A new study reveals that one-third of older adults admitted to the intensive care unit (ICU) were frail, increasing the risk of death, illness and adverse events.
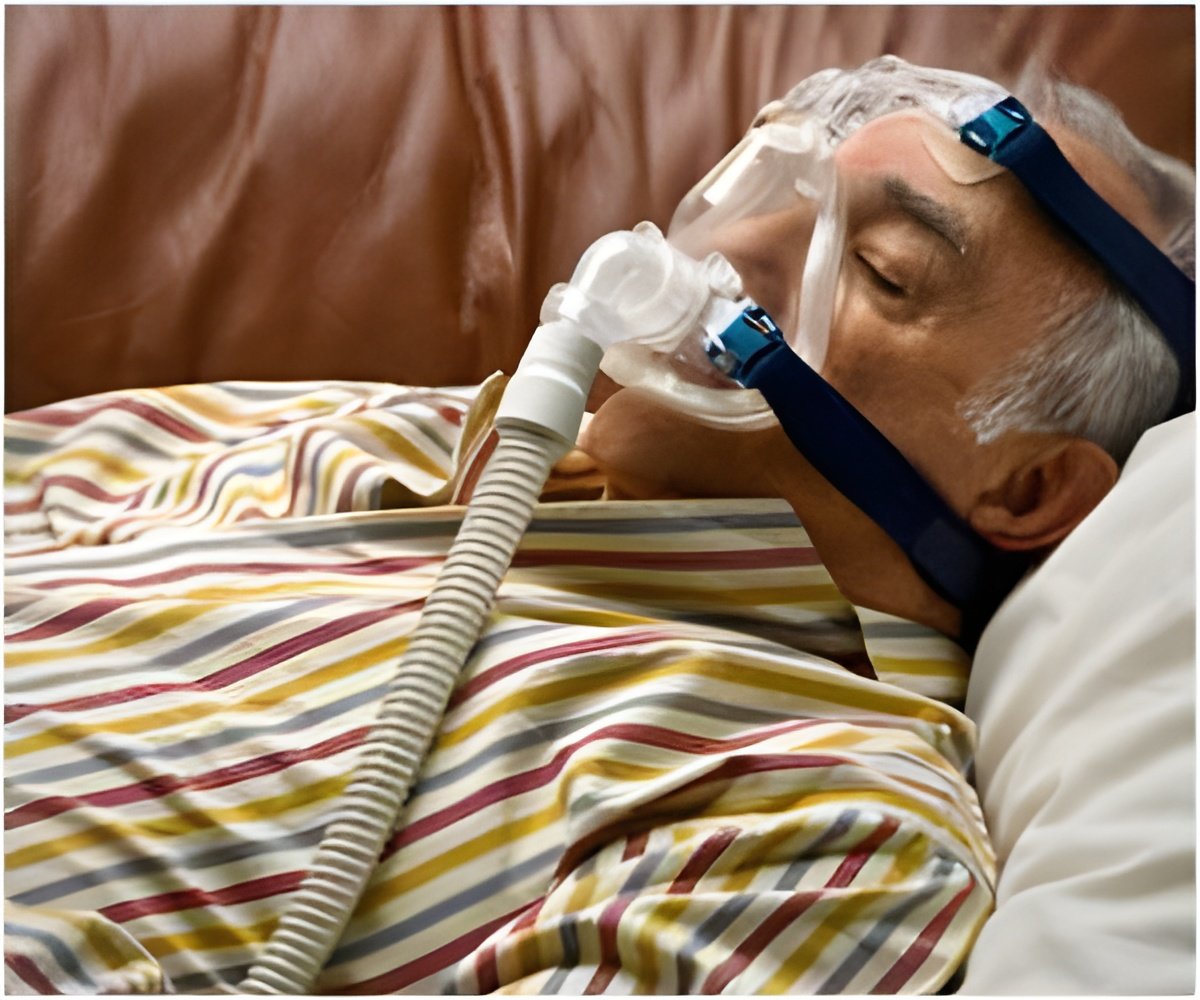
A study of 421 critically ill adults aged 50 years and over in ICUs at 6 hospitals in Alberta, Canada, found that 33% of patients were considered frail based on the Canadian Study on Health and Aging Clinical Frailty Scale (CFS). The mean age of the patients was 67 years, 39% were women, and most (95%) were living at home independently or with help. In addition to being older, frail patients had multiple illnesses and fewer social supports compared with patients who were not frail.
"Despite both groups having similar treatment intensity, frail patients were more likely to experience adverse events, had longer lengths of stay in ICU and hospital, and were more likely to die while in hospital and within 12 months after admission," writes Dr. Sean Bagshaw, Division of Critical Care Medicine, Faculty of Medicine and Dentistry, University of Alberta, with coauthors. "Among survivors, frail patients were more likely than nonfrail patients to have new functional dependence at hospital discharge and had higher rates of hospital readmission."
"Our findings suggest that routine assessment of frailty could provide more accurate prognostication and identify a vulnerable population that might benefit from follow-up and intervention," conclude the authors.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email





