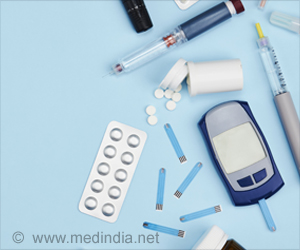
Opioid-related overdose deaths involving another substance is now the norm, not the exception, in Massachusetts, according to a new study.
TOP INSIGHT
Social barriers influencing patients with multiple substance use disorder like homelessness, mental health issues, and addiction need to be addressed adequately at an early stage.
Read More..
BMC collaborated with the Massachusetts Department of Public Health and analyzed opioid-related overdose deaths in the state from 2014 to 2015 using data from the Massachusetts Public Health Data Warehouse, which links data from various state agencies at the individual level. They examined postmortem toxicology data to identify the drugs present at the time of death and grouped into three categories - opioids only; opioids and other substances not including stimulants; and opioids with stimulants, with or without other substances.
During the two year period studied, there were 2,244 opioid-related overdose deaths in Massachusetts with toxicology results available. Seventeen percent of those deaths had only opioids present, 36 percent had opioids and stimulants (primarily cocaine), and 46 percent had opioids plus other substances, but not stimulants. The data also indicated that individuals over the age of 24, non-rural residents, those with co-morbid mental illness, non-Hispanic black residents, and those with recent homelessness were more likely to have opioids and stimulants, such as cocaine or methamphetamine, in their systems at their time of death than opioids alone.
"As a provider, these findings indicate a pressing need to address and treat not just opioid use disorder, but other substances that patients are misusing," said lead author Joshua Barocas, MD, who also is an infectious disease physician at BMC and assistant professor of medicine at BU School of Medicine. The challenge, he says, is that while there are FDA-approved medications to treat opioid use disorder, there are not effective medications to treat other substances, such as cocaine or amphetamines.
Additionally, the data clearly shows that untreated mental illness and social determinants of health are risk factors for overdose death. Specifically, those who are homeless or have mental illness are more likely to use opioids and stimulants, and more work is needed to identify ways to better engage these individuals in care. "To truly make a difference in reducing opioid overdose deaths, we must tackle issues such as homelessness and access to mental health services. This means not only investing in treatment but also implementing tailored programs that address the specific barriers to accessing care."
Source-Eurekalert
 MEDINDIA
MEDINDIA

 Email
Email