Clinicians have developed new guidelines for the diagnosis and treatment of blood clotting disorders.

The new guidelines, which will become the global standard of care for the diagnosis of DVT, are published in the February issue of Chest, the journal of the American College of Chest Physicians.
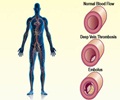
Deep venous thrombosis or DVT mainly affects the large veins in the lower leg and thigh. The clot can block blood flow and cause swelling and pain. When a clot breaks off and moves through the bloodstream, this is called an embolism. An embolism can get stuck in the brain, lungs, heart, or other area, leading to severe damage.
Rapid treatment for DVT is crucial to prevent potentially fatal complications. But the symptoms are often mistaken for a sprain or tendon injury, says Dr. Stevens.
"Thrombosis, particularly DVT, is the third most common cardiovascular disease in the United States, behind only heart attack and stroke," he says. "Prompt treatment is very important to prevent the clot from leaving the leg and traveling to the lungs, heart or brain. Physicians need good information on the best way to diagnose a DVT."
Because of research performed by Dr. Stevens and the team of thrombosis researchers at Intermountain Medical Center, Dr. Stevens was chosen to help draft a new chapter for the ninth edition of the guidelines. Previous editions have not included a chapter on diagnosing DVT.
Dr. Stevens says the new chapter provides a road map for the best-proven and most cost-effective ways to diagnose DVT.
Physicians from around the globe — everyone from primary care doctors to cardiologists, pulmonologists, orthopedic surgeons, and neurologists — will learn from the new guidelines at conferences, seminars, and journals in the coming months.
Dr. Stevens was joined in writing the chapter on DVT diagnosis by 11 other experts from hospitals and universities in Canada, England, Boston, and Buffalo, N.Y. Other chapters of the guidelines, written by different panels, examine the best treatment options for DVT and other blood-clotting disorders.
Source-Eurekalert
 MEDINDIA
MEDINDIA
 Email
Email








