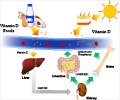
Prevention of vitamin D deficiency in children can potentially prevent chronic disease like cancer, heart disease, diabetes, and multiple sclerosis in adulthood.

In the UK, there has been an evidence of a resurgence of vitamin D deficiency in children. The National Diet and Nutrition Survey (NDNS) for young people (4–18 years old) in Great Britain reports that approximately 8 percent of children have less than 25 nmol/L of 25-hydroxy Vitamin D (25[OH]D) levels (or the storage form of vitamin D) and are thus considered vitamin D deficient. They also report that this deficiency is evident in most population age groups including older children and young adults.
Deficiency of vitamin D is seen to occur either due to dietary factors or non-dietary factors.
Dietary factors:
· Low intake of vitamin D rich food
· Insufficient vitamin D supplementation
· Genetic factors
· Skin pigmentation
· Age
· Ethnicity
· Sunshine exposure
· Body mass index
· Season
Vitamin D is mainly obtained from foods that are rich sources of this vitamin, for example, fatty fish such as salmon, tuna, and mackerel, fish liver oils, beef liver, cheese, and egg yolks. Other sources include dietary supplements, fortified foods such as infant foods, milk, or breakfast cereals and sunlight exposure.
The Recommended dietary allowance developed by the Food and Nutrition board for children, United States is as follows:
|
Age |
Vitamin D |
|
0–12 months* |
400 IU (10 mcg) |
|
1–13 years |
600 IU (15 mcg) |
|
14–18 years |
600 IU (15 mcg) |
The 2007 Scientific Advisory Committee on Nutrition report recommends that individuals at risk of inadequate sunshine exposure should receive supplementation of up to 10mcg/day. Additionally the UK government recommendations suggest regular, short periods of sunlight exposure without sunscreen during the summer months. They also highlight the risk of skin cancer and recommend the use of sunscreen (with a high UVB factor) for the majority of time spent outside.
In view of the paucity of data in the UK and indeed worldwide on the prevalence, predictors and associations of vitamin D insufficiency (VDI) astudy was conducted to evaluate the prevalence and predictors of vitamin D insufficiency VDI in children in Great Britain. A nationally representative cross-sectional study survey of children (1102) aged 4–18 years (999 white, 570 male) living in private households (January 1997–1998) was conducted. Information about dietary habits, physical activity, socio-demographics was taken and blood samples were collected.
The following variables, proposed as the possible predictors or causes for vitamin D deficiency amongst the children were studied.
· Age, gender and ethnicity
· Whether on income support
· Region residing
· Blood levels taken between December and May
· Amount spent per week in sports involving outdoor exercise or play
· Amount spent a day per week watching TV
· Vitamin D dietary intake and supplemental Vitamin D intake
· Body Mass Index (BMI [kg/m2])
For the purposes of this study, Vitamin D status was defined as insufficient when 25(OH) D levels were less than 50 nmol/L). Vitamin D levels were available for 1102 samples.
Following results were derived:
.35.1 percent of children aged between 4 to 18 years were vitamin D insufficient
·Plasma vitamin D levels decreased progressively with age in both sexes.
·There was no difference in the deficiency noted between girls and boys.
·There were marked seasonal differences found for vitamin D levels in children.
·Children whose families were on income support had significantly lower vitamin D levels.
.Children who spent more time doing outdoor exercise (at least half an hour/day/week) and less time watching TV per day (less than 2.5 hours) had higher vitamin D levels.
·Vitamin D dietary intake had no influence on vitamin D status. However, children who were taking vitamin D supplements had higher overall vitamin D levels.
·Overweight and obese children had lower vitamin D levels.
The results from this study confirm the high prevalence of VDI amongst UK children. The findings also clearly show that in children, there is no significant gender difference, but there is an increasing risk of VDI in older age groups. The researchers state that older children probably are lesser exposed to sunlight due to fewer incentives and opportunities to play outdoors. Supplements may be beneficial for older children, especially during the winter months given the higher risk of VDI shown.
Additionally, children whose families were in receipt of income support had more than twice the odds of those not on income supports; hence potentially government initiatives to tackle social inequalities may have an impact on vitamin D status.
Marked seasonal differences found in the study also stress that preventative strategies may be more necessary during the winter and spring months when vitamin D levels are at their lowest.
Children, who exercised outdoors for less than half an hour/day/week, were overweight and watched more than 2.5 hours/day/week of TV were at a greater risk of being deficient. These are potentially modifiable risk factors and therefore need to be seriously taken care of by the parents.
The study implies that initiatives to increase safe sunlight exposure by increasing opportunities and encouraging more outdoor activities, particularly in the summer months, may have an impact on vitamin D status. This also suggests that guidelines encouraging safe sunlight exposure and how this message is portrayed may need to be revised. It is interesting that dietary intake was not associated with vitamin D status, and therefore the study states the efforts in this area, would not be as effective as other suggested methods.
Prevention of vitamin D insufficiency in childhood may potentially prevent longer term chronic disease with presentation in adulthood and this is an area, which is under research at present. Unfavorable cardio metabolic risk factors in adults, hyperglycemia and the metabolic syndrome, type-1 diabetes, multiple sclerosis, malignancy and schizophrenia have all been implicated as potential consequences of early vitamin D insufficiency.
Experts suggest the need for devising clearer guidelines for vitamin D deficiency prevention coupled with increased awareness (especially in older children and at risk groups). Altogether the research undertaken clearly gets the clinicians to understand the severity of the problem and further guide their clinical decisions in order to establish preventive strategies.
Vitamin D requirements for children: The Recent Indian Recommendation:
As the body largely depends on vitamin D synthesis by the skin on sun-exposure, its dietary requirement is usually very small in the Indian context. It is important to note that even in India, the young growing children and adults, particularly in the urban areas, are physically less active and are not being exposed outdoors. This has eventually reduced the chances of vitamin D formation. This problem is being increasingly felt as more and more studies are reporting reduced circulating levels of 25 HCC in children of school age and also in some adults.
The Expert group of Indian Council of Medical Research feels that increasing the RDI (recommended dietary intake) is not the solution. Rather, ensuring adequate exposure to sunlight is the way out. Outdoor physical activity is a way of achieving both adequate vitamin D status and controlling overweight and obesity in the population. However, under situations of minimal exposure to sunlight, a recommendation of a daily supplement of 400 IU (10 μg) is suggested.
Reference:
Prevalence and Predictors of Vitamin D Insufficiency in Children: A Great Britain Population Based Study; Michael Absoud et al; Plos One 2011.
Nutrient requirements and recommended dietary allowances for Indians A report of the expert group of the Indian council of medical research, 2009. National Institute of Nutrition. Indian Council of Medical Research, Hyderabad.
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email