New study reveals subgroups of medulloblastoma - the most commonly occurring malignant brain tumor in children can be identified using imaging techniques, allowing early intervention.
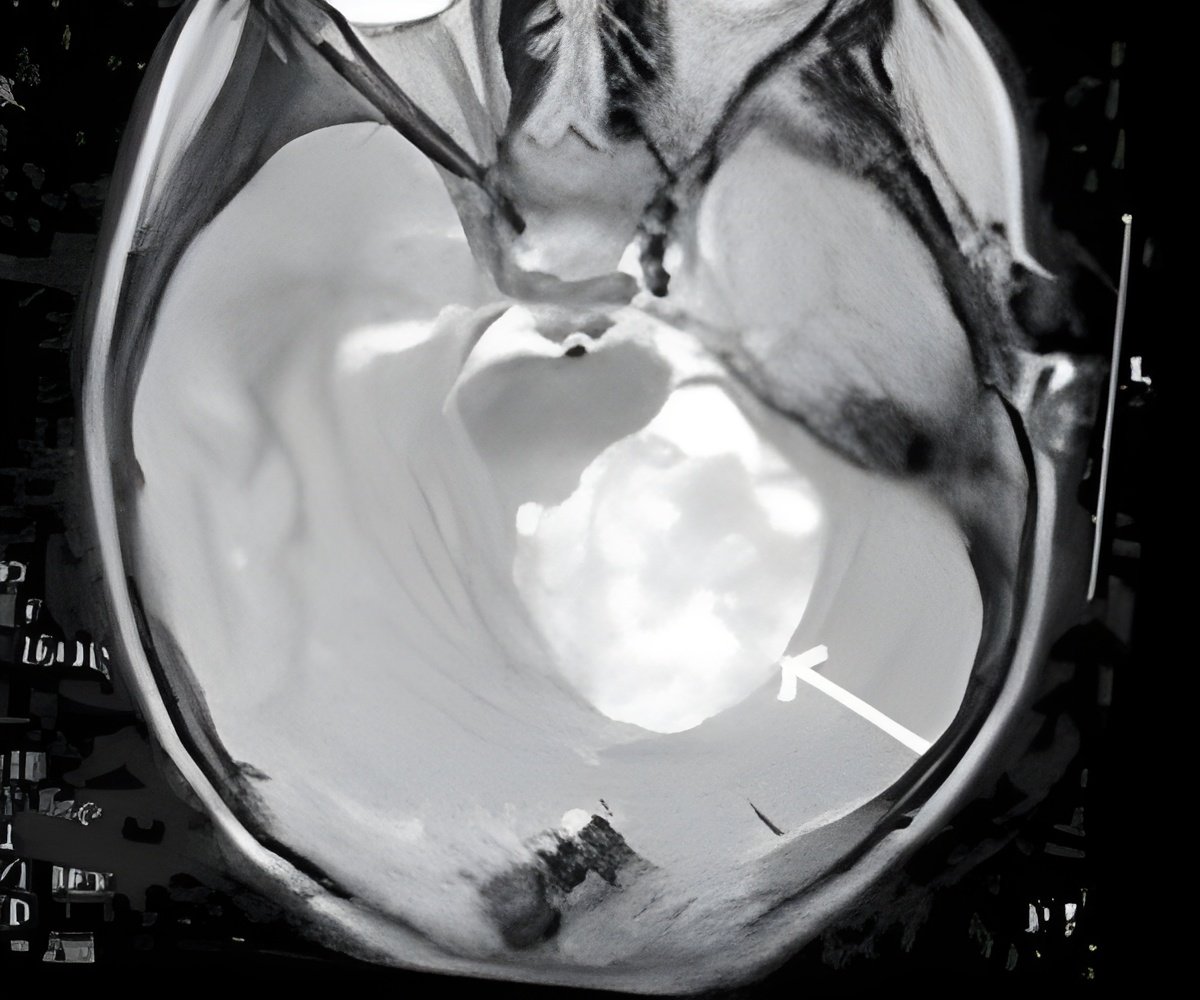
Treatment for medulloblastoma includes surgery, chemotherapy and radiation, with 5-year survival rates ranging from 30 to 90 percent depending upon risk profile. A recent discovery identified four subtypes of medulloblastoma (SHH, WNT, Group 3 and Group 4) with level of risk and clinical outcomes for each subtype varying significantly. Currently, classification requires surgical removal of the tumor followed by laboratory analysis of the tumor tissue. Given the clinical importance of subgroup determinations, a fast, reliable and easily accessible method could have a significant effect on the outcomes of children with this disease.
"MR spectroscopy is widely available, noninvasive and provides information on cellular metabolism, which is different in healthy and diseased tissue," said Stefan Bluml, PhD, investigator at The Saban Research Institute of CHLA and first author of the study. Bluml is also an associate professor of Research, Radiology and Biomedical Engineering at the Viterbi School of Engineering at USC.
Using frozen tumor tissue from 30 patients diagnosed with medulloblastoma, investigators performed subgroup analysis using standard techniques. These patients also had MRS performed at the time of diagnosis. With a screening panel composed of five metabolites, investigators found that the spectra for subgroups revealed distinct metabolic features, allowing them to differentiate subgroups SHH, WNT from Groups 3 and 4.
Clinical trials are being developed to incorporate molecular subgroups into risk and treatment stratifications. The ease of obtaining MRS at the time of diagnosis should allow its incorporation into future clinical trials aimed at validating this technique to improve diagnostic classification and, ultimately, improve outcomes in children with medulloblastoma.
Source-Eurekalert
 MEDINDIA
MEDINDIA



 Email
Email