Increase in vitamin D concentrations amid hospital patients has the potential to greatly reduce the risk of hospital-acquired infections points out a new study.

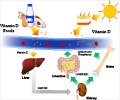
Patients are often vitamin D deficient since many diseases such as cancer, cardiovascular disease, and respiratory infections are linked to low vitamin D concentrations.
Pneumonia is the most likely HAI, followed by bacteremias, urinary tract infections, surgical site infections, sepsis, and others.
Vitamin D plays an important antimicrobial role. Among the antimicrobial actions are reducing local and systemic inflammatory responses as a result of modulating cytokine responses and reducing Toll-like receptor activation and stimulating the expression of potent antimicrobial peptides, such as cathelicidin and beta-defensin 2.
Cathelicidins are a family of peptides thought to provide an innate defensive barrier against a variety of potential microbial pathogens, such as gram-positive and gram-negative bacteria, fungi, and mycobacteria, at multiple entry sites, including skin and mucosal linings of the respiratory and gastrointestinal systems, as well as some viruses.
One of the advantages of vitamin D in combating HAIs is that it strengthens the innate immune response, thus overcoming the antibiotic resistance of many bacteria encountered in hospitals.
Advertisement
The study appeared recently in Dermato-Endocrinology, a peer-reviewed open-access journal published by Landis Bioscience in Austin, TX.
Advertisement