Drug hydroxyurea proven effective for sickle cell anemia treatment in adults and children was found to reduce hospitalizations and cut annual estimated medical costs by 21 percent, says report.

"We estimate that hydroxyurea cut overall annual medical expenses about $3,000 for each patient by helping patients avoid disease complications that require inpatient hospital care," said Wang, who is first and corresponding author of the Pediatrics study. "We expect those savings will grow along with patients, whose symptoms often increase in severity and frequency as they age."
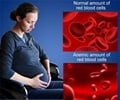
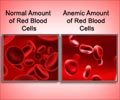
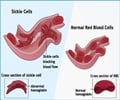
About 100,000 individuals in the U.S. and millions worldwide have sickle cell disease, which leaves them at risk for premature death and disability. The disease is the most common genetic disorder affecting African-American individuals, but those from other ethnic and racial backgrounds also inherit mutations in the hemoglobin gene. The mutations result in blood cells that are prone to assuming the sickled shape that gives the disease its name and that leave patients at increased risk for episodes of acute pain, stroke, organ damage and other complications.
The analysis comes two years after Wang and his colleagues reported that hydroxyurea reduced episodes of acute pain and pneumonia-like illness, eased other symptoms, reduced the need for blood transfusions and cut hospitalizations for infants and toddlers with sickle cell anemia. Sickle cell anemia is the most common and severe form of sickle cell disease.
Earlier studies had demonstrated that adults and adolescents with the disease benefited from hydroxyurea. BABY HUG showed the drug, which is inexpensive and easy to administer, was safe and effective for young children. The study involved 193 children who were 9 to 18 months old when they enrolled at one of the 13 participating medical centers. The children were randomly assigned to receive either a daily dose of hydroxyurea for two years or an inactive look-alike.
Continued concern about U.S. health care spending prompted BABY HUG researchers to retrospectively assess hydroxyurea's impact on treatment costs. Investigators used a national database of Medicaid expenditures to estimate the 2009 cost of caring for BABY HUG participants. Medicaid is the state-federal health insurance program that covers lower income and disabled children and adults. The six-year BABY HUG study ended in 2009.
Wang said actual savings associated with hydroxyurea treatment are likely greater, since medical costs are roughly 25 percent less for children enrolled in Medicaid than for those with private health insurance. The analysis was unable to capture all treatment-related costs. "The analysis also could not capture the anxiety patients and family experience when children must be hospitalized," Wang said.
The drug works by increasing production of fetal hemoglobin, a form of the oxygen-carrying protein that is unaffected by the mutations that cause sickle cell disease. Fetal hemoglobin normally drops dramatically after birth. Hydroxyurea, however, increases production of red blood cells that contain that form of hemoglobin.
The drug remains an underutilized treatment for sickle cell anemia. Wang estimated the drug is prescribed to about 30 percent of pediatric patients nationwide and an even smaller percentage of adults. Work is underway at St. Jude and other medical centers to identify and address barriers to more widespread use of the drug, including lingering concerns about possible long-term toxicity.
The senior author is Scott Grosse of the U.S. Centers for Disease Control and Prevention (CDC). The other authors are Suzette Oyeku, Montefiore Medical Center, Bronx, N.Y.; Zhaoyu Lou, Billie Fish and Bruce Thompson, all of Clinical Trials and Surveys Corp., Owings Mills, Md.; Sheree Boulet, CDC; Scott Miller, SUNY-Downstate Medical Center/King's County Hospital Center, Brooklyn; and James Casella, Johns Hopkins University School of Medicine, Baltimore.
The research was funded in part by the National Heart, Lung, and Blood Institute and the National Institute of Child Health and Human Development.
Source-Newswise
 MEDINDIA
MEDINDIA


 Email
Email