The researchers evaluated more than 77 million hospital admissions during 2005-2006, 271,983 of which were associated with dysphagia, as indicated by the National Hospital Discharge Survey (NHDS). The median number of days in the hospital for patients with dysphagia was 4.04, compared to 2.40 days for patients without dysphagia. Mortality increased significantly in patients with dysphagia and disk disorders or heart disease, and those undergoing rehabilitation had a greater than 13-fold increased risk of mortality. Patients ages 75 and older were twice as likely to have dysphagia.
"Our study shows that dysphagia has a significant impact on length of stay and prognostic indicators," said Kenneth W. Altman, MD, PhD, Associate Professor of Otolaryngology, lead author on the study. "Early identification of dysphagia and therapeutic intervention are critical to preventing further complications in these patients and reducing length of stay. These data indicate the necessity for health care providers to prevent or diagnose this condition early to reduce complications."
The impact of dysphagia on hospital resources was also substantial. Patients with dysphagia are often at risk of aspirating, which often requires antibiotic use and intubation. The increased mortality risk associated with the condition also increases end-of-life costs. Using a measurement tool previously developed for community-acquired pneumonia, the researchers estimated the cost of dysphagia at nearly $550 million over the two year period.
"With our country moving into a value-based health care system, we will truly feel the impact of the costs associated with dysphagia," said Dr. Altman. "As such, it's important to develop strategies to prevent and treat this debilitating condition to reduce those costs."
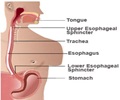
Dysphagia is present with a number of serious conditions, which may contribute to mortality risk. The most common conditions associated with dysphagia were stroke, aspiration pneumonia, urinary tract infection, esophageal disease, fluid or electrolyte disorder, and congestive heart failure. Patients with these conditions are especially susceptible to aspiration. The authors emphasize that dysphagia is severely underreported, due to minor cases not being documented, or clinicians seeing it as a side effect of another condition rather than a condition itself.
Advertisement
Advertisement