalp, as in the case of dandruff.
- Increased sensitivity of the skin.
- Formation of deep cracks on the skin that may be painful.
In the case of ichthyosis vulgaris, symptoms are usually quite mild, but this is not always the case and at times they could be severe. The severity of these symptoms can also vary greatly among family members, so it is not necessary that the symptoms will be as severe in offspring afflicted with the condition, even though they might be severe in the parent.
The symptoms are a lot more pronounced during winter and in cold dry climatic conditions and will usually resolve to some extent when the weather turns warm and humid.
In severe cases, patients may also experience problems such as:
- The patient’s ability to sweat may be impaired, causing overheating.
- Range of movement may be affected as it becomes difficult and painful to go through certain movements if the skin is affected in that area.
- There is a risk of secondary infections developing because of cracks or splitting of the skin.
- The thickening and buildup of skin around the eyes and ears can even impair audiovisual senses.
How to Diagnose Ichthyosis?
To arrive at a diagnosis your health care provider will need to ask you about your family history of disease and your medical history as well. A physical examination is essential and very often doctors will be able to diagnose the condition based solely on such an examination. To confirm a diagnosis of ichthyosis your doctor may request a blood test or skin biopsy. In some cases, patients may also be advised to undergo genetic testing, although the value in such testing is often questionable because the results do not necessarily direct any specific treatment. Diagnostic tests can help to rule out other conditions that could cause dryness and thickening of the skin.
How do You Treat Ichthyosis?
Ichthyosis is not curable but treatment with an appropriate skin care routine can offer relief from the symptoms. A customized skin care routine for ichthyosis should include regular moisturizing and exfoliating of the skin. In most cases, a dermatologist will make specific recommendations or prescribe certain ointments, creams and lotions or bathing oils. When applying emollient to the skin keep in mind:
- Try to apply an emollient soon after having a bath or shower as this well help to retain moisture.
- Use a pumice stone to get rid of some of the thickened dead skin, by rubbing it gently against the skin when wet.
- To get rid of flakes of skin present on the scalp, brush your hair gently after it has been washed.
- It may also help to use other exfoliating or moisturizing products. Lanolin creams and other ointments or creams that contain alpha hydroxy acids, urea, and lactic acid are worth considering.
- Patients may also be advised to use ointments and creams containing salicylic acid for an exfoliating effect on the skin. Salicylic acid containing creams may cause irritation in sensitive skin however.

While mild cases may just require some amount of additional skin care, things are quite different when dealing with severe cases of ichthyosis. With severe icthyosis, symptoms can surface at any time and patients need to spend several hours a day just taking care of their skin.
Depending on the severity of symptoms and risk of other complications, doctors may also recommend treatment with antiseptics or antibiotics to prevent or treat any skin infection. Retinoid tablets are prescribed in many cases to reduce the growth and thickening of scaly skin. This does not help to bring about any reduction in inflammation or redness however.
What are the Complication and Risks of Ichthyosis?
While ichthyosis is a purely physical affliction, the symptoms can be so severe and have such a profound impact on one’s appearance that there can also be psychological fallout. In almost all cases the condition is disfiguring to some extent and to make matters worse patients often face some amount of social stigma. Social attitudes stem from a lack of knowledge about the condition and a natural fear that is associated with such unknown conditions. As a consequence patients tend to suffer from isolation, low self-esteem, depression and social anxiety disorders.
In cases where the skin condition causes itching, patients may involuntarily scratch at the surface and there is a risk of bacterial infections developing.
 MEDINDIA
MEDINDIA

 Email
Email





