American Cancer Society updated the cervical cancer screening guidelines. The new guidelines are simple, and they reflect the developments in cervical cancer prevention.
Highlights:
- Cervical cancer screening is recommended from the age of 25 to 65 years
- American Cancer Society recommends Human Papillomavirus (HPV) test or cotesting every 5 years
- Also, recommends cytology testing every 3 years, if HPV testing is unavailable
- Cervical cancer screening can be stopped at the age of 65 if adequate cumulative negative tests are obtained within the past 10 years
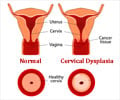
Cervical cancer is a type of cancer that forms in the cells of the cervix. The most common types are squamous cell type (70%) and adenocarcinoma type (25%).
TOP INSIGHT
American Cancer Society updated cervical cancer screening guidelines. The new guidelines recommend less and more simplified screening procedures. The recommendations reflect on the growth of cervical cancer prevention.
Read More..
Cervical Cancer and Human Papillomavirus (HPV)
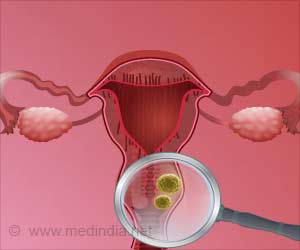
Cervical cancer is caused by an infectious virus called human papillomavirus (HPV).
HPV is classified as high-risk and low-risk types based on their risk of causing cervical cancer:
- High-risk HPV – HPV 16, 18, 31, 33, 34, 35, 39, 45, 51, 52, 56, 58, 59, 66, 68, 70
- Low-risk HPV – HPV 6, 11, 42, 43, 44
What are the Updated Cervical Screening Guidelines?
The preferred method of testing is the primary human papillomavirus (HPV) testing every 5 years. Primary HPV testing is HPV testing without Pap Test.
HPV testing is generally considered more accurate compared to the Pap test. If only cytology testing is used, testing every 3 years is acceptable.
A negative HPV test is often associated with a very low cervical cancer risk.
Individuals older than 65 years with no history of CIN2+ within the past 25 years with adequate negative prior screening within 10 years, can stop cervical cancer screening with any modality.
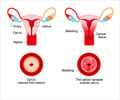
CIN2+ is cervical intraepithelial neoplasia (CIN). It is a premalignant lesion and exists in three stages – CIN1, CIN2, and CIN3. CIN2 and CIN3 are collectively known as CIN2+. If the precancers are left untreated, they can progress to cervical cancer.
Adequate negative prior screening is 2 consecutive negative tests of either primary HPV or cotests and 3 consecutive negative cytology tests within the past 10 years.
If sufficient data is not met, individuals above the age of 65 should continue screening for cervical cancer until criteria are met.
Why is Cervical Cancer Screening Age Moved from 21 to 25 years?
The HPV vaccine is available for the past 15 years. Since then, the use of HPV vaccination has increased, and a drop in precancerous cervical changes was observed.
There are also potential harms associated with the treatment of precancerous cells, including preterm birth between 20-24 years. Screening has not shown to lower the rate of cancer in this age group. Thus, ACS changed the recommended screening age from 21 to 25 years.
Starting screening at the age of 25 can prevent 13% more cervical cancers and 7% more cervical cancer deaths compared to starting at 21 years old, according to Dr. Saslow. “Our model showed we could do that with a 9% increase in follow-up procedures, but with 45% fewer tests required overall.”
In summary, the updated cervical cancer screening guidelines from the American Cancer Society recommend clear and simple screening procedures.
Source-Medindia
 MEDINDIA
MEDINDIA



 Email
Email