Manipulating the renin angiotensin system that both prevents and reverses some characteristics of diabetic retinopathy was seen in mice model.

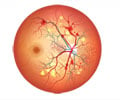
‘Diabetic retinopathy results from pathologic changes to small blood vessels in the retina. Common features are inflammation, leukostasis, and microangiopathy (a condition in which the capillary walls become so thick and weak that they bleed, leak protein, and slow the flow of blood).’





"We are not aware of another study that has demonstrated a therapy capable of reversing this form of retinal pathology, particularly in the presence of persistent untreated hyperglycemia," commented lead investigator Maria B. Grant, MD, of the Eugene and Marilyn Glick Eye Institute of Indiana University, Indianapolis, IN. "This research is based on the hypothesis that an imbalance between two axes of the RAS is a key initial event that leads to development of diabetic microvascular complications," explained Dr. Grant. The two axes consist of the classic and vasoprotective RAS.
The proinflammatory, vasoconstrictive classical RAS component is normally kept in check by a vasoprotective axis that is both anti-inflammatory and vasodilatory. Angiotensin converting enzyme-2 (ACE-2) is the primary enzyme of the vasoprotective component.
Administration of AAV-ACE--the therapeutic agent under evaluation--directly into the vitreous cavity of the eye using an adeno-associated virus vector, increases ACE-2 expression.
Investigators used mice, some of which were injected with streptozotocin (STZ) to induce diabetes. The protective effects of AAV-ACE2 were examined by performing two sets of experiments. In one cohort, AAV-ACE2 was administered two weeks prior to STZ injection. In a second cohort, to evaluate whether the enhanced expression of ACE2 could reverse diabetic retinopathy, AAV-ACE2 was administered six months after STZ, when diabetes and retinopathy were already established.
Advertisement
In addition, using a histological endpoint of retinal vascular degeneration, called acellular capillaries, the group determined that the AAV-ACE2 injection could reverse the diabetes-induced pathology. "These findings are very exciting because it is traditionally believed that this endpoint of vascular degeneration, acellular capillaries, represents an irreversible lesion," emphasized Dr. Grant.
Advertisement
Source-Eurekalert