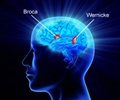
A team of neuroscientists is revivifying NMDA receptor antagonists, who have an anti-stroke potential, by minimizing their side effects.
Senior author Stephen Traynelis at Emory University School of Medicine said, "We have found neuroprotective compounds that can limit damage to the brain during ischemia associated with stroke and other brain injuries, but have minimal side effects. These compounds are most active when the pH is lowered by biochemical processes associated with injury of the surrounding tissue. This is a proof of concept study that shows this mechanism of action could potentially be exploited clinically in several conditions, such as stroke, traumatic brain injury (TBI) and subarachnoid hemorrhage."
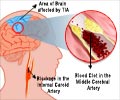
In brain tissue affected by stroke or TBI, the environment becomes more acidic because of the lack of oxygen and the buildup of metabolites such as lactic acid. Additionally, NMDA receptors get overstimulated by an increase in the neurotransmitter glutamate, enough to kill cells. Researchers reasoned that the NMDA receptor antagonists whose activity is dependent on acidic conditions should, at the right dose, be active only in the injured areas of the brain.
The results have been published in Neuron.
Source-Medindia
 MEDINDIA
MEDINDIA
 Email
Email