Recent study says that pregnant women are at higher heart attack risk.
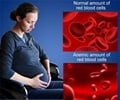
The analysis found that most pregnant women did not present with traditional cardiovascular risk factors, such as high blood pressure, diabetes or high cholesterol levels, yet they tended to have more serious heart attacks. In fact, the death rate in these women was 7 percent, which is two to three times higher than what is expected in non-pregnant patients of the same age. In addition, heart attacks in most of these women were caused by different mechanisms than those occurring in the non-pregnant general population.
"Despite advances in the management of myocardial infarction, we found that the rate of severe complications including heart failure, cardiogenic shock, and maternal or fetal mortality continues to be high among pregnant women compared to others," said Uri Elkayam, MD, professor of medicine at the University of Southern California in Los Angeles and the study's lead investigator. "Therefore, every effort should be made for early diagnosis and appropriate treatment of pregnancy-associated acute myocardial infarction. We believe this study provides important information that can help guide clinicians, and hopefully improve the care of these patients."
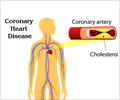
While atherosclerosis—or a narrowing of the arteries due to fatty build-up—is the most common cause of heart attacks in the general population, this was only the cause in one-third of pregnant women. More common among pregnant women was coronary dissection, a separation of the layers of the artery wall that blocks normal blood flow. This is very rare in non-pregnant patients and is thought to occur during and immediately after pregnancy because of the weakening of the wall of the coronary arteries. Researchers also found that coronary dissection may actually be worsened by blind use of guideline-recommended standard therapies such as thrombolytic therapy.
"We have very clear guidelines for treating myocardial infarction in the general population. These guidelines, however, may not always apply to women with pregnancy-associated heart attacks, and may actually cause more harm than good," said Dr. Elkayam. "It is, therefore, important to identify the cause of heart attack in pregnant women before deciding what therapies to use."
In particular, he said coronary angiography to identify the mechanism of heart attack and guide therapy is recommended in high-risk patients when urgent treatment is needed. At the same time, however, in several patients coronary dissection was reportedly caused by coronary angiography or angioplasty and led to either death, a need for extensive stenting or coronary bypass surgery. For this reason, Dr. Elkayam advises that stable and low-risk women with pregnancy-associated heart attack be treated conservatively.
This analysis included 150 cases published in the literature or consulted by the research team since 2005 and builds upon previous analysis of another 228 cases prior to 2005. More positively, maternal mortality has been decreasing steadily since the first survey, dropping from 16 percent prior to 2005 to 7 percent after 2005.
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email