Hyperglycemia in diabetes patients is also linked to the adverse impact on lung physiology, and a possible increase in the risk of COPD, stated new study.
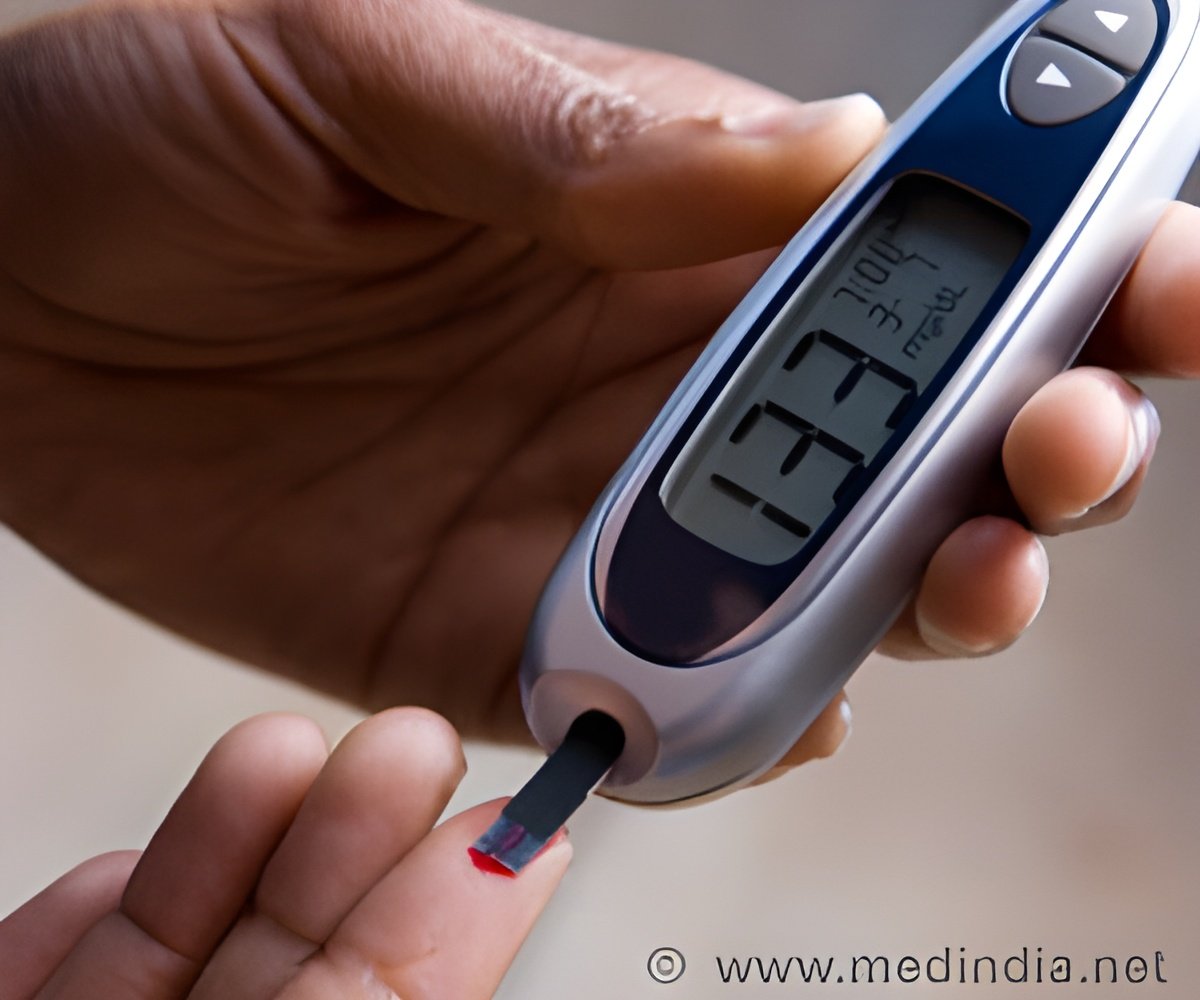
‘Hyperglycemia in diabetes patients is also linked to the adverse impact on lung physiology, and a possible increase in the risk of COPD.’





According to the review, the estimated global prevalence of COPD in 2010 is 11.7% corresponding to 384 million affected cases and is projected to be the third leading cause of death globally by 2030. Type 2 diabetes (T2 DM) is a metabolic disease associated with hyperglycemia, insulin resistance, and relative insulin deficiency. The global prevalence of T2 DM has increased dramatically in the last two decades, with an estimated 382 million people diagnosed in 2013 and the incidence is rapidly growing. It is projected to affect 592 million people by 2035. COPD is increasingly being recognized as a systemic inflammatory condition affecting more than just the lung. Comorbid chronic health conditions associated with COPD have poorer outcomes and require complex personalized therapeutic intervention approach.
COPD is being increasingly recognized as a risk factor for the development of T2 DM through different mechanisms including systemic inflammation, obesity, hypoxia and use of corticosteroids.
T2 DM and COPD are both expected to be among the top ten leading causes of mortality and burden of disease worldwide by 2030. There are limited clinical studies addressing the management of patients who have T2 DM and COPD.
Presently, management options are geared towards symptomatic management but do not address the underlying cause of these diseases. It would be ideal to target treatments to address the underlying systemic inflammation, but no such therapeutic agents are available yet. The standard of care respiratory management with timely treatment of COPD exacerbations, flu vaccination, antibiotic use can result in the reduction of oxidative stress and systemic inflammation, which will, in turn, will reduce insulin resistance and optimize glucose control in T2 DM patients.
Advertisement
Given the overwhelming evidence of the association between the COPD and T2 DM, their intertwined pathologies and the impact on the prognosis, it is important for the endocrinologist to measure lung function in T2 DM patients and for pulmonologists to screen for T2 DM in COPD patients. The team of researchers believes that this collaborative partnership is crucial for improving the outcomes in patients. The team also agrees additional research is required to improve our knowledge about the relationship between COPD and T2 DM, to help with providing better care with these two common disorders.
Advertisement