Research reveals that patients with rheumatoid arthritis may not need to halt use of their antirheumatic drugs prior to surgery due to fears of increased infection risk.
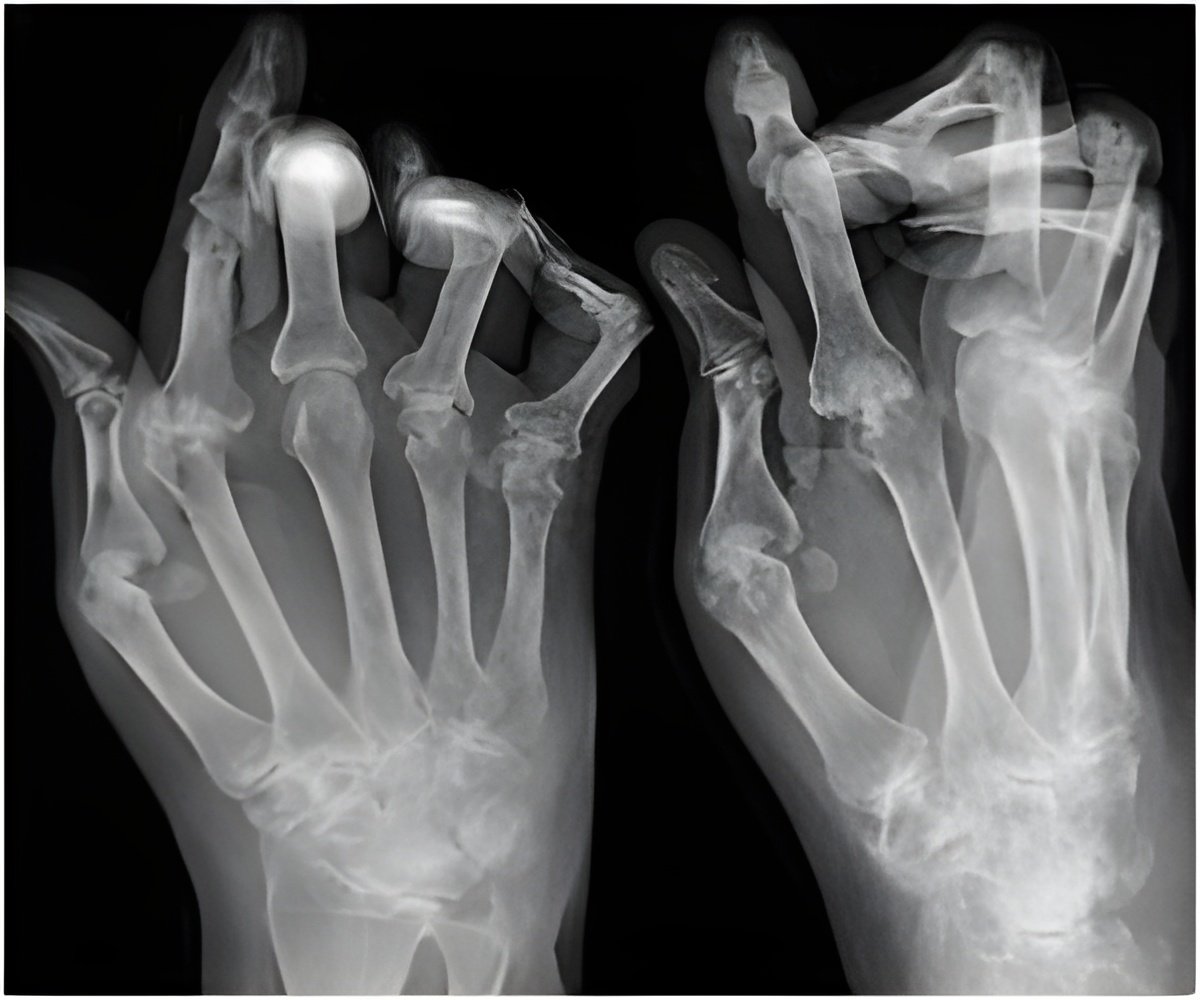
Researchers based at the Michael E. DeBakey Veterans Affairs Medical Center and the Baylor College of Medicine in Houston, Tex., gathered data on perioperative use of disease-modifying antirheumatic drugs, such as methotrexate, and the subsequent rate of postoperative infections from RA patients treated in the VA Medical Center over a 10-year period from 2000 to 2009. While there was little evidence to support temporary stopping of DMARDs or biologic agents in RA patients prior to surgery, the common reasoning had been that the drugs may increase patients' infection risk due to their suppression of the immune system to control inflammation in autoimmune diseases like RA.
The researchers' aim was to examine postoperative infection rates in a sample of RA patients in order to determine if use of the immunosuppressant drugs prior to surgery had any effect on their infection risks 30 days after their procedures, says Bernard Ng, MD; associate professor of medicine and chief of rheumatology; VA Puget Sound HCS; and an investigator in the study.
"Our ability to make evidence-based recommendations on whether immunosuppressive drugs for treatment of RA should be stopped before an elective surgery is limited based on current literature on this topic," explains Dr. Ng. "We often receive consults from our surgery colleagues for this issue, and apart from certain orthopedic surgeries and the use of methotrexate, we don't really have much to say when other surgeries and DMARDs are involved."
Using VA administrative patient databases, the researchers looked at 6,548 RA patients who had been using only one DMARD or biologic agent in the perioperative period. Those patients using multiple agents were excluded to simplify the results. The researchers then compared the rate of wound infections within 30 days of surgery for these patients with the amount of time prior to surgery that their medication had been stopped. Wound infections, according to the modified 1992 U.S. Centers for Disease Control and Prevention criteria for postoperative infection, were recorded and analyzed by themselves and together with other infections like pneumonia, urinary tract infections and sepsis. Other factors that might also affect infection rates, such as co-existing diseases, diabetes mellitus, smoking or chronic steroid use, were also factored in by the researchers.
Results showed that RA patients who did not stop their use of a DMARD or biologic agent prior to surgery did not have a significantly higher risk of postoperative infection compared to patients who did stop their drugs. Conversely, those patients who stopped using their DMARD or biologic agent after surgery did have an increased incidence of both postoperative wound infections and general infections. Drug treatments likely were halted because the patients developed postoperative infections, the study authors concluded.
Advertisement
Dr. Ng goes on to say, "This is a preliminary database study with several limitations. For example, the analyses done involved only single DMARD and biologic use, and the types of surgeries were not categorized. Further studies analyzing various combinations of DMARD and biologics, and specific types of surgeries will be useful in helping us develop deeper knowledge in this area."
Patients should talk to their rheumatologists to determine their best course of treatment.
Advertisement