- Information About Biliary Atresia - (http://www.liverfoundation.org/abouttheliver/info/biliaryatresia)
- What Is Biliary Atresia? - (https://www.cincinnatichildrens.org/health/b/biliary)
- Biliary Atresia - (https://www.niddk.nih.gov/health-information/liver-disease/biliary-atresia)
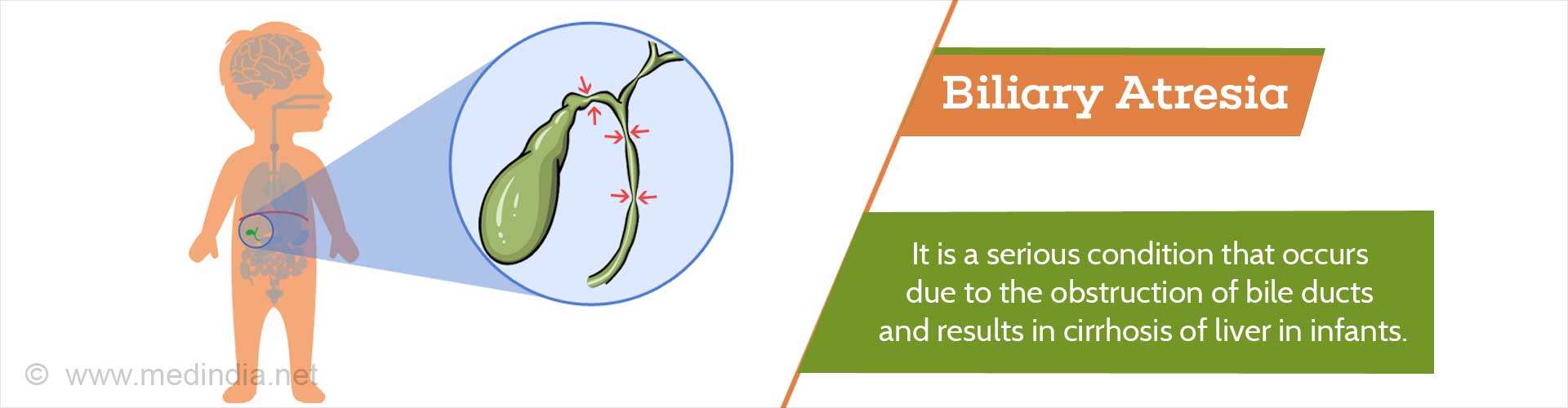
What is Biliary Atresia?
Biliary atresia is a congenital or acquired defect in the biliary transport system that occurs at birth or in a few weeks after birth. Bile produced by the liver is carried via ducts to the intestine to help in the digestion of fats. The ducts present in the liver are called intra-hepatic ducts and the ones present outside the liver are called extra-hepatic ducts.
Biliary atresia is characterized by the absence of extra-hepatic ducts. This leads to failure in transport of bile presenting as jaundice. The bile then accumulates in the liver thereby damaging the liver cells due to inflammation and portal hypertension. The liver undergoes scarring and fibrosis due to the stasis of bile and shrinks with time. This irreversible shrinking is called cirrhosis and can be life-threatening. The child needs a liver transplantation in due course to survive.
What are the Types of Biliary Atresia?
Based on the onset of disease, biliary atresia is classified as fetal and perinatal. In the fetal type, the biliary duct obstruction occurs during pregnancy in-utero. While the perinatal type occurs after birth due to either infection or toxin exposure.
Based on the site of obstruction, biliary atresia is classified into three types, Types I, II and III. Type III is the commonest and is seen in more than 90% of the cases.
What are the Causes of Biliary Atresia?
The cause of biliary atresia remains unclear till date. It is very clear that it is not transmitted by the parents to the child. Research suggests that it is caused either
a. due to a viral infection at birth or in the womb, or
b. exposure to toxic substances leading to the damage of the biliary ducts.
The disease cannot spread from one child to another and also the affected child cannot transmit the disease to his children in later life. In as many as 10 to 15 per cent infants the disease is associated with other system disorders like the heart and blood vessels, the spleen and intestine. Hence an infant with biliary atresia should be investigated for other system disorders. This behavior also points to a possible mutation being the cause of the disease as it affects multiple system development. Research is ongoing to find whether mutation is the cause.
What are the Symptoms of Biliary Atresia?
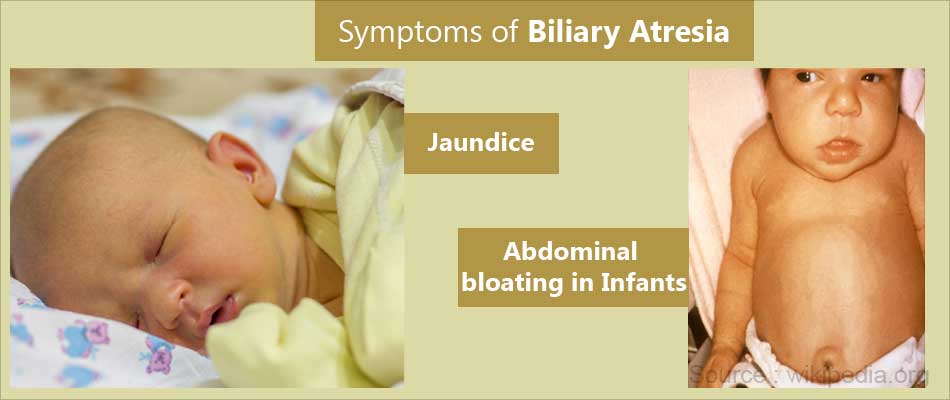
Biliary atresia affected infants are completely normal for the first two weeks of their life. After two weeks, they slowly develop jaundice, i.e. yellowish discoloration of the skin and sclera of the eyes. This is due to accumulation of bile in the liver. The urine passed by the infant is dark yellow colored and the stools are clay colored. Jaundice is common in the first two weeks of life and can be easily treated. But sudden appearance of jaundice or continued jaundice after two weeks of birth should alarm the parents and the doctor. The infant should then be investigated for biliary atresia.
Due to collection of bile in liver, the liver gets inflamed and swollen. This leads to abdominal bloating or distension in the infant. There is increased itching due to excess bile which makes the infant irritable. Due to continued inflammation and poor digestion, the infant progressively loses weight and appears ill and toxic.
How do you Diagnose Biliary Atresia?
Varied tests are required to arrive at a diagnosis of biliary atresia.
- Blood tests – To assess liver function and levels of bilirubin (bile pigment) in blood. They also help to rule out any associated infection.
- X-ray of abdomen – To diagnose enlarged liver and / or spleen.
- Ultrasound of the abdomen – It is a noninvasive simple procedure to evaluate the liver status. The test helps to examine the size of liver, the status of bile ducts and the gall bladder (the organ that stores bile).
- Liver biopsy – This is an invasive procedure in which a needle is inserted into the abdomen of the infant under ultrasound guidance. Small bits of liver tissue are extracted and studied under the microscope. The microscopic picture confirms the diagnosis of the disease.
- Diagnostic Surgery – In cases where the diagnosis remains unclear even after biopsy and the infant is becoming progressively ill, diagnostic surgery is advised. The surgeon explores the abdomen and traces the path of the bile ducts from the liver to the intestine. This helps in identifying the exact problem.
- Operating cholangiogram – During diagnostic surgery, the surgeon injects a dye into the gall bladder and a series of X-rays are taken. The dye being radio-opaque can be easily visualized on an X-ray. If the dye does not travel to the intestine, it indicates that the ducts are blocked confirming biliary atresia. If the dye travels normally, the disease is ruled out and other liver disorders are investigated.
How do you Treat Biliary Atresia?
There is no medical treatment available for treating biliary atresia. It requires timely surgery to prevent cirrhosis of the liver.
The treatment of choice is Kasai procedure or hepatoportoenterostomy. Kasai procedure is a surgical procedure to establish a communication between liver and intestine for drainage of bile in cases where the bile duct is obstructed.

The surgeon attempts to establish a transport route for bile from liver to the intestine by utilizing small patent ducts. A loop of the intestine is brought in contact with the ducts and biliary drainage pathway is re-established. The success rate of the procedure ranges from 60 to 80% and the time of surgery determines the success rate. The best prognosis is obtained if the procedure is conducted by 3 months of age. This underscores the significance of timely diagnosis and prompt surgery.
In cases where Kasai procedure turns out to be unsuccessful, the only option left is liver transplantation. The biggest challenge in transplantation is the availability of donors in this age group.
How do you Prevent Biliary Atresia?
Biliary atresia is not a preventable disorder. But early diagnosis and timely intervention can help save many lives. A keen eye on the onset of jaundice after two weeks of birth can help in parent’s seeking medical care for the child. With advancements in technology, diagnosis is simple and the liver can be salvaged by surgical techniques effectively.
Health Tips
Biliary atresia causes malnutrition due to poor digestion and absorption. Hence infants require nutritional supplements to overcome this deficit.
In cases where transplant is required, infants are given strong drugs to suppress their immunity. The drugs prevent rejection of the transplanted liver, but make the infant susceptible to a variety of infections. Hence special attention to hygiene and nutrition is essential.