An American research team has found that retinal detachment, a condition that puts an individual at risk for vision loss or blindness, can be treated with using one of three currently
An American research team has found that retinal detachment, a condition that puts an individual at risk for vision loss or blindness, can be treated with using one of three currently available surgical techniques.
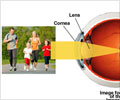
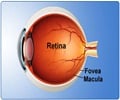
"Although no randomized trials have been conducted that show definitively that one procedure is best for every situation, improvements in these surgical techniques have led to effective treatments for most patients," says Dr. Donald J. D'Amico, ophthalmologist-in-chief at NewYork-Presbyterian Hospital/Weill Cornell Medical Center, professor and chairman of ophthalmology at Weill Cornell Medical College, and an international leader in vitreoretinal surgery.Retinal detachment can occur when holes, tears or breaks appear in the light-sensitive retina as a result of trauma or pulling away of the gelatinous mass, known as the vitreous, that fills the back of the eye.
Though retinal tears occur most often in adults over age 60, they may occur much earlier, especially among people with high myopia.
The sudden onset of light flashes and "floaters" may signal an impending retinal detachment.
Dr. D'Amico has revealed that there are three surgical options that can be used to treat retinal detachment, namely scleral buckling, pneumatic retinopexy, and vitrectomy
In scleral buckling. a piece of silicone is sutured onto the outside wall of the eyeball and left in place permanently to create an indentation, or buckle, that restores contact with the detached retina. The individual tears are then closed by a localized scar that is induced with a freezing probe or laser.
Advertisement
Pneumatic Retinopexy is a newer and less invasive procedure than scleral buckling that involves injecting a gas bubble into the vitreous cavity of the eye, and then positioning the patient's head so that the bubble floats to the break in the detached retina. It allows the natural forces in the eye to reattach the retina, and the break is permanently sealed by the application of a freezing probe or laser to create a scar around the break.
Advertisement
Vitrectomy is a surgery within the eye in which the vitreous gel is removed, Since vitreous traction is the typical cause of the retinal tears in a detachment, this approach has the advantage of directly attacking the underlying cause of the detachment. It is a newer surgery than scleral buckling, and is continually improving due to innovations in instrumentation and technique.
D'Amico notes that vitrectomy for detachment may be associated with a higher risk of postoperative cataract, and this appears to be its main disadvantage compared to buckling, which has lower risk of cataract but higher risk of other complications.
According to the researcher, in cases where bleeding in the vitreous gel is present with the detachment, a vitrectomy approach is clearly preferred to remove the vitreous hemorrhage in order to gain better visualization to find and repair tears or holes in the retina.
For the patient described in the vignette who went to his ophthalmologist with classic symptoms of primary retinal detachment, including flashing lights, floaters and progressive loss of vision, Dr. D'Amico's first recommendation would be to perform a pneumatic retinopexy.
"I would select this option for this patient because this specific detachment is well-suited to pneumatic retinopexy by virtue of the retinal breaks being located close together in the superior retina, which is the easiest location to treat with an intraocular gas bubble. Furthermore, the procedure can be done immediately in the doctor's office at lower cost and with fewer risks of complications, compared to buckling or vitrectomy, and it also compares quite favorably with the other procedures with having a 75 percent chance of restoring vision to 20/50 or better after this minimally invasive procedure," Dr. D'Amico says.
Dr. D'Amico admits that there are risks associated with each of the three surgical techniques.
"The benefits of surgery, however, far outweigh the risks. No matter which procedure the surgeon chooses, there is a very good chance today that a patient's retina can be reattached and his or her vision preserved," says Dr. D'Amico, who performs all of these procedures.
Source-ANI
SRM