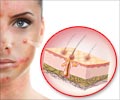
A new genetically modified protein developed by scientists reverses the skin disorder vitiligo in mice.

I. Caroline Le Poole, PhD, and colleagues describe the modified protein in the journal Science Translational Medicine. Le Poole is a professor in Loyola's Oncology Institute and in the departments of Pathology and Microbiology and Immunology.
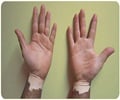
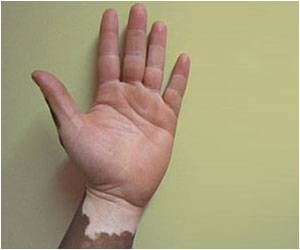
About 1 million Americans have vitiligo, and the condition affects about 1 in 200 people worldwide. Vitiligo is most noticeable in people of color, but also can be distressing to Caucasians. Vitiligo is an autoimmune disease, in which the immune system goes into overdrive and kills pigment cells, which give skin its color.
Previous studies have found that a protein called HSP70i plays a vital role in the autoimmune response that causes vitiligo. (HSP70i stands for inducible heat shock protein 70.)
HSP70i consists of 641 building blocks called amino acids. Le Poole and colleagues genetically modified one of these amino acids to create a mutant HSP70i. This mutant protein supplants normal HSP70i, thereby reversing vitiligo's autoimmune response.
Resarchers Jeffrey A. Mosenson and Andrew Zloza gave mutant HSP70i to mice that developed vitiligo, and the results were striking. Mouse fur - affected by vitiligo -- had the coloring of a salt-and-pepper beard. But when the mice were vaccinated with mutant HSP70i, the fur turned black.
Some of the effects seen in mice also were seen in human skin specimens.
Le Poole and colleagues wrote that mutant HSP70i "may offer potent treatment opportunities for vitiligo."
The study was supported by a NIH/National Institute of Arthritis and Musculoskeletal and Skin Diseases grant to Le Poole.
Authors of the study are Jeffrey A. Mosenson, Andrew Zloza, John D. Nieland, Elizabeth Garrett-Mayer, Jonathan M. Eby, Erica J. Huelsmann, Previn Kumar, Cecele Denman, Andrew T. Lacek, Federick J. Kohlhapp, Ahmad Alamiri, Tasha Hughes, Steven D. Bines, Howard L. Kaufman, Andreas Overbeck, Shikhar Mehrotra, Claudia Hernandez, Michael I. Nishimura, Jose A. Guevara-Patiño and I. Caroline Le Poole.
Work on this study was performed primarily in the laboratories of Guevara-Patino and Le Poole at Loyola University Chicago Stritch School of Medicine. Other institutions involved in the study are Rush University Medical Center, Aarhus University in Denmark, Medical University of South Carolina, Illinois Math and Science Academy, University of Chicago, University of Illinois at Chicago and Lumiderm in Madrid, Spain.
Source-Newswise
 MEDINDIA
MEDINDIA


 Email
Email