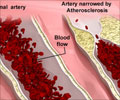
Stem cells could be used for creating transplant arteries very soon. These transplants will replace damaged or diseased arteries and help save the lives of patients suffering from cardiovascular diseases.
- Stem cells will soon be capable of creating transplant arteries
- These transplants will be able to replace arteries that are damaged or diseased
- This could help save the lives of many patients suffering from cardiovascular diseases
The study, published in Stem Cell Reports, found a way to grow smooth muscle cells from pluripotent stem cells that is superior to conventional methods. The study has also identified a potential new drug that can significantly reduce the risk of complications arising during cardiac bypass surgery.
The study was led by Dr. James Thomson, PhD, who is Director of the Regenerative Medicine Laboratory at the Morgridge Institute for Research, Madison, Wisconsin, USA. The lead author of the study was Jue Zhang, who is an Associate Scientist at the Morgridge Institute for Research.
“We decided to focus on blood vessels because cardiovascular disease is a major cause of death worldwide,” Thomson says. “In the U.S. for example, heart disease and stroke are the No. 1 and No. 3 killers, respectively. And this work also has implications beyond making vessels for transplantation; it’s sort of a stepping stone to more advanced tissue engineering.”
TOP INSIGHT
Stem cells could soon be used to create transplant arteries that would replace damaged or diseased arteries and help save the lives of cardiovascular disease patients.
Read More..
How Were the Arteries Created in the Lab?
Two essential cell types are required for the production of arteries in the lab. These are endothelial cells and smooth muscle cells. The Morgridge researchers in 2017 reported the production and characterization of endothelial cells. The present study focuses on smooth muscle cells.In this regard, Zhang indicated that the growth factors that are conventionally used for producing smooth muscle cells from stem cells also produce intimal hyperplasia – a condition in which a part of the arterial wall becomes thickened due to multiplication and migration of smooth muscle cells, resulting in narrowing of the artery.
It should be noted that intimal hyperplasia is the most common cause of rejection of bypass grafts. Therefore, the researchers were, naturally, looking for a method that would reduce the chances of intimal hyperplasia; as otherwise, it would be very difficult to construct an artery in the lab.
What is the Importance of RepSox?
RepSox is a small molecule identified by the researchers using high throughput screening (HTS), which has the potential for producing cells that are capable of contraction. RepSox was identified by screening 4,804 small molecules. In contrast to currently available growth factors, RepSox is capable of inhibiting intimal hyperplasia and is much more stable than the former and is also more cost-effective to produce.RepSox is not only effective for differentiating smooth muscle cells, but also an ideal drug candidate for inhibiting intimal hyperplasia that can cause serious complications following bypass surgery. Moreover, since RepSox is cell-type specific, it acts on smooth muscle cells without affecting the neighboring endothelial cells.
Therefore, the stem cell-based HTS technique can be considered as a novel strategy for the identification of potential new drug molecules that prevent narrowing of the arteries.
“Even after you have bypass surgery, you can have some problems with your artery, like restenosis (narrowing arteries) due to intimal hyperplasia,” Zhang says. “Currently there are only two FDA-approved drugs on the market [to address these problems], and they’re not cell-type specific, meaning they have side-effects. We found that RepSox inhibits intimal hyperplasia and has fewer side-effects.”
Concluding Remarks
The study findings have brought the scientists one step closer to their goal of developing improved treatments for cardiovascular diseases. However, despite this huge progress, there is still another challenge, concerning cell maturity.“Basically this cell type is better than previous efforts, but it’s still not mature yet,” Zhang says. “We need to induce these cells to become more mature, to be more similar to our native artery, to make it more functional.”
Reference:
- Stem Cell Scientists Clear Another Hurdle in Creating Transplant Arteries - (https://morgridge.org/story/stem-cell-scientists-clear-another-hurdle-in-creating-transplant-arteries/)
Source-Medindia
 MEDINDIA
MEDINDIA




 Email
Email