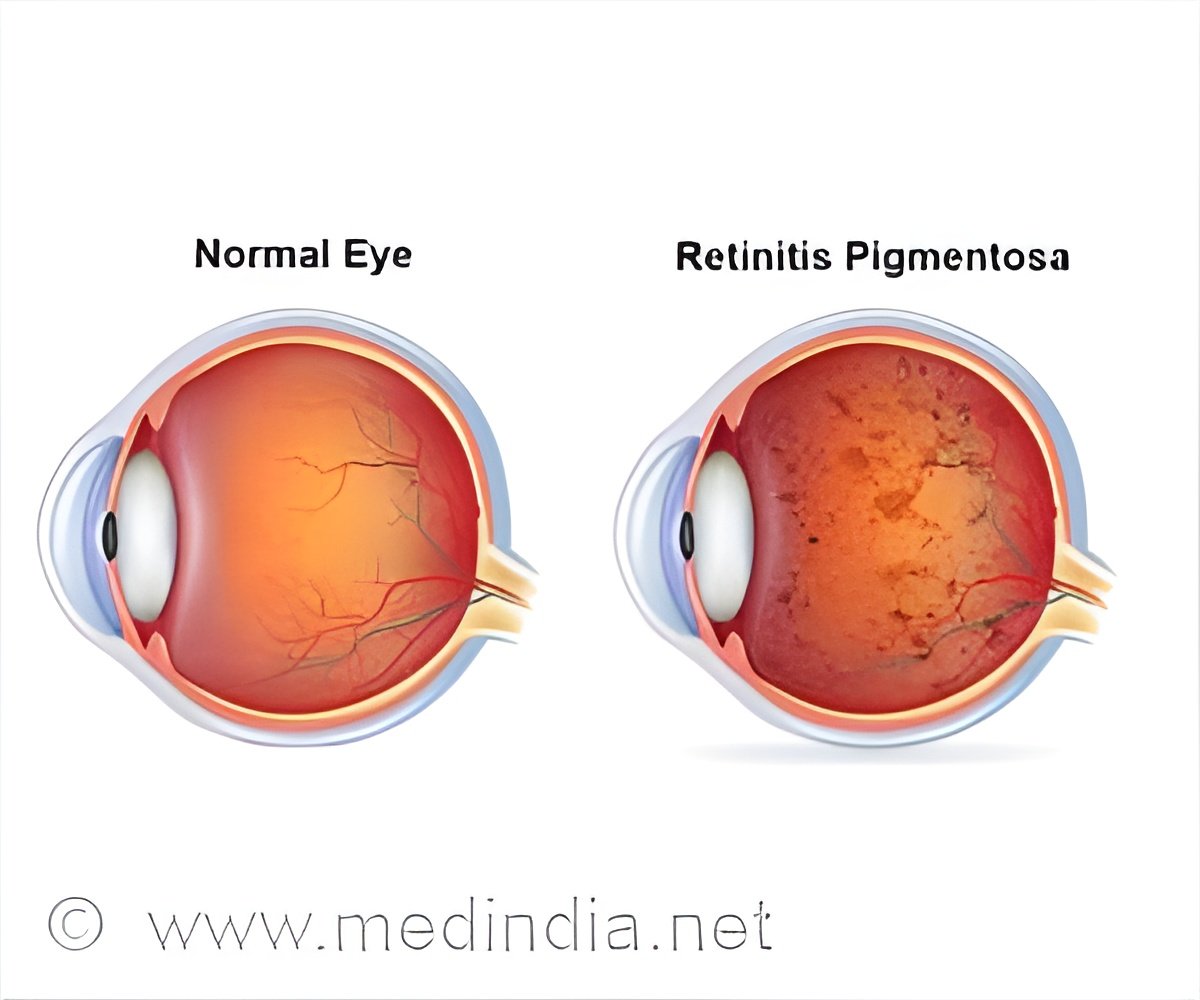
Complement system found to play a vital role to slow retinal degeneration in a mouse model of retinitis pigmentosa.
‘Complement activation is actually found to useful for clearing dead cells and maintaining a state of homeostasis or a physiological balance in the retina delaying the progression of degenerative eye disease.’
Read More..




Retinitis pigmentosa is an incurable and unpreventable blinding eye disease that affects 1 in 4,000 people. Read More..
"Much research is devoted to studying therapies that attempt to alter the immune system's role in inherited diseases such as retinitis pigmentosa because such treatments would have broad applicability, regardless of a patient's causative mutation," said the study's principal investigator Wai T Wong, M.D., Ph.D., chief the Neuron-Glia Interactions in Retinal Disease Section at NEI.
In previous studies, activation of the complement system, which mediates some aspects of inflammation, worsens damage in age-related macular degeneration (AMD), a leading cause of blindness in people age 65 years and older.
"The current study involving retinitis pigmentosa underscores the notion that the complement system may in fact exacerbate or curb retinal degeneration depending on the context. Appreciating this complexity is important for guiding the development of therapies that target the complement immune system to treat degenerative diseases of the retina," Dr. Wong said.
Sean Silverman, Ph.D., an NEI postdoctoral researcher in Dr. Wong's lab and the lead author on the study, and colleagues monitored the genetic expression of the complement system in a transgenic mouse model of retinitis pigmentosa. They found that upregulation of complement expression and activation coincided with the onset of photoreceptor degeneration. What's more, this upregulation occurs in the exact location of the degeneration.
Advertisement
Using the retinitis pigmentosa mouse model, the researchers examined the role of C3 and CR3, the central component of complement and its receptor, by comparing mice with genetically ablated C3 or CR3 to mice with normal expression. They found that the absence of C3 or CR3 made degeneration worse. Rod photoreceptors, the light-sensing cells that die off first in retinitis pigmentosa, were precipitously lost along with a surge in the expression of neurotoxic inflammatory cytokines.
Advertisement
" When placed alongside each other in a dish, microglia from C3- or CR3-ablated retinas turned out to be toxic to photoreceptors.
Taken together, the results show that in the context of retinitis pigmentosa, complement activation is actually helpful for clearing away dead cells and maintaining a state of homeostasis, a physiological balance, in the retina.
However, in the context of AMD, harmful effects observed from complement activation have spurred clinical trials testing complement inhibitors. "Our findings suggest that this approach may be appropriate for some disease scenarios, but may induce complex responses in other disease scenarios by inhibiting helpful and homeostatic functions of inflammation," Dr. Wong said.
Source-Eurekalert