Vitamin D related genetic variants may increase the risk of liver damage in children diagnosed with the non-alcoholic fatty liver disease. Genetic and nutritional factors may influence the progression and development of the disease.
TOP INSIGHT
Vitamin D related genetic variants may increase the risk of liver damage in children diagnosed with the non-alcoholic fatty liver disease.
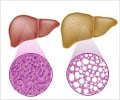
Non-alcoholic fatty liver disease is now the most common chronic liver disease in children. Both genetic and nutritional factors are thought to influence the progression and development of the disease. Previous studies have raised the question of whether improving vitamin D status through diet or supplements may benefit patients.
Study co-author Dr. Bernadette Moore, from the School of Food Science and Nutrition at the University of Leeds, said: "Despite the high prevalence of non-alcoholic fatty liver disease, thus far lifestyle change is the only proven effective treatment for those diagnosed. However, the lack of understanding regarding the disease's molecular pathogenesis makes it very difficult to identify patients who are most likely to suffer disease progression and therefore to benefit from intervention.
"Our research hopes to add to the growing body of work that would make it easier to identify those at risk of progression, allowing for more targeted individualized therapy."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email