Giving the Salk inactivated poliovirus vaccine to individuals who had already been given the Sabin live-attenuated oral poliovirus vaccine may improve their immunity.
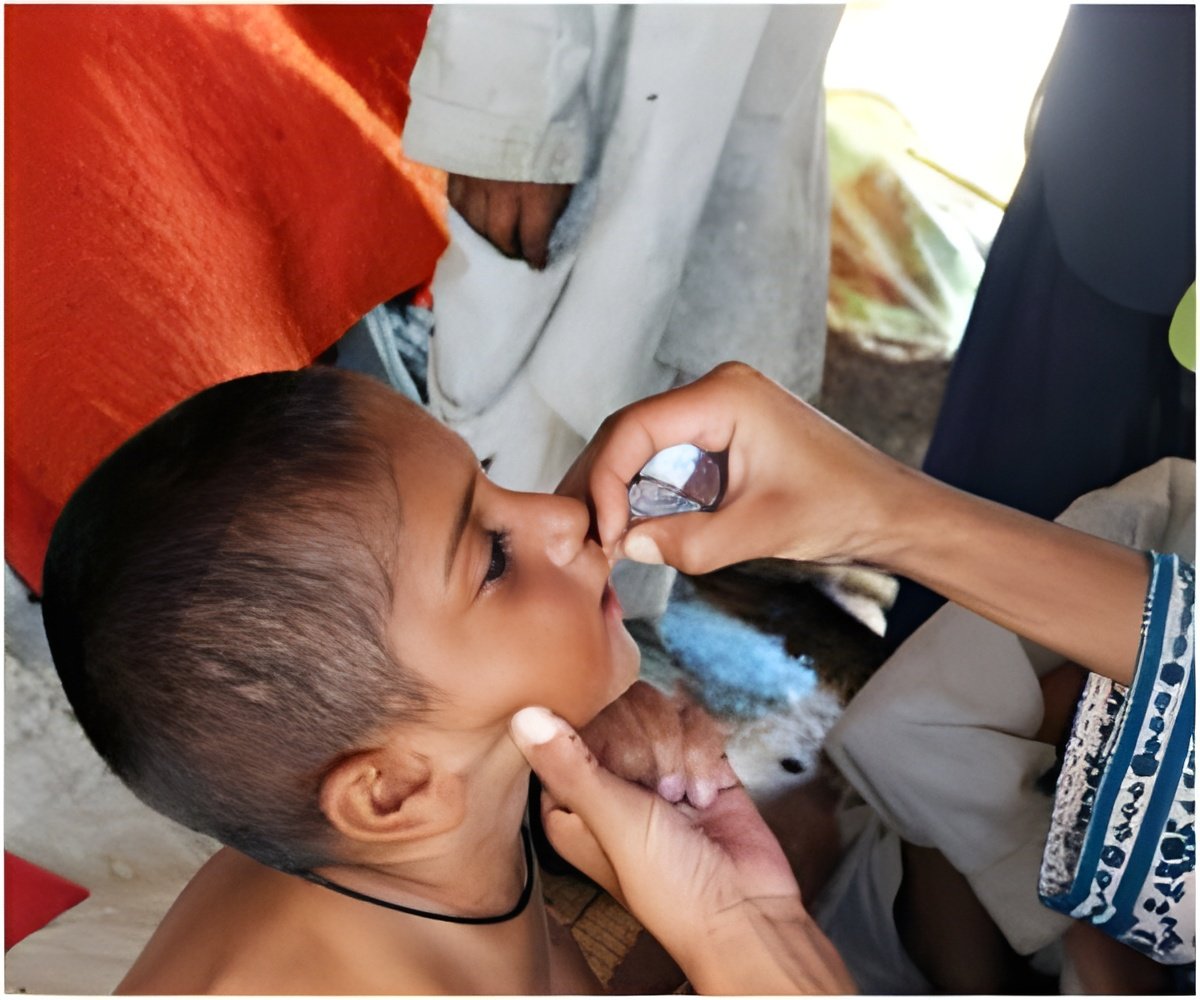
"This study revolutionized our understanding of IPV and how to use it in the global eradication effort to ensure children receive the best and quickest protection possible from this disease," said senior author Dr. Bruce Aylward, assistant director-general for Polio, Emergencies and Country Collaboration at the World Health Organization (WHO).
"IPV should be used to accelerate the eradication of the virus in populations that have limited access to vaccination," added Dr. Hamid Jafari, WHO's director for polio operations and research and the lead author of the report. "The study has also provided the evidence for use of IPV among travelers to limit further international spread of the virus."
Since the development of the polio vaccine in the 1950s, efforts to eradicate the poliovirus, which can cause life-long paralysis, relied mainly on OPV—the choice of the Global Polio Eradication Initiative—rather than IPV.
"This is because OPV has a superior ability to induce mucosal immunity, is easy to administer requiring no needles, and is substantially cheaper," said Caroline Ash, a senior editor at Science.
However, in parts of the globe where polio is proving difficult to eradicate, the choice between OPV and IPV continues to be widely debated by scientists. This is because mucosal immunity (the protection offered by the linings that separate the body's sterile interior from the outside world) diminishes rapidly after OPV treatment, meaning several doses of this vaccine are required. And providing multiple doses to eradicate wild poliovirus is challenging in remote areas or conflict zones like Afghanistan, Nigeria and Pakistan.
In hopes of one day withdrawing OPV from treatment regimens, Jafari, Aylward and colleagues tested whether use of both vaccines would improve mucosal immunity; although administering IPV after OPV is known to close certain immunity gaps, its effect on intestinal mucosal immunity is less well-characterized.
In children who were given IPV, viral shedding was reduced, meaning that these children were much less infectious to others—a key in halting the spread of the virus.
Dr. Jafari and colleagues also found that a single dose of IPV, which is administered by injection, induced intestinal mucosal immunity more effectively in children than an additional OPV dose.
The results of this study could help resolve the 50-year-old controversy, dating back to the time of Jonas Salk and Albert Sabin, over vaccine choice. "The answer is now very clear," explained Dr. Roland Sutter, WHO's coordinator for research and product development, polio operations and research. "Both vaccines complement one another and should be used to interrupt the final chains of transmission to attain a polio-free world in the most rapid and effective way possible."
"The global eradication effort is at a critical crossroad," continued Dr. Jafari. "Endemic polio is increasingly geographically restricted to populations in insecure and inaccessible areas. Yet the virus in these areas persists with incredible tenacity and threatens the increasingly vulnerable populations in polio-free countries with weak or conflict-affected health systems."
Source-Eurekalert
 MEDINDIA
MEDINDIA


 Email
Email