- Hohoff A, Joos U, Meyer U, Ehmer U, Stamm T. The spectrum of Apert syndrome: phenotype, particularities in orthodontic treatment, and characteristics of orthognathic surgery. Head & Face Medicine20073:10 DOI: 10.1186/1746-160X-3-10
- Apert syndrome - (https://ghr.nlm.nih.gov/condition/apert-syndrome#diagnosis)
- FGFR-Related Craniosynostosis Syndromes - (https://www.ncbi.nlm.nih.gov/books/nbk1455/#craniosynostosis.diagnosis)
- What is Apert Syndrome ? - (http://www.faces-cranio.org/disord/apert.htm)
- About Apert Syndrome - (https://rarediseases.org/rare-diseases/apert-syndrome/)
What is Apert Syndrome?
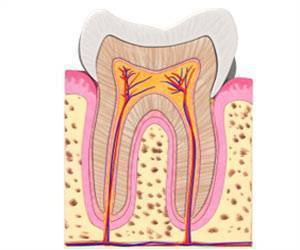
Apert syndrome or acrocephalosyndactyly is a genetic disorder marked by early fusion of skull bones resulting in abnormal shape of the face and the head. Fusion of fingers and toes (syndactyly) is also noted.
Apert syndrome is a rare condition affecting 1 in 160,000-200000 births. Child specialists and clinicians should be aware and recognize the condition for prompt management. Left untreated, the brain development can get affected resulting in significant morbidity.
The condition was described back in 1842 by Baumgartner but the eponymic credit goes to the French pediatrician Eugene Apert who first presented the condition in 1906.
What is the Cause of Apert Syndrome?
As mentioned previously, Apert syndrome is a genetic disorder due to an alteration or mutation in a specific gene.
In Apert syndrome, the defect has been found to be in the fibroblast growth factor receptor 2 (FGFR2) gene. This gene encodes a protein called FGFR2. One of the many functions of this protein is to cause immature cells to become bone cells during fetal development. At least seven mutations in the FGFR2 gene found to cause Apert syndrome.
Due to the mutation, the normal function of the protein becomes affected leading to premature fusion of the skull bones (craniosynostosis) and other defects.
The condition is autosomal dominant i.e, one copy (out of 2) of the defective gene is sufficient to cause the abnormality in the offspring.
Most new cases described occur in babies with no previous family history of the condition i.e occur sporadically. The reason for the mutation is not known but advanced paternal age has been implicated as one of the risk factors.
What are the Symptoms and Signs of Apert Syndrome?
Most of the clinical features of Apert syndrome result from premature fusion of the skull bones. The hands and feet and other organs are also involved to varying degrees. The various clinical features include:
Face and skull
- Sunken appearance of the face (midface hypoplasia)
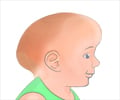
- Broad skull
- Abnormally pointed head at the top with prominent forehead
- Widely spaced eyes (hypertelorism)
- Abnormally bulging eyes (exophthalmos)
- Flat face with right and left asymmetry
- Flat nose with a low bridge
- Narrowed opening between nose and throat affecting swallowing and breathing
- Narrow roof of mouth or palate
- Cleft palate with a bifid uvula
- Protruding lower jaw
- Crowding of teeth
- Bad bite due to malocclusion of teeth

Upper and lower limbs
- Unusually broad thumbs and big toes
- Short digits of hands and feet with partial or complete fusion (syndactyly)
- Mitten-like syndactyly due to complete fusion of 2-4th fingers with a single common nail
- Fusion of bones of the wrist
Other organs
- Chronic ear infections and hearing loss
- Hole in the wall of the ventricle
- Tracheal cartilage defects affecting breathing and swallowing
- Narrow gastric outlet with potential for obstruction
- Obstruction of the food pipe
- Malposition of the anal opening
- Failure of descent of testes into the scrotum in males
- Obstruction of the vagina in females
- Enlarged kidneys
- Fusion of the vertebral bones of the neck
- Moderate-to-severe acne
- Varying degrees of mental retardation
How do you Diagnose Apert Syndrome?
1. After birth
Physical examination:
In most cases, the diagnosis may be suspected at birth by recognizing the characteristic abnormalities followed by a thorough physical examination and confirmed by other tests.
Imaging tests:
The diagnosis may be confirmed by diagnostic imaging including CT, MRI scan and echocardiogram to determine the presence of other abnormalities such as skeletal and heart defects.
Genetic analysis
Genetic or molecular testing may be done to localize the defect in the FGFR2 gene. Incidentally there are 8 craniosynostosis syndrome types including Apert syndrome related to defects in the FGFR2 gene.

2. Before birth
In a high-risk pregnancy e.g. presence of family history of the disorder or advanced paternal age, prenatal testing may be requested for the purpose of pregnancy termination at an early stage. In sporadic cases, the prenatal ultrasound may reveal findings suspicious for a craniosynostosis disorder, warranting further testing.
Imaging tests
Prenatal diagnosis and pre-implantation genetic diagnosis (PGD) in high-risk pregnancies may be done if there is a prior family history of Apert syndrome.
Prenatal ultrasound may show suspicious findings such as abnormal bi-parietal diameter (BPD) and enlarged ventricles of the brain.
Further imaging by MRI may reveal underlying brain abnormalities such as absence of corpus callosum, hydrocephalus (causing increased BPD) or a clover leaf skull.
Genetic testing
DNA testing for the affected fetal gene may be done in case of a prior family history of the disorder.
How do you Treat Apert Syndrome?
Standard Therapies
The treatment of Apert syndrome aims at addressing the specific symptoms that may be present in the particular individual. Treatment is usually symptomatic and supportive.
- Craniosynostosis and associated hydrocephalus in some cases may give rise to an abnormally increased pressure within the skull (intracranial pressure) and on the brain. In these cases, early surgery (within 2 to 4 months after birth) becomes necessary to correct the defects in the skull and facial bones.
- Insertion of a tube (shunt) to drain excess cerebrospinal fluid (CSF) away from the brain and into another part of the body like the abdomen where the CSF can be absorbed can be done to relieve associated hydrocephalus (fluid accumulation in the brain).
- Early repair and reconstructive surgery may also be done in some infants with Apert syndrome to address craniofacial abnormalities.
- Other defects such as those of heart, eye and ear defects may also need correction.
Advancements in craniofacial surgery have helped children with Apert syndrome to attain their full potential by increasing the chances for brain growth, improving their physical appearance, and in gaining social acceptance.
Children with Apert syndrome still face mistaken notions of mental retardation and social stigmatization because of their facial appearance. It is extremely critical for families and health care providers to help in fostering their adjustment and supporting them during these psychologically trying times.
Thus, a coordinated effort by a team of professionals and family is necessary to draw up the best and optimal plan to help the child’s all round development and lead a near normal and productive life.
 MEDINDIA
MEDINDIA

 Email
Email