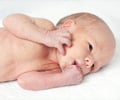
Only half (52%) of women who are eligible to receive a simple, effective, low-cost treatment to prevent death and disability in their newborn babies are getting it, finds a major international study of more than 303 000 births in 29 low-income and middle-income countries.
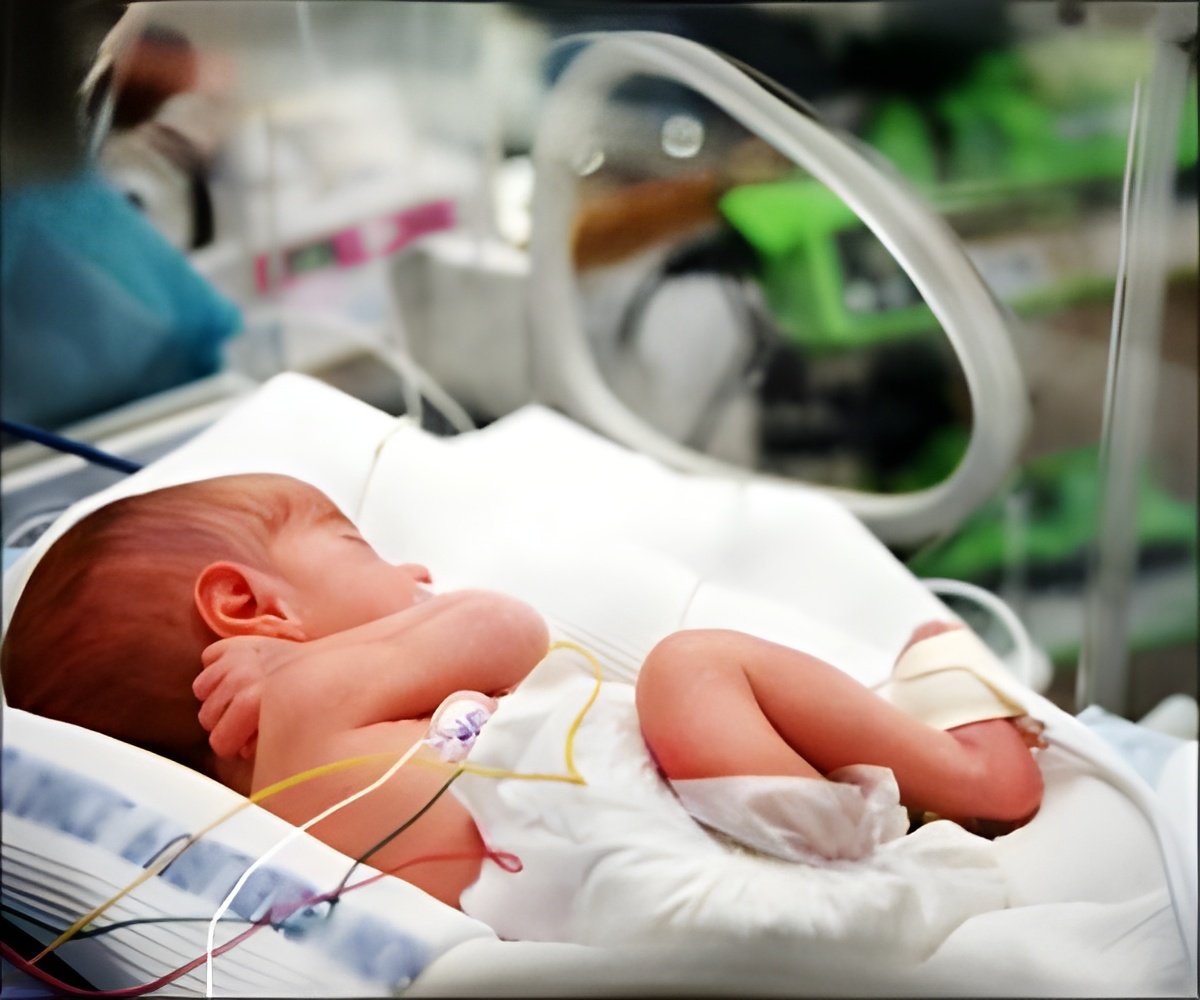
Use of antenatal corticosteroids was highly variable ranging from 16% of eligible women in Afghanistan, the Democratic Republic of Congo, Nepal, and Niger which have particularly high rates of neonatal deaths, to 91% in Jordan and 88% in the Occupied Palestinian territory. For more detailed findings by country see table 2 page 4.
An estimated 15 million babies (more than one in 10) are born prematurely every year. Around 1 million children die each year due to complications of preterm birth. Many survivors face a lifetime of disability, including learning disabilities and visual and hearing problems.
"Giving antenatal corticosteroids to women at risk of preterm birth is one of the most effective treatments for reducing newborn death and illness. More than three-quarters of premature babies could be saved with cost-effective interventions such as antenatal corticosteroids. This is particularly important in Africa and Asia where more than 60% of preterm deliveries occur and where resources are scarce and it is difficult to provide expensive neonatal care", said study leader Dr Joshua Vogel from the Department of Reproductive Health and Research at WHO in Geneva.
Using data from the WHO Multicountry Survey on Maternal and Newborn Health (WHOMCS), the researchers looked at patterns of antenatal corticosteroid use in preterm births and tocolytic drugs (to delay delivery) in spontaneous preterm births among 303 842 births that took place in 359 hospitals in 29 countries.
The analysis showed that a substantial proportion of antenatal corticosteroid use occurred in women who delivered at gestational ages at which benefit is controversial (19% at 22 weeks, and 24% at 34 weeks). Of women most likely to benefit (who gave birth between 26 and 34 weeks gestation), only half (52%) received them.
Dr Vogel explained, "Ideally, women in preterm labour between 26 and 34 weeks' gestation should receive antenatal corticosteroids, yet only 52% of eligible women received them. For women in spontaneous preterm labour, using tocolytic drugs can delay delivery and allow more time for antenatal corticosteroids to work, but only 18% of eligible women received both treatments and 42% received neither."*
Writing in a linked Comment, Stuart Dalziel, Caroline Crowther, and Jane Harding from The University of Auckland in New Zealand say, "Antenatal corticosteroids are not the panacea for preterm mortality in low-income and middle-income countries. Rather, the drugs should be included in a set of simple efficacious measures—family planning, access to antenatal care, antibiotic drugs for premature rupture of membranes, immediate and simple care for all babies, effective neonatal resuscitation, and kangaroo mother care…Future research should not focus on efficacy but on strategies to reduce barriers for appropriate use of antenatal corticosteroids. The WHOMCS approach would allow monitoring of progress. Let us not wait another 40 years to translate evidence into global practice."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email