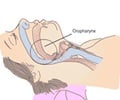
Obstructive sleep apnea is defined as a sleep disorder involving decrease in airflow in the presence of breathing effort. The treatment for OSA includes pharmacologic and non- pharmacologic modalities.

Individuals suffering from obstructive sleep apnea complain of daytime sleepiness, poor quality of life and cardiac, psychiatry and metabolic disorders.
The occurrence of OSA is 3 percent to 7 percent in males and about 2 percent to 5 percent in females. The morbidity percentage in obese individuals is 78.
The prevalence of OSA increases with advancing age and the primary risk factor is obesity.
The criterion of diagnosis for OSA is either an apnea-hypopnea index (AHI) of more than five events per hour along with excessive daytime sleepiness or an AHI greater than 15 events per hour irrespective of symptoms. Overnight polysomnography is needed to calculate the frequency of hypopneic and apneic events.
Peppard et al conducted a study to assess the relationship between hypertension and obstructive sleep apnea. They observed that OSA was a risk factor for hypertension and with continuous positive airway pressure (CPAP), high blood pressure can be treated.
It was also observed that OSA may lead to insulin resistance and diabetes.
The treatment for obstructive sleep apnea (OSA) includes pharmacologic and non- pharmacologic modalities. Continuous positive airway pressure (CPAP) is the most sought after treating option for OSA. It is effective in creating a pneumatic splint and maintaining patency of airway and thus eliminates apnea and hypopnea episodes.
Other therapies are oral appliances, drug therapy, weight loss and surgery. Reduction of risk factors, rectifying the underlying metabolic ailments, treating the repercussions and preventing the episodes of hypopnea and apnea constitute the goals of the treatment.
Tricyclic Antidepressants:
Antidepressants improve obstructive sleep apnea by ‘increasing rapid eye movement (REM) sleep latency while decreasing the overall amount of time spent in REM sleep’.
Smith and colleagues and Brownell et al have studied the effect of Protriptyline as a REM sleep suppressant. Smith et al revealed that there was a reduction in snoring and apnea-hypopnea index (AHI) and oxygen saturation and daytime somnolence improved significantly.
Serotonin Agents:
The muscle tone of the upper airway can be increased by selective serotonin reuptake inhibitors. Hanzel et al conducted a study that revealed reduction in apnea-hypopnea index (AHI) from 57 to 34 events per hour with both protriptyline and fluoxetine but no reduction was noticed in AHI during REM sleep.
‘Prasad et al combined fluoxetine with ondansetron, which yielded small reductions in AHI during non-REM and REM sleep after 28 days of treatment.’
Nicotine Products:
Nicotine products not only stimulate respiration but also increase the activity of the muscles responsible for dilating the upper airway. ‘Gothe et al reported that the use of nicotine gum (2 or 4 mg) at bedtime eliminated obstructive apneas in the first 2 hours of sleep.’
Methylxanthine Derivatives:
Methylxanthine such as oral theophylline and IV aminophylline work by inhibiting the adenosine receptors and stimulates the ventilator drive.
‘Mulloy and McNicholas evaluated oral theophylline for 4 weeks in 12 patients with OSA. They reported a small yet statistically significant decrease in AHI (from 49 to 40 episodes per hour) as did Hein et al in a similar study (from 9.2 to 6.7 episodes per hour).’
Inhaled Corticosteroids:
Allergic rhinitis is known to cause nasal obstruction and deteriorates obstructive sleep apnea. Inhaled nasal corticosteroids can improve the patency of airway.
‘Kiely et al investigated the use of intranasal fluticasone in 23 snorers with rhinitis for 4 weeks. Further evaluation of the subpopulation of 13 patients with AHI values above 10 episodes per hour resulted in an observed drop in AHI from 30.3 to 23.3 with the use of inhaled nasal fluticasone.’
Leukotriene Antagonists:
The use of oral leukotriene antagonists such as intranasal budesonide and oral montelukast has been successful in treating sleep-disordered breathing in children.
‘Goldbart et al studied daily montelukast therapy (4 or 5 mg) in 24 children with OSA for 16 weeks. They reported a significant reduction in respiratory disturbance index (RDI) and adenoid size.’
Nasal Decongestants:
The nasal decongestants act on the arterioles of the mucosa of nose and result in vasoconstriction by stimulating alpha-adrenergic receptors.
‘Braver and Block evaluated the use of oxymetazoline in 20 OSA patients, but found it to have no benefit when used as monotherapy.’
Thyroid Replacement:
It is seen that patients with hypothyroidism often suffer from obstructive sleep apnea. This could be either due to reduction in ventilator drive or weight gain.
Thyroid replacement therapy may improve the situation however the evidences are quite conflicting.
Hormone Replacement:
Menopause or cessation of menstruation is regarded as a risk factor for sleep-disordered breathing and snoring. The effects of medroxyprogesterone, estrogen and combination therapy with progesterone and estrogen on obstructive sleep apnea are also beneficial in hypercapnia-associated disorders.
Wake-Promoting Agents:
Stimulant medications such as armodafinil and modafinil have been clinically investigated as adjunctive therapy for obstructive sleep apnea. The adverse effects are dizziness, nausea, headache and insomnia.
Miscellaneous Agents:
Sleep apnea can be treated by additional therapies such as agents for acromegaly, testosterone, antihypertensives, glutamate antagonists, physostigmine, acetazolamide, opiate antagonists, tumor necrosis factor (TNF)-alpha agonists, and carbon dioxide inhalation.
Except for physostigmine, TNF-alpha antagonists, carbon dioxide inhalation and agents for acromegaly other miscellaneous agents have not been proved to be effective in lowering OSA symptoms.
‘A pilot study of TNF-alpha agonists did demonstrate reduced AHI and reduced sleepiness, but further studies would be required to establish their benefit in OSA.’
Agents like mirtazapine and donepezil are also beneficial in treating obstructive sleep apnea. Donepezil is a reversible inhibitor of acetylcholinesterase enzyme, and is known to improve saturation of oxygen in Alzheimer’s patients.
‘A one-month, double-blind, placebo-controlled study of donepezil in OSA patients found an improvement in AHI, oxygen saturation, and REM sleep. The study failed to find improvement in sleep efficiency or EPSS.’
With increasing doses of mirtazapine, significant decrease in collapse of upper-airway has been noticed. However the associated side effects are sedation and weight gain.
Hazardous Medications:
Obstructive sleep apnea can be worsened by CNS depressants such as barbiturates, older sleep agents, benzodiazepines, opiates and alcohol. These agents can adversely affect the ventilation control during sleep and make the upper airway easily collapsible.
Other harmful drugs such as sildenafil, an erectile dysfunction medication and propranolol, a beta-blocker should also be avoided in OSA.
It is finally concluded that clinical trials have failed to reveal noteworthy benefit in pharmacologic treatment of OSA. Continuous positive airway pressure (CPAP) still remains a better choice in comparison to drug therapy.
The researchers said that further pharmacologic therapies should be formulated for treating daytime sleepiness and fatigue related to obstructive sleep apnea.
Another important point is the treatment of metabolic disorders and obesity for controlling patients with OSA.
Reference:
Pharmacotherapy Options in the Treatment of Obstructive Sleep Apnea; Kimberly Tackett et al; US Pharm. 2012;37(7):23-26.
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email