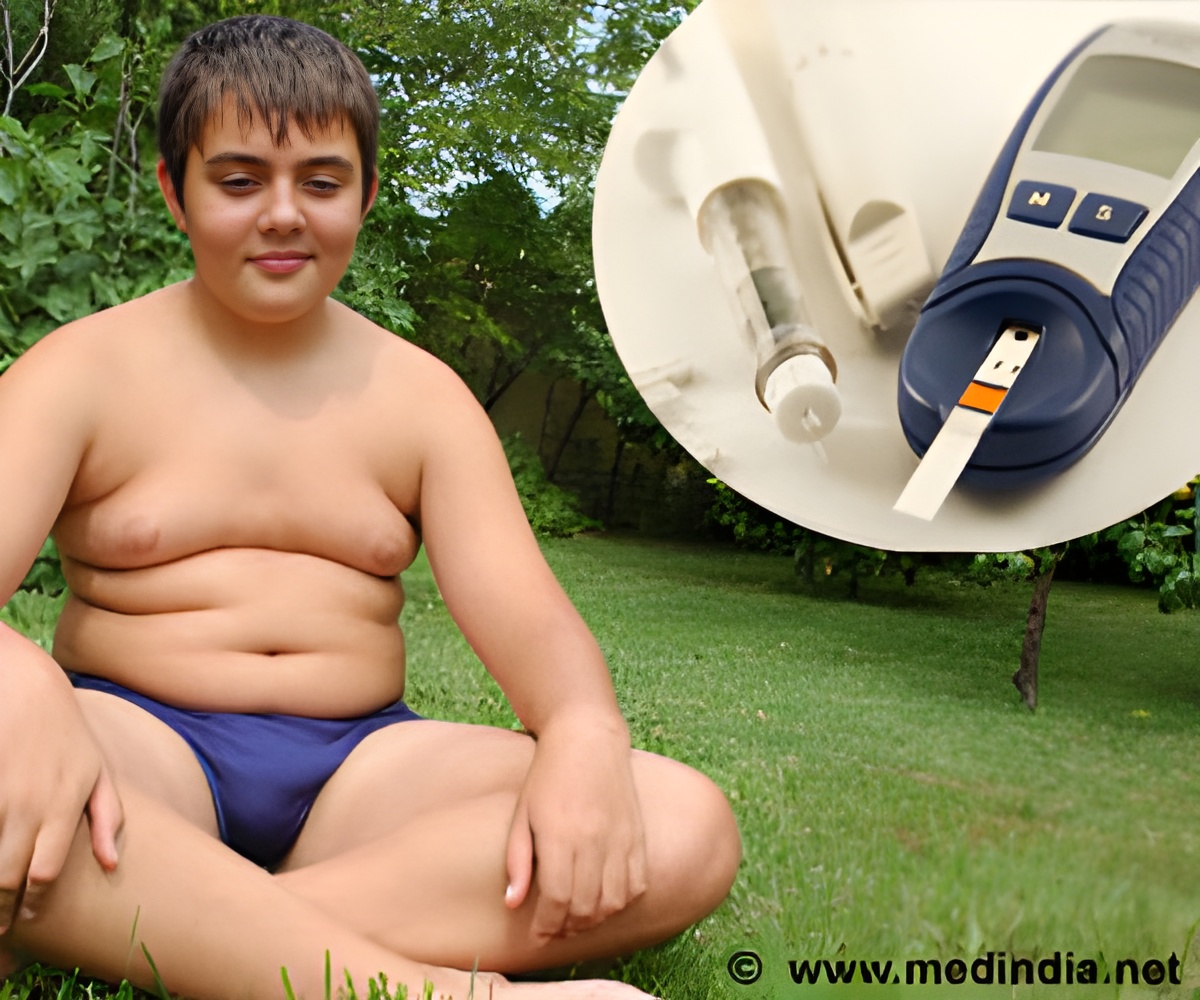
It is important to control blood glucose levels, too high sugar levels for longer period of time increases the risk of developing diabetes complications.
TOP INSIGHT
Sugar transport from the blood into the brain plays an important role. Among individuals with obesity and diabetes, blunted entry of glucose was found in the brain.
After fasting overnight, the study participants received intravenous infusions of glucose for two hours. During the infusions, the researchers used a brain scanning technique -- magnetic resonance spectroscopy -- to measure levels of glucose in the brain.
While blood glucose levels among the participants were similar, the researchers detected significant differences in brain glucose. Among the obese and diabetic participants, "we found decreased or blunted entry of glucose into the brain," said first author and assistant professor of medicine Janice Hwang, M.D.
That blunting could be one mechanism that undermines the ability of the brain to sense glucose, she noted.
The researchers also rated participants’ hunger, satisfaction, and fullness before and after the infusions. "The lean people who had more glucose entry into the brain also felt more full, even though they hadn’t eaten overnight," she said.
The study points to the importance of sugar transport from the blood into the brain as both a target for further research and possible pharmacological intervention in people with obesity and type 2 diabetes, the researchers noted.
 MEDINDIA
MEDINDIA


 Email
Email










