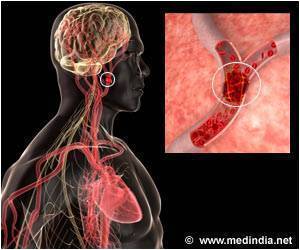
Endovascular treatment may not be superior to intravenous treatment for stroke.
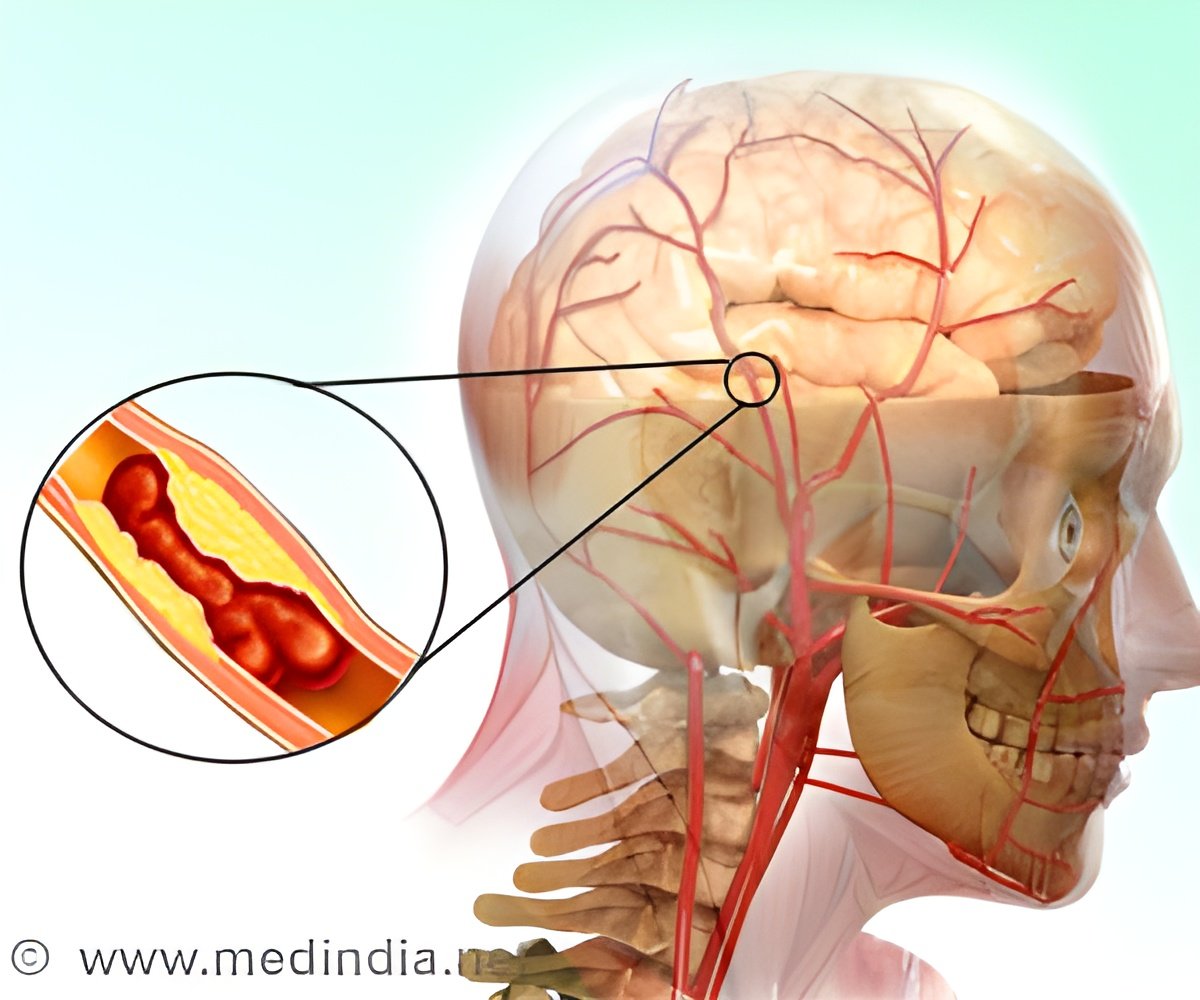
Stroke arises due to sudden obstruction in blood
flow to a part of the brain. The obstruction is often due to a clot in
important blood vessels. The treatment in such cases is to break the clot with
medications and allow the free flow of blood. This has often been achieved by
injecting drugs like recombinant tissue plasminogen activator (t-PA) into the
veins, through which it goes to the site of obstruction and breaks the clot.
Intravenous therapy (injecting the drug through the
vein) has been associated with side effects like bleeding. In addition, it has
to be administered within 3 to 4.5 hours of the stroke. Therefore, endovascular
revascularization techniques have been adopted in the recent years to overcome
some of the difficulties of intravenous treatment. These techniques deliver the
drug at the site of the block and therefore prevent widespread bleeding. They
are also effective even after 3 hours following a stroke and therefore can be
used when the patient reaches the hospital a little late.
But is endovascular revascularization more effective
than intravenous treatment? Maybe not, according to a recent study published in
the
New England Journal of Medicine.
The study was conducted on 362 stroke patients
between the ages of 18 and 80 years undergoing either of the procedures.
The study found that endovascular treatment
was not superior to intravenous t-PA in terms of being alive without disability
at the end of three months. The incidence of side effects, especially with
respect to bleeding within the brain, was similar in the two groups.
The study thus concluded that based on the outcomes,
both the procedures are similar and it is not possible to proclaim one superior
over the other.
Thus, it is not necessary to prefer endovascular
procedures which are more expensive and require more expertise to the
conventional intravenous treatments. However, the researchers do not deny that
it is possible that newer devices used for endovascular treatment could provide
added benefits.
Reference:
Advertisement
1. Endovascular Treatment for Acute Ischemic Stroke; Alfonso Ciccone, et
al; NEJM 2013
Source-Medindia